Abstract
Objectives
Several delivery models of palliative care are currently available: hospital-based, outpatient-based, home-based, nursing home-based, and hospice-based. Weighing the differences in costs of these delivery models helps to advise on the future direction of expanding palliative care services. The objective of this review is to identify and summarize the best available evidence in the US on cost associated with palliative care for patients diagnosed with cancer.
Methods
The systematic review was carried out of studies conducted in the US between 2008 and 2018, searching PubMed, Medline, the Cochrane library, CINAHL, EconLit, the Social Science Citation Index, Embase, and Science Citation Index, using the following terms: palliative, cancer, carcinoma, cost, and reimbursement.
Results
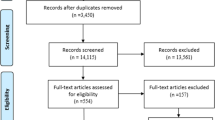
The initial search identified 748 articles, of which 16 met the inclusion criteria. Eight studies (50%) were inpatient-based, four (25%) were combined outpatient/inpatient, two (12.5%) reported only on home-based palliative services, and two (12.5%) were in multiple settings. Most included studies showed that palliative care reduced the cost of health care by $1285–$20,719 for inpatient palliative care, $1000–$5198 for outpatient and inpatient combined, $4258 for home-based, and $117–$400 per day for home/hospice, combined outpatient/inpatient palliative care.
Conclusion
Receiving palliative care after a cancer diagnosis was associated with lower costs for cancer patients, and remarkable differences exist in cost saving across different palliative care models.

Similar content being viewed by others
References
Hughes MT, Smith TJ (2014) The growth of palliative care in the United States. Annu Rev Public Health 35(1):459–475. https://doi.org/10.1146/annurev-publhealth-032013-182406
Dumanovsky T, Augustin R, Rogers M, Lettang K, Meier DE, Morrison RS (2016) The growth of palliative care in U.S. hospitals: a status report. J Palliat Med 19(1):8–15. https://doi.org/10.1089/jpm.2015.0351
Ferrell BR, Temel JS, Temin S, Alesi ER, Balboni TA, Basch EM, Firn JI, Paice JA, Peppercorn JM, Phillips T, Stovall EL. Integration of Palliative Care Into Standard Oncology Care: American Society of Clinical Oncology Clinical Practice Guideline Update. Journal of Clinical Oncology: Official Journal of the American Society of Clinical Oncology 35(1):96
Sepúlveda C, Marlin A, Yoshida T, Ullrich A 2002 Palliative care: the World Health Organization's global perspective. Journal of Pain and Symptom Management 24(2):91–6
Zimmermann C, Swami N, Krzyzanowska M, Hannon B, Leighl N, Oza A, Moore M, Rydall A, Rodin G, Tannock I, Donner A, Lo C (2014) Early palliative care for patients with advanced cancer: a cluster-randomised controlled trial. Lancet. 383(9930):1721–1730. https://doi.org/10.1016/S0140-6736(13)62416-2
Temel JS, Greer JA, Muzikansky A, Gallagher ER, Admane S, Jackson VA, Dahlin CM, Blinderman CD, Jacobsen J, Pirl WF, Billings JA, Lynch TJ (2010) Early palliative care for patients with metastatic non–small-cell lung cancer. N Engl J Med 363(8):733–742. https://doi.org/10.1056/NEJMoa1000678
Scibetta C, Kerr K, Mcguire J, Rabow MW (2016) The costs of waiting: implications of the timing of palliative care consultation among a cohort of decedents at a comprehensive cancer center. J Palliat Med 19(1):69–75. https://doi.org/10.1089/jpm.2015.0119
Colligan EM, Ewald E, Ruiz S, Spafford M, Cross-Barnet C, Parashuram S (2017) Innovative oncology care models improve end-of-life quality, reduce utilization and spending. Health Aff 36(3):433–440. https://doi.org/10.1377/hlthaff.2016.1303
Lowery WJ, Lowery AW, Barnett JC, Lopez-Acevedo M, Lee PS, Secord AA, Havrilesky L (2013) Cost-effectiveness of early palliative care intervention in recurrent platinum-resistant ovarian cancer. Gynecol Oncol 130(3):426–430. https://doi.org/10.1016/J.YGYNO.2013.06.011
Bakitas M, Lyons KD, Hegel MT, Balan S, Brokaw FC, Seville J, Hull JG, Li Z, Tosteson TD, Byock IR, Ahles TA (2009) Effects of a palliative care intervention on clinical outcomes in patients with advanced cancer. JAMA. 302(7):741–749. https://doi.org/10.1001/jama.2009.1198
