Abstract
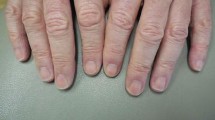
Longitudinal erythronychia is a linear red band on the nail plate that originates at the proximal nail fold, traverses the lunula, and extends to the free edge of the nail plate. Longitudinal erythronychia is classified based upon the number of nails affected and the number of red streaks present on each nail as follows: type Ia (monodactylous — single band), type Ib (monodactylous — bifid bands), type IIa (polydactylous — single band), and type IIb (polydactylous — multiple bands). Associated morphologic findings that can be present at the distal tip of the nailwith longitudinal erythronychia include fragility, onycholysis, splinter hemorrhage, splitting, subungual keratosis, thinning, and V-shaped nick. Some patients with longitudinal erythronychia seek medical evaluation because of pain in the associated distal digit; however, the linear red nail plate dyschromia is often asymptomatic and the individual is concerned about the cosmetic appearance or distal nail fragility. Longitudinal erythronychia can be a clinical manifestation of an underlying local or systemic condition. Benign tumors (glomus tumor, onychopapilloma, and warty dyskeratoma), malignant neoplasms (malignant melanoma and squamous cell carcinoma), and other conditions (hemiplegia and postsurgical scar) can be associated with monodactylous longitudinal erythronychia or it may be idiopathic or the initial stage of polydactylous longitudinal erythronychia-associated systemic conditions. Polydactylous longitudinal erythronychia ismost commonly reported in patients with Darier disease (keratosis follicularis); other associated conditions include acantholytic dyskeratotic epidermal nevus, acantholytic epidermolysis bullosa, acrokeratosis verruciformis of Hopf, amyloidosis, graft-versus-host disease, lichen planus, and pseudobulbar syndrome. Polydactylous longitudinal erythronychia has also been observed as an idiopathic finding.
Biopsy of the nail matrix and nail bed may be necessary to establish the diagnosis of a longitudinal erythronychia-associated condition. Indeed, a biopsy should be seriously considered in patients aged more than 50 years who present with a monodactylous longitudinal red band to exclude squamous cell carcinoma. Treatment of longitudinal erythronychia depends on the etiology. For patients with longitudinal erythronychia- associated discomfort or severe nail splitting, a surgical excision may provide not only the underlying diagnosis of the nail dyschromia, but also relief of related symptoms.





Similar content being viewed by others
References
Baran R. The red nail: always benign? Actas Dermosifiliogr 2009; 100 Suppl. 1: 106–13
Baran R. Red nails [abstract]. European Nail Society Meeting; 2004 Nov 17; Florence. Dermatol Online J 2005; 11 (1): 29
Cohen PR. Red lunula: case report and literature review. J Am Acad Dermatol 1992; 26: 292–4
Baran R, Dawber RPR, Richert B. Physical signs. Chapter 2. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. Osney Mead: Blackwell Science, 2001: 48–103
Cohen PR. The lunula. J Am Acad Dermatol 1996; 34: 943–53
Siragusa M, Del Gracco S, Elia M, et al. Peculiar dyschromic changes of finger nails in a patient with multiple system atrophy [letter]. Int J Dermatol 1998; 37: 156–60
Baran R, Perrin C. Longitudinal erythronychia with distal subungual keratosis: onychopapilloma of the nail bed and Bowen’s disease. Br J Dermatol 2000; 143: 132–5
Jellinek NJ. Longitudinal erythronychia: suggestions for evaluation and management. J Am Acad Dermatol 2011; 64: 167–74
de Berker DA, Perrin C, Baran R. Localized longitudinal erythronychia: diagnostic significance and physical explanation. Arch Dermatol 2004; 140: 1253–7
Baran R, Dawber RPR, Perrin C, et al. Idiopathic polydactylous longitudinal erythronychia: a newly described entity [letter]. Br J Dermatol 2006; 155: 219–21
