Abstract
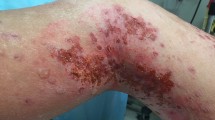
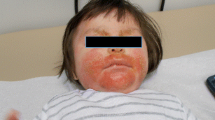
Clinicians have long since been aware that bacteria and other microorganisms play a role in the etiology of atopic dermatitis. Indeed, the immunological profile of atopy favors colonization by Staphylococcus aureus, and the bacteria are present in most patients with atopic dermatitis, even in the absence of skin lesions. Clinical signs of impetiginization, such as weeping and crusting, periauricular fissuration, or small superficial pustules are a sensitive indicator that the numbers of S. aureus may have increased and a clinical indication of secondary infected dermatitis. However, recent research that has focussed on the role of S. aureus in atopic dermatitis, offers a reversed perspective, by presenting evidence that the underlying pathology of atopic dermatitis, i.e. an alteration of the skin barrier and inflammation of the upper dermis, depends itself on the presence of an infectious process. In other words, secondary infection with S. aureus emerges as a cause of atopic dermatitis. Secondary infections due to fungi have, comparatively, received less attention, but there is evidence for a role for Malassezia spp. as a factor in dermatitis with a head and neck distribution pattern. Viral infections, such as herpes simplex virus, and mixed infections of intertriginous spaces, may complicate an underlying atopic dermatitis, but are not perceived as etiologic factors.
Recent research has greatly contributed to our understanding of the pathophysiological potential of S. aureus superantigens in atopic dermatitis, suggesting that antibiotic therapy might be an important element in the therapeutic management of atopic dermatitis. At present, however, the clinical evidence is scarce with regards to demonstrating a clear advantage of combined anti-inflammatory and antibiotic treatment, compared with anti-inflammatory treatment alone. If there is a consensus that the presence of clinically infected lesions in atopic dermatitis warrants a course of specific antibiotic topical therapy, the clinical benefit of antibiotic agents in apparently uninfected atopic dermatitis, as present in the majority of patients, remains an open question.
Moreover, the impact of adjuvant skin care on the cutaneous microflora needs to be quantified in order to properly assess the role of specific antibiotic therapy in clinically uninfected atopic dermatitis. In the meantime, secondary infections in atopic dermatitis remain a secondary problem in clinical atopic dermatitis management, and specific anti-infective therapy remains a method of fine-tuning for optimizing individual atopic dermatitis treatment.








Similar content being viewed by others
Notes
The use of tradenames is for product identification purposes only and does not imply endorsement.
References
Saurat JH. Principes de traitement du syndrome eczéma. In: Saurat JH, Grosshaus E, Laugier P et al., editors. Dermatologie et maladies sexuellement transmissibles. Paris: Masson, 1999: 35
Storck H. Experimentelle Untersuchung zur Frage der Bedeutung von Mikroben in der Ekzemgenese. Dermatologica Helvetica 1948; 96: 177–262
Bockhart M. Untersuchungen über die parasitäre Natur des Ekzems und über das Staphylotoxin-Ekzem. Monatsh f prakt Derm 1901; 33 (9): 421–36
