Abstract
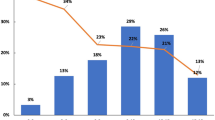
Microbiologic studies are routinely performed in the assessment of peritonsillar abscess (PTA). Though the bacterial growth rates of PTA are expected to be uniform due to high accessibility and reasonable sterility, they demonstrate a vast range of results, which is partially explained by the differing culturing methods and incubation times. Our aim was to retrospectively examine the changing features identified in the occurrence of PTA bacterial growth rates over a period of seven years. A retrospective study was undertaken on all cases of PTA admitted from January 1996 to December 2002. Details regarding sex, age and country of birth were obtained. Population data and the maximum residue level (MRL) of antibiotics in food were collected. Bacteriologic studies were analysed for gram stain, aerobic and anaerobic culture results, and also antibiotic sensitivities, if obtained. Four hundred and fifty-seven consecutive hospitalisations due to PTA were identified; 281 patients who had 310 hospitalisations with known results of the microbiologic studies were included. The most common pathogens were Streptococcus pyogenes and Prevotella. A statistically significant escalation was seen in the anaerobic growth rate from 6.8% of cases in 1996 to 37% in 1999. A similar change, though not significant, was noticed with the polymicrobial growth rate. None of the parameters investigated showed any statistically significant influence on this tendency. These results may clarify the immense range of bacterial study results reported, suggest a change in the biologic behaviour of the studied bacteria and direct further research.





Similar content being viewed by others
References
Schechter GL, Sly DE, Roper AL, Jackson RT (1982) Changing face of treatment of peritonsillar abscess. Laryngoscope 92:657–659
Brook IE, Frazier H, Thompson DH (1991) Aerobic and anaerobic microbiology of peritonsillar abscess. Laryngoscope 101:289–292
Jousimies-Somer H, Savolainen S, Mäkitie A, Ylikoski J (1993) Bacteriologic findings in peritonsillar abscesses in young adults. Clin Infect Dis 16:S292–S298
Mitchelmore IJ, Prior AJ, Montgomery PQ, Tabaqchali S (1995) Microbiological features and pathogenesis of peritonsillar abscesses. Eur J Clin Microbiol Infect Dis 14:870–877 doi:10.1007/BF01691493
Ophir D, Bawnik J, Poria Y, Porat M, Marshak G (1988) Peritonsillar abscess. A prospective evaluation of outpatient management by needle aspiration. Arch Otolaryngol Head Neck Surg 114:661–663
Snow DG, Campbell JB, Morgan DW (1991) The microbiology of peritonsillar sepsis. J Laryngol Otol 105:553–555
Prior A, Montgomery P, Mitchelmore I, Tabaqchali S (1995) The microbiology and antibiotic treatment of peritonsillar abscesses. Clin Otolaryngol 20:219–223 doi:10.1111/j.1365-2273.1995.tb01852.x
Herzon FS (1995) Peritonsillar abscess: incidence, current management practices, and a proposal for treatment guidelines. Laryngoscope 105:1–17
Matsuda A, Tanaka H, Kanaya T, Kamata K, Hasegawa M (2002) Peritonsillar abscess: a study of 724 cases in Japan. Ear Nose Throat J 81:384–389
Coyle MB, Morello JA, Byrd Smith P (1985) In: Lennette EH (ed) Manual of clinical microbiology, 4th edn. ASM Press, Washington, DC, pp 143–407
Beović B (2006) The issue of antimicrobial resistance in human medicine. Int J Food Microbiol 112:280–287 doi:10.1016/j.ijfoodmicro.2006.05.001
Kim WJ, Park SC (1998) Bacterial resistance to antimicrobial agents: an overview from Korea. Yonsei Med J 39:488–494
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gavriel, H., Lazarovitch, T., Pomortsev, A. et al. Variations in the microbiology of peritonsillar abscess. Eur J Clin Microbiol Infect Dis 28, 27–31 (2009). https://doi.org/10.1007/s10096-008-0583-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-008-0583-6