Grudzen CR, Richardson LD, Johnson PN, Hu M, Wang B, Ortiz JM, Kistler EA, Chen A, Morrison RS (2016) Emergency department–initiated palliative care in advanced cancer. JAMA Oncol 2(5):591–598. https://doi.org/10.1001/jamaoncol.2015.5252
Greer JA, Tramontano AC, McMahon PM et al (2016) Cost analysis of a randomized trial of early palliative care in patients with metastatic nonsmall-cell lung cancer. J Palliat Med 19(8):842–848. https://doi.org/10.1089/jpm.2015.0476
Henk HJ, Chen C, Benedict A, Sullivan J, Teitelbaum A (2013) Retrospective claims analysis of best supportive care costs and survival in a US metastatic renal cell population. Clin Econ Outcomes Res 5:347. https://doi.org/10.2147/CEOR.S45756
Connor SR, Pyenson B, Fitch K, Spence C, Iwasaki K (2007) Comparing hospice and nonhospice patient survival among patients who die within a three-year window. J Pain Symptom Manag 33(3):238–246. https://doi.org/10.1016/J.JPAINSYMMAN.2006.10.010
May P, Garrido MM, Cassel JB, Kelley AS, Meier DE, Normand C, Smith TJ, Morrison RS (2017) Cost analysis of a prospective multi-site cohort study of palliative care consultation teams for adults with advanced cancer: where do cost-savings come from? Palliat Med 31(4):378–386. https://doi.org/10.1177/0269216317690098
May P, Garrido MM, Cassel JB, Kelley AS, Meier DE, Normand C, Stefanis L, Smith TJ, Morrison RS (2016) Palliative care teams’ cost-saving effect is larger for cancer patients with higher numbers of comorbidities. Health Aff 35(1):44–53. https://doi.org/10.1377/hlthaff.2015.0752
Gade G, Venohr I, Conner D, McGrady K, Beane J, Richardson RH, Williams MP, Liberson M, Blum M, Penna RD (2008) Impact of an inpatient palliative care team: a randomized controlled trial. J Palliat Med 11(2):180–190. https://doi.org/10.1089/jpm.2007.0055
Cassel JB, Webb-Wright J, Holmes J, Lyckholm L, Smith TJ (2010) Clinical and financial impact of a palliative care program at a small rural hospital. J Palliat Med 13(11):1339–1343. https://doi.org/10.1089/jpm.2010.0155
Ferrell BR, Temel JS, Temin S, Smith TJ (2017) Integration of palliative care into standard oncology care: ASCO clinical practice guideline update summary. J Oncol Pract 13(2):119–121
Postier A, Chrastek J, Nugent S, Osenga K, Friedrichsdorf SJ (2014) Exposure to home-based pediatric palliative and hospice care and its impact on hospital and emergency care charges at a single institution. J Palliat Med 17(2):183–188. https://doi.org/10.1089/jpm.2013.0287
May P, Normand C, Morrison RS (2014) Economic impact of hospital inpatient palliative care consultation: review of current evidence and directions for future research. J Palliat Med 17(9):1054–1063. https://doi.org/10.1089/jpm.2013.0594
Temel JS, Greer JA, Admane S, Gallagher ER, Jackson VA, Lynch TJ, Lennes IT, Dahlin CM, Pirl WF (2011) Longitudinal perceptions of prognosis and goals of therapy in patients with metastatic non-small-cell lung cancer: results of a randomized study of early palliative care. J Clin Oncol 29(17):2319–2326. https://doi.org/10.1200/JCO.2010.32.4459
Elsayem A, Swint K, Fisch MJ, Palmer JL, Reddy S, Walker P, Zhukovsky D, Knight P, Bruera E (2004) Palliative care inpatient service in a comprehensive cancer center: clinical and financial outcomes. J Clin Oncol 22(10):2008–2014. https://doi.org/10.1200/JCO.2004.11.003
Blackhall LJ, Read P, Stukenborg G, Dillon P, Barclay J, Romano A, Harrison J (2016) CARE track for advanced cancer: impact and timing of an outpatient palliative care clinic. J Palliat Med 19(1):57–63. https://doi.org/10.1089/jpm.2015.0272
Pirl W (2011) Effect of early palliative care on chemotherapy use and end-of-life care in patients with metastatic non-small-cell lung cancer addressing psychological distress in parents of children with cancer view project building resiliency in a Palliative Care Team View project. Artic J Clin Oncol 30:394–400. https://doi.org/10.1200/JCO.2011.35.7996