Andersen E, Heilesen B. On the occurrence of staphylococcus pyogenes in weeping eczema (and the role played by these bacteria in the pathogenesis and course of eczema). Acta Derm Venereol 1951; 31: 679–703
Marples M. The ecology of the human skin. Springfield (IL): Charles C. Thomas, 1965
Williamson P, Kligman A. A new method for quantitative investigation of cutaneous bacteria. J Invest Dermatol 1965; 45: 498–503
Leyden J, Marples R, Kligman A. Staphylococcus aureus in the lesions of atopic dermatitis. Br J Dermatol 1974; 90: 525–30
Lever R, Hadley K, Downey D, et al. Staphylococcal colonization in atopic dermatitis and the effect of topical mupirocin therapy. Br J Dermatol 1988; 119: 189–98
Leung D. Atopic dermatitis: new insights and opportunities for therapeutic intervention. J Allergy Clin Immunol 2000; 105: 860–76
Roth R, James W. Microbiology of the skin: resident flora, ecology, infection. J Am Acad Dermatol 1989; 20: 367–90
Noble W, Sommerville D. The streptococci, in major problems in dermatology. London: WB Saunders, 1974: 160–171
Bibel D, Lovell D. Skin flora maps: a tool in the study of cutaneous ecology. J Invest Dermatol 1976; 67 (2): 265–9
Kligman A, Leyden J, McGinley K. Bacteriology. J Invest Dermatol 1976; 67: 160–8
Noble W, Sommerville D. The micrococcaceae. In: Noble W, Sommerville D, editors. Microbiology of human skin. London: WB Saunders, 1974: 125
Williams R, Gibson A, Aitchison T. Assessment of a contact-plate sampling technique and subsequent bacterial studies in atopic dermatitis. Br J Dermatol 1990; 123: 493–501
Aly R, Maibach HI. Aerobic microbial flora of intertriginous skin. Appl Environ Microbiol 1977; 33: 97–100
Jappe U, Heuck D, Witte W, et al. Superantigen production by staphylococcus aureus in atopic dermatitis: no more than a coincidence? J Invest Dermatol 1998; 110 (5): 844–6
Barth J. Nasal carriage of saphylococci and streptococci. Int J Dermatol 1987; 26: 24–6
Aly R, Maibach HI, Shinefield H. Microbial flora of atopic dermatitis. Arch Dermatol 1977; 113: 780–2
Nishijima S, Namura S, Kawai S, et al. Staphylococcus aureus on hand surface and nasal carriage in patients with atopic dermatitis. J Am Acad Dermatol 1995; 32: 677–9
Hauser C, Wuethrich B, Matter L. Staphylococcus aureus skin colonization in atopic dermatitis. Dermatologica Helvetica 1985; 170: 35
Goodyear HM, Watson PJ, Egan SA, et al. Skin microflora of atopic eczema in first time hospital attenders. Clin Exp Dermatol 1993; 18: 300–4
Ewing C, Ashcroft C, Gibbs A. Flucloxacillin in the treatment of atopic dermatitis. Br J Dermatol 1998; 138: 1022–9
Matsui K, Nishikawa A, Suto H, et al. Comparative study of staphylococcus aureus isolated from lesional and non-lesional skin of atopic dermatitis patients. Microbiol Immunol 2000; 44: 945–7
Nilsson E, Henning C, Magnusson J. Topical corticosteroids and staphylococcus aureus in atopic dermatitis. J Am Acad Dermatol 1992; 27: 29–34
Nilsson E, Henning C, Hjörleifson ML. Density of the microflora in hand eczema before and after topical treatment with a potent corticosteroid. J Am Acad Dermatol 1986; 15: 192–7
Saloga J, Gelfand E, Knop J. Superantigens. Exp Dermatol 1996; 5: 65–71
Michie C, Davis T. Atopic dermatitis and staphylococcal superantigens [letter]. Lancet 1996; 347: 324
Strange P, Skov L, Lisby S, et al. Staphylococcal enterotoxin B applied on intact normal and intact atopic skin induces dermatitis. Arch Dermatol 1996; 132: 27–33
