Abstract
Background: Surgical resection of colorectal liver metastases (CLM) is the only hope for cure, with a 5-year survival rate ranging from 20% to 54%. However, the resectability rate of CLM is reported to be <20%. This limitation is mainly due to insufficient remnant liver and to extrahepatic disease. Among extrahepatic locations, lymph node metastases are often considered indications of a very poor prognosis and a contra-indication to resection.
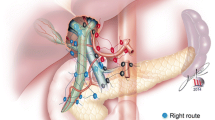
Methods and Results: Our studies showed that the prevalence of hepatic pedicle lymph node metastases ranges from 10% to 20%. When located near the hilum and along the hepatic pedicle (area 1) they should not be considered an absolute contra-indication to resection of CLM, and an extended lymphadenectomy should be performed. However, when they reach the celiac trunk (area 2), there is no survival benefit after resection of CLM. For other cases of liver malignancies, lymph node dissection seems justified only in cases of fibrolamellar hepatocellular carcinoma and in case of hilar cholangiocarcinoma. However, few data are available, and they are controversial.
Conclusions: There is a need for more evaluation of lymph node involvement, at least in patients with high risk of such an extension, i.e., patients with more than three metastases, located in segment 4 or 5. There is also a need for prospective trials in order to evaluate the survival benefit of liver resection in such circumstances and the impact of extensive lymphadenectomy.
Similar content being viewed by others
REFERENCES
Hughes KS, Simon R, Songhorabodi S, et al. Resection of the liver for colorectal carcinoma metastases: a multi-institutional study of patterns of recurrence. Surgery 1996;100:278–84.
Nordlinger B, Jaeck D, Guiguet M, et al. Surgical resection of hepatic metastases: multicentric retrospective study by the French Association of Surgery Nordlinger B, Jaeck D Eds. Treatment of Hepatic Metastases of Colorectal Cancer. Paris:: Springer-Verlag, 1992: 129–46.
Nakamura S, Yokoi Y, Suzuki S, et al. Results of extensive surgery for liver metastases in colorectal carcinoma. Br J Surg 1992;79:35–8.
Scheele J, Stangl R, Altendorf-Hofmann A, et al. Resection of colorectal liver metastases. World J Surg 1995;19:59–71.
Jaeck D, Bachellier PH, Guiget M, et al. Long-term survival following resection of colorectal hepatic metastases. Br J Surg 1997;84:977–80.
Iwatsuki S, Dvorchik I, Madariaga JR, et al. Hepatic resection for metastatic colorectal adenocarcinoma: a proposal of prognostic scoring system. J Am Coll Surg 1999;189:291–9.
Fong Y, Fortner J, Sun RL, et al. Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: analysis of 1001 consecutive cases. Ann Surg 1999;230:309–21.
Rougier P, Milan C, Lazorthes F, et al. Prospective study of prognostic factors in patients with unresected hepatic metastases from colorectal cancer. Br J Surg 1995;82:1397–400.
Bismuth H, Adam R, Levi F, et al. Resection of nonresectable liver metastasis from colorectal cancer after neoadjuvant chemotherapy. Ann Surg 1996;224:509–22.
Elias D, Lasser P, Rougier P, et al. Frequency, technical aspects, results and indications of major hepatectomy after prolonged intra-arterial hepatic chemotherapy for initially unresectable hepatic tumors. J Am Coll Surg 1995;180:213–9.
Minagawa M, Makuuchi M, Torzilli G, et al. Extension of the frontiers of surgical indications in the treatment of liver metastases from colorectal cancer: long-term results. Ann Surg 2000;231:487–99.
Azoulay D, Casting D, Smail A, et al. Resection of nonresectable liver metastases from colorectal cancer after percutaneous portal vein embolization. Ann Surg 2000;231:480–6.
Elias D, Ouellet JF, de Baère T, et al. Preoperative selective portal vein embolization before hepatectomy for liver metastases: long-term results and impact on survival. Surgery 2002;131:294–9.
Curley SA, Izzo F, Delrio P, et al. Radiofrequency ablation of unresectable primary and metastatic hepatic malignancies: results in 123 patients. Ann Surg 1999;230:1–8.
Adam R, Akpinar E, Johann M, et al. Place of cryosurgery in the treatment of malignant liver tumors. Ann Surg 1997;225:39–50.