Gee BC, Milard PR, Dawber RPR. Onychopapilloma is not a distinct clinicopathological entity [letter]. Br J Dermatol 2002; 146: 156
Harwood M, Telang GH, Robinson-Bostom L, et al. Melanoma and squamous cell carcinoma on different nails of the same hand. J Am Acad Dermatol 2008; 58: 323–6
Abimelec P, Dumontier C. Basic and advanced nail surgery: part 2. Indications and complications. Chapter 24. In: Scher RK, Daniel III CR, editors. Nails: diagnosis, therapy, surgery. 3rd ed. Philadelphia (PA): Elsevier Saunders, 2005: 291–308
Baran R, Haneke E, Drape J-L, et al. Tumours of the nail apparatus and adjacent tissues. Chapter 11. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. Osney Mead: Blackwell Science, 2001: 515–630
Baran R, Perrin C. Localized multinucleate distal subungual keratosis. Br J Dermatol 1995; 133: 77–82
Higashi N. Focal acantholytic dyskeratosis. Hifu 1990; 32: 507–10
Baran R, Perrin C. Focal subungual warty dyskeratoma. Dermatology 1997; 195: 278–80
Cogrel O, Beylot-Barry M, Doutre MS. Subungual squamous cell carcinoma revealed by longitudinal erythronychia. Ann Dermatol Venereol 2008; 135: 883–5
Reuter G, Keller F, Samama B, et al. Maladie de Bowen ungueale a type d’erythronychie longitudinale: aspect dermoscopique et etude virologique. Ann Dermatol Venereol 2005; 132: 569
Dalle S, Depape L, Phan A, et al. Squamous cell carcinoma of the nail apparatus: clinicopathological study of 35 cases. Br J Dermatol 2007; 156: 871–4
Siragusa M, Schepis C, Palazzo R, et al. Skin pathology findings in a cohort of 1500 adult and elderly subjects. Int J Dermatol 1999; 38: 361–6
Siragusa M, Schepis C, Cosentino FI, et al. Nail pathology in patients with hemiplegia. Br J Dermatol 2001; 144: 557–60
Munro CS, Cox NH. An acantholytic dyskeratotic epidermal naevus with other features of Darier’s disease on the same side of the body. Br J Dermatol 1992; 127: 168–71
Cambiaghi S, Brusasco A, Grimalt R, et al. Acantholytic dyskeratotic epidermal nevus as a mosaic form of Darier’s diease. J Am Acad Dermatol 1995; 32: 284–6
Venencie PY, Dallot A. Acantholytic dyskeratotic epidermal nevus: a mosaic form of Darier’s disease? Ann Dermatol Venereol 1999; 126: 829–30
Hoffman MD, Fleming MG, Pearson RW. Acantholytic epidermolysis bullosa. Arch Dermatol 1995; 131: 586–9
Dhitavat J, Macfarlane S, Dode L, et al. Acrokeratosis verruciformis of Hopf is caused by mutation in ATP2A2: evidence that it is allelic to Darier’s disease. J Invest Dermatol 2003; 120: 229–32
Juhlin L, Baran R. Hereditary and congenital nail disorders. Chapter 9. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. Osney Mead: Blackwell Science, 2001: 370–424
Berk DR, Taube JM, Bruckner AL, et al. A sporadic patient with acrokeratosis verruciformis of Hopf and a novel ATP2A2 mutation [letter]. Br J Dermatol 2010 Sep; 163 (3): 653–4
Rallis E, Economidi A, Papadakis P, et al. Acrokeratosis verruciformis of Hopf (Hopf disease): case report and review of the literature. Dermatol Online J 2005; 11 (2): 10
Tosti A, Baran R, Dawber RPR. The nail in systemic diseases and druginduced changes. Chapter 6. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. Osney Mead: Blackwell Science, 2001: 223–329
Mancuso G, Fanti PA, Berdondine RM. Nail changes as the only skin abnormality inmyeloma-associated systemic amyloidosis [letter]. Br JDermatol 1997; 137: 471–2
Cholez C, Cuny J-F, Pouaha J, et al. Nail abnormalities and scleroderma-like lesions on the face associated with systemic amyloidosis. Ann Dermatol Venereol 2005; 132: 252–4
Derrick EK, Price ML. Primary systemic amyloid with nail dystrophy. J R Soc Med 1995; 88: 290P–1P
Prat C, Moreno A, Vinas M, et al. Nail dystrophy in primary systemic amyloidosis [letter]. J Eur Acad Dermatol Venereol 2008; 22: 107–9
Desirello G, Nazzari G, Stradini D, et al. Primary amyloidosis. G Ital Dermatol Venereol 1988; 123: 99–101