Strickland I, Hauk P, Trumble A, et al. Evidence for superantigen involvement in skin homing of T-cells in atopic dermatitis. J Invest Dermatol 1999; 112: 249–53
Akiyama H, Toi Y, Kanzaki H, et al. Prevalence of producers of exotoxins and toxic shock syndrome toxin-1 among Staphylococcus aureus strains isolated from atopic dermatitis lesions. Arch Dermatol Res 1996; 288: 418–20
Bunikowski R, Mielke M, Skarabis H, et al. Evidence for a disease-promoting effect of staphylococcus aureus-derived exotoxins in atopic dermatitis. J Allergy Clin Immunol 2000; 105: 814–9
Zollner T, Wichelhaus T, Hartung A, et al. Colonization with superantigen-producing staphylococcus aureus is associated with increased severity of atopic dermatitis. Clin Exp Allergy 2000; 30: 994–1000
Zollner T, Kaufmann R. Superantigens in T-cell mediated skin diseases: more than a coincidence. J Invest Dermatol 1999; 112 (1): 118–9
Nomura I, Tanaka K, Tomita H, et al. Evaluation of the staphylococcal exotoxins and their specific IgE in childhood atopic dermatitis. J Allergy Clin Immunol 1999; 104: 441–6
Leung D, Harbeck R, Bina P, et al. Presence of IgE antibodies to staphylococcal exotoxins on the skin of patients with atopic dermatitis: evidence for a new group of allergens. J Clin Invest 1993; 92 (3): 1374–80
Bunikowski R, Mielke M, Skarabis H, et al. Prevalence and role of serum IgE antibodies to the staphylococcus aureus-derived superantigens SEA and SEB in children with atopic dermatitis. J Allergy Clin Immunol 1999; 103: 119–24
Tada J, Toi Y, Akiyama H, et al. Presence of specific IgE antibodies to staphylococcal enterotoxins in patients with atopic dermatitis. Eur J Dermatol 1996; 6: 552–4
Hauk P, Leung D. Tacrolimus (FK506): new treatment approach in superantigen-associated diseases like atopic dermatitis? J Allergy Clin Immunol 2001; 107 (2): 391–2
Stalder J, Fleury M, Sourisse M. Local steroid therapy and bacterial skin flora in atopic dermatitis. Br J Dermatol 1994; 131: 536–40
Brockow K, Grabenhorst P, Abeck D, et al. Effect of gentian violet, corticosteroid and tar preparations in staphylococus aureus-colonized eczema. Dermatology 1999; 199: 231–6
Cho SH, Strickland I, Tomkinson A, et al. Preferential binding of staphylococcus aureus to skin sites of Th2-mediated inflammation in a murine model. J Invest Dermatol 2001; 116: 658–63
Cho SH, Strickland I, Boguniewicz M, et al. Fibronectin and fibrinogen contribute to the enhanced binding of staphylococcus aureus to atopic skin. J Allergy Clin Immunol 2001; 108: 269–74
Lübbe J. Evidence-based corneotherapy. Dermatology 2000; 200: 285–6
Cork M. The importance of skin barrier function. J Dermatol Treat 1997; 8: S7-S13
Akiyama H, Huh WK, Fujii K, et al. Confocal laser microscopic observation of glycocalix production by staphylococcus aureus in vitro. J Dermatol Sci 2002; 29: 54–61
Ong PY, Ohtake T, Brandt C, et al. Endogenous antimicrobial peptides and skin infections in atopic dermatitis. N Engl J Med 2002; 347: 1151–60
David T, Cambridge G. Bacterial infection and atopic eczema. Arch Dis Child 1986; 61: 20–3
Kim K, Hwang J, Park K. Periauricular eczematization in childhood atopic dermatitis. Pediatr Dermatol 1996; 13 (4): 278–80
Hanifin J, Rogge J. Staphylococcal infections in patients with atopic dermatitis. Arch Dermatol 1977; 113: 1383–6