Kokudo N, Miki Y, Sugai S, et al. Genetic and histologic assessment of surgical margins in resected liver metastases from colorectal carcinoma. Arch Surg 2002;137:833–40.
Fan ST, LO CM, Liu CL, et al. Hepatectomy for hepatocellular carcinoma: toward zero hospital deaths. Ann Surg 1999;229:322–30.
August DA, Sugarbaker PH, Schneider PD. Lymphatic dissemination of hepatic metastases: implications for the follow-up and treatment of patients with colorectal cancer. Cancer 1985;55:1490–4.
Lefor AT, Hughes KS, Shiloni E, et al. Intra-abdominal extrahepatic disease in patients with colorectal hepatic metastases. Dis Colon Rectum 1988;31:100–3.
Jaeck D, Nakano H, Bachellier P, et al. Significance of hepatic pedicle lymph node involvement in patients with colorectal liver metastases: a prospective study. Ann Surg Oncol 2002;9:430–8.
Adson MA. The resection of hepatic metastases: another view. Arch Surg 1989;124:1023–4.
Foster JH. Survival after liver resection for secondary tumors. Am J Surg 1978;135:389–94.
Pedersen IK, Burcharth F, Roikjaer O, et al. Resection of liver metastases from colorectal cancer: indications and results. Dis Colon Rectum 1994;37:1078–82.
Rodgers MS, McCall JL. Surgery for colorectal liver metastases with hepatic lymph node involvement: a systematic review. Br J Surg 2000;87:1142–55.
Beckurts KT, Holscher AH, Thorban S, et al. Significance of hepatic involvement at the hepatic hilum in the resection of colorectal liver metastases. Br J Surg 1997;84:1081–4.
Elias D, Saric J, Jaeck D, et al. Prospective study of microscopic lymph node involvement of the hepatic pedicle during curative hepatectomy for colorectal metastases. Br J Surg 1996;83:942–5.
Trutmann M, Sasse D. The lymphatics of the liver. Anat Embryol 1994;190:201–9.
Ito M, Mishima Y, Sato T. An anatomical study of the lymphatic drainage of the gallbladder. Surg Radiol Anat 1991;13:89–104.
Willis RA. The Spread of Tumors in the Human Body. London: Butterworth and Company, 1973;19:175–83.
Shirabe K, Shimada M, Harimoto N, et al. Intrahepatic cholangiocarcinoma: its mode of spreading and therapeutic modalities. Surgery 2002;131:S159–64.
Shimada M, Yamashita Y, Aishima S, et al. Value of lymph node dissection during resection of intrahepatic cholangiocarcinoma. Br J Surg 2001;88:1463–6.
Tsugi T, Hiraoka T, Kanemitsu K, et al. Lymphatic spreading pattern of intrahepatic cholangiocarcinoma. Surgery 2001;129:401–7.
Kitigawa Y, Nagino M, Kamiya J, et al. Lymph node metastasis from hilar cholangiocarcinoma: audit of 110 patients who underwent regional and paraaortic node dissection. Ann Surg 2001;233:385–92.
The Liver Cancer Study Group of Japan. Primary liver cancer in Japan: clinicopathologic features and results of surgical treatment. Ann Surg 1990;211:277–87.
Uenishi T, Hirokaski K, Tanaka H, et al. A surgically treated case of hepatocellular carcinoma with extensive lymph node metastases. Hepatogastroenterology 2000;47:1714–6.
Hiramatsu K, Okamoto K, Uesaka K, et al. Surgical management of lymph node recurrence of resected fibrolamellar hepatocellular carcinoma: a case report. Hepatogastroenterology 1999;46:1160–3.
Weber JC, Nakano H, Bachellier P, et al. Is a proliferation index of cancer cells a reliable prognostic factor after hepatectomy in patients with colorectal liver metastases? Am J Surg 2001;182:81–8.
Weber JC, Schneider A, Rohr S, et al. Analysis of allelic imbalance in patients with colorectal cancer according to stage and presence of synchronous liver metastases. Ann Surg 2001;234:795–803.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jaeck, D. The Significance of Hepatic Pedicle Lymph Nodes Metastases in Surgical Management of Colorectal Liver Metastases and of Other Liver Malignancies. Ann Surg Oncol 10, 1007–1011 (2003). https://doi.org/10.1245/ASO.2003.09.903
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1245/ASO.2003.09.903