Ruck JM, Canner JK, Smith TJ, Johnston FM (2018) Use of inpatient palliative care by type of malignancy. J Palliat Med 21(9):1300–1307. https://doi.org/10.1089/jpm.2018.0003
May P, Garrido MM, Cassel JB, Kelley AS, Meier DE, Normand C, Smith TJ, Stefanis L, Morrison RS (2015) Prospective cohort study of hospital palliative care teams for inpatients with advanced cancer: earlier consultation is associated with larger cost-saving effect. J Clin Oncol 33(25):2745–2752. https://doi.org/10.1200/JCO.2014.60.2334
Bhulani N, Gupta A, Gao A et al (2018) Palliative care and end-of-life health care utilization in elderly patients with pancreatic cancer. J Gastrointest Oncol 9(3):495–502. https://doi.org/10.21037/jgo.2018.03.08
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151(4):264–269. https://doi.org/10.7326/0003-4819-151-4-200908180-00135
Richardson WS, Wilson MC, Nishikawa J, Hayward RS (1995) The well-built clinical question: a key to evidence-based decisions. ACP J Club 123(3). https://doi.org/10.7326/ACPJC-1995-123-3-A12
Bekelman JE, Halpern SD, Blankart CR, Bynum JP, Cohen J, Fowler R, Kaasa S, Kwietniewski L, Melberg HO, Onwuteaka-Philipsen B, Oosterveld-Vlug M, Pring A, Schreyögg J, Ulrich CM, Verne J, Wunsch H, Emanuel EJ, for the International Consortium for End-of-Life Research (ICELR) (2016) Comparison of site of death, health care utilization, and hospital expenditures for patients dying with cancer in 7 developed countries. JAMA 315(3):272–283. https://doi.org/10.1001/jama.2015.18603
Schardt C, Adams MB, Owens T, Keitz S, Fontelo P (2007) Utilization of the PICO framework to improve searching PubMed for clinical questions. BMC Med Inform Decis Mak 7. https://doi.org/10.1186/1472-6947-7-16
Smith S, Brick A, O’Hara S, Normand C (2014) Evidence on the cost and cost-effectiveness of palliative care: a literature review. Palliat Med 28(2):130–150. https://doi.org/10.1177/0269216313493466
Husereau D, Drummond M, Petrou S, Carswell C, Moher D, Greenberg D, Augustovski F, Briggs AH, Mauskopf J, Loder E, CHEERS Task Force (2013) Consolidated health economic evaluation reporting standards (cheers) statement. Int J Technol Assess Health Care 29(2):117–122. https://doi.org/10.1017/S0266462313000160
Brian Cassel J, Kerr KM, McClish DK et al (2016) Effect of a home-based palliative care program on healthcare use and costs. J Am Geriatr Soc 64(11):2288–2295. https://doi.org/10.1111/jgs.14354
Chang S, May P, Goldstein NE, Wisnivesky J, Ricks D, Fuld D, Aldridge M, Rosenzweig K, Morrison RS, Dharmarajan KV (2018) A palliative radiation oncology consult service reduces total costs during hospitalization. J Pain Symptom Manag 55(6):1452–1458. https://doi.org/10.1016/J.JPAINSYMMAN.2018.03.005
McCarthy IM, Robinson C, Huq S, Philastre M, Fine RL (2015) Cost savings from palliative care teams and guidance for a financially viable palliative care program. Health Serv Res 50(1):217–236. https://doi.org/10.1111/1475-6773.12203
Morrison RS, Penrod JD, Cassel JB, Caust-Ellenbogen M, Litke A, Spragens L, Meier DE, Palliative Care Leadership Centers' Outcomes Group (2008) Cost savings associated with US hospital palliative care consultation programs. Arch Intern Med 168(16):1783–1790. https://doi.org/10.1001/archinte.168.16.1783
Mulvey CL, Smith TJ, Gourin CG (2016) Use of inpatient palliative care services in patients with metastatic incurable head and neck cancer. Head Neck 38(3):355–363. https://doi.org/10.1002/hed.23895
Nijboer C, Triemstra M, Tempelaar R, Sanderman R, van den Bos GA (1999) Measuring both negative and positive reactions to giving care to cancer patients: psychometric qualities of the Caregiver Reaction Assessment (CRA). Soc Sci Med 48(9):1259–1269. https://doi.org/10.1016/S0277-9536(98)00426-2
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yadav, S., Heller, I.W., Schaefer, N. et al. The health care cost of palliative care for cancer patients: a systematic review. Support Care Cancer 28, 4561–4573 (2020). https://doi.org/10.1007/s00520-020-05512-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05512-y