Leyden J, Kligman A. The case for steroid-antibiotic combinations. Br J Dermatol 1977; 96: 179–87
Brown EM, Thomas P. Fusidic acid resistance in Staphylococcus aureus isolates [letter]. Lancet 2002; 359: 803
Shah M, Mohanraj M. High levels of fusidic acid resistant Staphylococcus aureus in dermatology patients. Br J Dermatol 2003; 148: 1018–20
Martinez F, Holt P. Role of microbial burden in aetiology of allergy and asthma. Lancet 1999; 354 Suppl. II: 12–5
Droste J, Wieringa M, Weyler J, et al. Does the use of antibiotics in early childhood increase the risk of asthma and allergic disease? Clin Exp Allergy 2000; 30: 1547–53
Wills-Karp M, Santeliz J, Karp C. The germless theory of allergic disease: revisiting the hygiene hypothesis. Nat Rev Immunol 2001; 1: 69–75
Pournaras CC, Lübbe J, Saurat JH. Staphylococcal colonization in atopic dermatitis treatment with topical tacrolimus (Fk506). J Invest Dermatol 2001; 116: 480–1
Remitz A, Kyllönen H, Granlund H, et al. Tacrolimus ointment reduces staphylococcal colonization of atopic dermatitis lesions. J Allergy Clin Immunol 2001; 107 (1): 196–7
Wachs G, Maibach HI. Cooperative double-blind trial of an antibiotic/corticoid combination in impetiginized atopic dermatitis. Br J Dermatol 1976; 95: 323–8
Hjorth N, Schmidt H, Thomsen K. Fusidic acid plus betamethasone in infected or potentially infected eczema. Pharmatherapeutica 1985; 4 (2): 126–31
Emerson R, Williams H, Allen B. Severity distribution of atopic dermatitis in the community and its relationship to secondary referral. Br J Dermatol 1998; 139: 73–6
Polano M, De Vries H. Analysis of the results obtained in the treatment of atopic dermatitis with corticosteroid and neomycin containing ointments. Dermatologica 1960; 120: 191–9
Ramsay C, Savoie C, Gilbert M. The treatment of atopic dermatitis with topical fusidic acid and hydrocortisone acetate. J Eur Acad Dermatol Venereol 1996; 7 Suppl.: S15–22
Sasai-Takedatsu M, Kojima T, Yamamoto A, et al. Reduction of staphylococcus aureus in atopic skin lesions with acid electrolytic water: a new therapeutic strategy for atopic dermatitis. Allergy 1997; 52: 1012–6
Valenta C, Bernkopf-Schnürch A, Rigler H. The antistaphylococcal effect of nisin in a suitable vehicle: a potential therapy for atopic dermatitis in man. J Pharm Pharmacol 1996; 48 (9): 988–91
Stalder J, Fleury M, Sourisse M, et al. Comparative effects of two topical antiseptics (chlorhexidine vs KMnO4) on bacterial skin flora in atopic dermatitis. Acta Derm Venereol (Stockh) Suppl 1992; 176: 132–4
Thestrup-Pedersen C. Treatment principles of atopic dermatitis. J Eur Acad Dermatol Venereol 2002; 16: 1–9
Akiyama H, Tada J, Toi Y, et al. Changes in staphylococcus aureus density and lesion severity after topical application of povidone-iodine in cases of atopic dermatitis. J Dermatol Sci 1997; 16: 23–30
Gehring W, Forssmann T, Gloor M. Die keimreduzierende Wirkung von Erythromycin und Triclosan bei der atopischen Dermatitis. Akt Dermatol 1996; 22: 28–31
Yoshimura M, Namura S, Akamatsu H, et al. Antimicrobial effects of phototherapy and photochemotherapy in vivo and in vitro. Br J Dermatol 1996; 135: 528–35
Schempp C, Effinger T, Czech W, et al. Charakterisierung von non-Respondern bei der hochdosierten UVA1-Therapie der akut exazerbierten atopischen Dermatitis. Hautarzt 1997; 48: 94–9