Sanli H, Arat M, Oskay T, et al. Evaluation of nail involvement in patients with chronic cutaneous graft versus host disease: a single-center study from Turkey. Int J Dermatol 2004; 43: 176–80
Palencia SI, Rodriguez-Peralto JL, Castano E, et al. Lichenoid nail changes as sole external manifestation of graft vs. host disease. Int J Dermatol 2002; 41: 44–5
Liddle BJ, Cowan MA. Lichen planus-like eruption and nail changes in a patient with graft-versus-host disease [letter]. Br J Dermatol 1990; 122: 841–3
de Berker DAR, Baran R, Dawber RPR. The nail in dermatological diseases. Chapter 5. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. Osney Mead: Blackwell Science, 2001: 172–222
Siragusa M, Del Gracco S, Ferri R, et al. Longitudinal red streaks on the big toenails in a patient with pseudobulbar syndrome [letter]. J Eur Acad Dermatol Venereol 2001; 15: 85–6
Van Geertruyden J, Lorea P, Goldschmidt D, et al. Glomus tumours of the hand: a retrospective study of 51 cases. J Hand Surg Br 1998; 21: 257–60
Moon SE, Won JH, Kwon OS, et al. Subungual glomus tumor: clinical manifestations and outcome of surgical treatment. J Dermatol 2004; 31: 993–7
Lee LJ, Park DH, Park MC, et al. Subungual glomus tumours of the hand: diagnosis and outcome of the transungual approach. J Hand Surg Eur 2009; 34E: 685–8
Okada O, Demitsu T, Manabe M, et al. A case of multiple subungual glomus tumors associated with neurofibromatosis type 1. J Dermatol 1999; 26: 535–7
De Smet L, Sciot R, Legius E. Multifocal glomus tumours of the fingers in two patients with neurofibromatosis type 1. J Med Genet 2002; 39: e45
Kohout E, Stour AP. The glomus tumor in children. Cancer 1961; 14: 555–6
Parsons ME, Russo G, Fucich L, et al. Multiple glomus tumor. Int J Dermatol 1997; 36: 894–900
Ekin A, Ozkan M, Kabaklioglu T. Subungual glomus tumours: a different approach to diagnosis and treatment. J Hand Surg Br 1977; 22: 228–9
Matsunaga A, Ochiai T, Abe I, et al. Subungual flomus tumour: evaluation of ultrasound imaging in preoperative assessment. Eur JDermatol 2007; 17: 67–9
Fujioka H, Kokubu T, Akisue T, et al. Treatment of subungual glomus tumor. Kobe J Med Sci 2009; 55: E1–4
Takata H, Ikuta Y, Ishida O, et al. Treatment of subungual glomus tumour. Hand Surg 2001; 8: 25–7
Richert B, Iorizzo M, Tosti A, et al. Nail bed lichen planus associated with onychopapilloma [letter]. Br J Dermatol 2007; 156: 1071–2
Criscione V, Telang G, Jellinek NJ. Onychopapilloma presenting as longitudinal leukonychia [letter]. J Am Acad Dermatol 2010; 63: 541–2
Meesiri S. Subungual squamous cell carcinoma masquerading as chronic common infection. J Med Assoc Thai 2010; 93: 248–51
Robinette JW, Day 3rd F, Hahn Jr P. Subungual squamous cell carcinoma mistaken for a verruca [letter]. J Am Podiatr Med Assoc 1999; 89: 435–7
Oon HH, Kumarasinghe SPW. Subungual squamous cell carcinoma masquerading as a melanotic macule. Singapore Med J 2008; 49: e76–7
Saijo S, Kato T, Tagami H. Pigmented nail streak associated with Bowen’s disease of the nail matrix. Dermatologica 1990; 181: 156–8
Telfer NR, Burge SM, Ryan TJ. Vesiculo-bullous Darier’s disease. Br J Dermatol 1990; 122: 831–4
Cohen PR. Nonimmunologic acantholytic diseases. Chapter 11. In: Jordon RE, editor. Atlas of bullous diseases. New York (NY): Churchill Livingstone, 2000: 213–25
Cooper SM, Burge SM. Darier’s disease: epidemiology, pathophysiology, and management. Am J Clin Dermatol 2003; 4: 97–105
Cohen PR. Darier disease: sustained improvement following reduction mammaplasty. Cutis 2003; 72: 124–6
Acknowledgments
No sources of funding were used to prepare this review. The author has no conflicts of interest that are directly relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cohen, P.R. Longitudinal Erythronychia. Am J Clin Dermatol 12, 217–231 (2011). https://doi.org/10.2165/11586910-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11586910-000000000-00000