Akiyama H, Yamasaki O, Kanzaki H, et al. Effects of zinc oxide on the attachment of Staphylococcus aureus strains. J Dermatol Sci 1998; 17: 67–74
Akiyama H, Fujii K, Yamasaki O, et al. Antibacterial action of several tannins against Staphylococcus aureus. J Antimicrob Chemother 2001; 48: 487–91
Akiyama H, Oono T, Huh WK, et al. Actions of farnesol and xylitol against Staphylococcus aureus. Chemotherapy 2002; 48: 122–8
Nizet V, Ohtake T, Lauth X, et al. Innate antimicrobial peptide protects the skin from invasive bacterial infection. Nature 2001; 414: 454–7
Ganz T, Lehrer R. Antibiotic peptides from higher eukaryotes: biology and applications. Mol Med Today 1999; 5: 292–7
Abeck D, Mempel M. Staphylococcus aureus colonization in atopic dermatitis and its therapeutic implications. Br J Dermatol 1998; 139 Suppl. 53: 13–6
Wilkinson J. Fusidic acid in dermatology. Br J Dermatol 1998; 139 Suppl. 53: 37–40
Cork M. The role of staphylococcus aureus in atopic eczema: treatment strategies. J Eur Acad Dermatol Venereol 1996; 7 Suppl. 1: S31–7
Leung D, Hauk P, Strickland I, et al. The role of superantigens in human disease: therapeutic implications for the treatment of skin diseases. Br J Dermatol 1998; 139 Suppl. 53: 17–29
Hanifin J. Staphylococcal colonization, infection, and atopic dermatitis: association not etiology. J Allergy Clin Immunol 1986; 78 (4): 563–6
Thestrup-Pedersen C. Bacteria and the skin: clinical practice and therapy update. Br J Dermatol 1998; 139: 1–3
Lever R. Infection in atopic dermatitis. Dermatol Ther 1996; 1: 32–7
Adachi J, Endo K, Fukuzumi T, et al. Increasing incidence of streptococcal impetigo in atopic dermatitis. J Dermatol Sci 1998; 17 (1): 45–53
Veien N. The clinician’s choice of antibiotics in the treatment of bacterial skin infection. Br J Dermatol 1998; 139 Suppl. 53: 30–6
Strannegard O, Strannegard I. Changes in cell-mediated immunity in atopic eczema. In: Ruzicka T, Ring J, Pryzbilla B, editors. Handbook of atopic eczema. Berlin: Springer Verlag, 1991: 221–231
Leyden J, Baker D. Localized herpes simplex infections in atopic dermatitis. Arch Dermatol 1979; 115: 311–2
Bork K, Bräuninger W. Increasing incidence of eczema herpeticum: analysis of seventy-five cases. J Am Acad Dermatol 1988; 19: 1024–9
Yoshida M, Amatsu A. Asymptomatic shedding of herpes simplex virus into the oral cavity of patients with atopic dermatitis. J Clin Virol 2000; 16 (1): 65–9
Wollenberg A, Zoch C, Wetzel S, et al. Predisposing factors and clincal features of eczema herpeticum: a retrospective analysis of 100 cases [online]. J Am Acad Dermatol 2003; 49. Available from URL:
Amatsu A, Yoshida M. Detection of herpes simplex virus DNA in non-herpetic areas of patients with eczema herpeticum. Dermatology 2000; 200: 104–7
Brook I, Frazier E, Yeager J. Microbiology of infected eczema herpeticatum. J Am Acad Dermatol 1998; 38 (4): 627–9
Lübbe J, Pournaras CC, Saurat JH. Eczema herpeticum during treatment of atopic dermatitis with 0.1% tacrolimus ointment. Dermatology 2000; 201: 249–51
Lübbe J. Topical tacrolimus for atopic dermatitis: euphoria and vigilance. Dermatology 2001; 203 (1): 32–7
Lübbe J. Herpes simplex history, serology, and symptomatic infection in patients treated with topical tacrolimus for atopic dermatitis [abstract]. J Invest Dermatol 2002; 119 (3): 760
Lübbe J, Sanchez-Politta S, Tschanz C, et al. Adults with atopic dermatitis, herpes simplex, and topical therapy with tacrolimus: what kind of prevention? Arch Dermatol 2003; 139 (5): 670–1
Lacour M, Hauser C. The role of microorganisms in atopic dermatitis. Clin Rev Allergy 1993; 11: 491–522
Hanifin J, Ray L, Lobitz W. Immunological reactivity in dermatophytosis. Br J Dermatol 1974; 90: 213–20
Scheynius A, Johansson C, Buentke E, et al. Atopic eczema/dermatitis syndrome and maassezia. Int Arch Allergy Immunol 2002; 127: 161–9
Faergemann J. Pityrosporum species as a cause of allergy and infection. Allergy 1999; 54: 413–9
Broberg A, Faergemann J. Topical antimycotic treatment of atopic dermatitis in the head/neck area. Acta Derm Venereol (Stockh) 1995; 75: 46–9
Bäck O, Bartosik J. Systemic ketoconazole for yeast allergic patients with atopic dermatitis. J Eur Acad Dermatol Venereol 2001; 15: 34–8
Hjorth N, Clemensson O. Treatment of dermatitis of the head and neck with ketoconazole in patients with type I hypersensitivity for Pityrosporum orbiculare. Semin Dermatol 1983; 2: 26–9
Bäck O, Scheynius A, Johansson S. Ketoconazole in atopic dermatitis: therapeutic response is correlated with with decrease in serum IgE. Arch Dermatol Res 1995; 287: 448–51
Morita E, Hide M, Yonega Y, et al. An assessment of the role of candida albicans in atopic dermatitis. J Dermatol 1999; 26: 282–7
Kolmer H, Taketomi E, Hazen K, et al. Effect of combined antibacterial and antifungal treatment in severe atopic dermatitis. J Allergy Clin Immunol 1996; 98: 702–7
Gumowski P, Lech B, Chaves I, et al. Chronic asthma and rhinitis due to candida albicans, epidermophyton, and trichophyton. Ann Allergy 1987; 59 (1): 48–1
Ward G, Woodfolk J, Hayden M, et al. Treatment of late-onset asthma with fluconazole. J Allergy Clin Immunol 1999; 104: 541–6
Jones H, Reinhardt J, Rinaldi M. Immunologic susceptibility to chronic dermatophytosis. Arch Dermatol 1974; 110: 213–20
Svejgaard E, Christophersen J, Jelsdorf HM. Tinea pedis and erythrasma in Danish patients. J Am Acad Dermatol 1986; 14 (6): 993–9
Wilson B, Deuell B, Mills T. Atopic dermatitis associated with dermatophyte infection and trichophyton hypersensitivity. Cutis 1993; 51: 191–2
Hürlimann A, Fäh J. Asthma, rhinitis and dermatitis triggered by fungal infection: therapeutic effects of terbinafine. Dermatology 2001; 202 (4): 330–2
Schwanitz H. Atopic palmoplantar eczema. Heidelberg: Springer Verlag, 1988
Goldman L. Dental floss as a factor in the development of perlèche [letter]. Arch Dermatol 1979; 115 (1): 108
Laymon C. Treatment of perlèche. JAMA 1969; 207 (5): 959–60
Leyden J, Kligman A. Interdigital athlete’s foot. Arch Dermatol 1978; 114: 1466–72
Amonette R, Rosenberg E. Infection of the toe webs by gram-negative bacteria. Arch Dermatol 1973; 107: 71–3
Eaglestein N, Marley W, Marley N, et al. Gram-negative bacterial toe web infection: successful treatment with a new third generation cephalosporin. J Am Acad Dermatol 1983; 8: 225–8
Acknowledgements
The author has provided no information on sources of funding or on conflicts of interest directly relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lübbe, J. Secondary Infections in Patients with Atopic Dermatitis. Am J Clin Dermatol 4, 641–654 (2003). https://doi.org/10.2165/00128071-200304090-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00128071-200304090-00006