Abstract
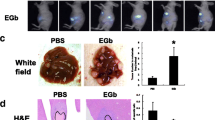
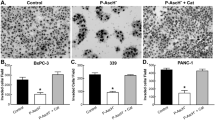
Bovine liver catalase derivatives possessing diverse tissue distribution properties were synthesized, and their effects on hepatic metastasis of colon carcinoma cells were examined in mice. An intraportal injection of 1 × 105 colon 26 cells resulted in the formation of more than 50 metastatic colonies on the surface of the liver at 14 days after injection. An intravenous injection of catalase (CAT; 35 000 units/kg of body weight) significantly (P < 0.001) reduced the number of the colonies in the liver. Galactosylated (Gal-), mannosylated (Man-) and succinylated (Suc-) CAT were also tested in the same system. Of these derivatives, Gal-CAT showed the greatest inhibitory effect on hepatic metastasis, and the number of colonies was significantly (P < 0.001) smaller than following treatment with catalase. High activities of matrix metalloproteinases (MMPs), especially MMP-9, were detected in the liver of mice bearing metastatic tumor tissues, which was significantly (P < 0.05) reduced by Gal-CAT. These results, combined with our previous finding that Gal-CAT can be efficiently delivered to hepatocytes, indicate that the targeted delivery of catalase to the liver by galactosylation is a promising approach to suppress hepatic metastasis. Decreased MMP activity by catalase delivery seems to be involved in its anti-metastatic effect.
Abbreviations: CAT – bovine liver catalase; ECM – extracellular matrix; Gal – galactosylated; HBSS – Hanks' balanced salt solution; H2O2– hydrogen peroxide; Man – mannosylated; MMP – matrix metalloproteinase; ROS – reactive oxygen species; Suc – succinylated; SOD – superoxide dismutase
Similar content being viewed by others
References
Engers R, Gabbert HE. Mechanisms of tumor metastasis: Cell biological aspects and clinical implications. J Cancer Res Clin Oncol 2000; 126: 682–92.
Onoda JM, Piechocki MP, Honn KV. Radiation-induced increase in expression of the aIIβ3 integrin in melanoma cells: Effects on metastatic potential. Radiat Res 1992; 130: 281–8.
Sellak H, Franzini E, Hakim J et al. Reactive oxygen species rapidly increase endothelial ICAM-1 ability to bind neutrophils without detectable upregulation. Blood 1994; 83: 2669–77.
Shaughnessy SG, Whaley M, Lafrenie RM et al. Walker 256 tumor cell degradation of extracellular matrices involves a latent gelatinase activated by reactive oxygen species. Arch Biochem Biophys 1993; 304: 314–21.
Rajagopalan S, Meng XP, Ramasamy S et al. Reactive oxygen species produced by macrophage-derived foam cells regulate the activity of vascular matrix metalloproteinases in vitro. Implications for atherosclerotic plaque stability. J Clin Invest 1996; 98: 2572–9.
Belkhiri A, Richards C, Whaley M et al. Increased expression of activated matrix metalloproteinase-2 by human endothelial cells after sublethal H2O2 exposure. Lab Invest 1997; 77: 533–9.
Mukai M, Shinkai K, Tateishi R et al. Macrophage potentiation of invasive capacity of rat ascites hepatoma cells. Cancer Res 1987; 47: 2167–71.
Murrell GA, Francis MJ, Bromley L. Modulation of fibroblast proliferation by oxygen free radicals. Biochem J 1990; 265: 659–65.
Adamson IY, Young L, Orr FW. Tumor metastasis after hyperoxic injury and repair of the pulmonary endothelium. Lab Invest 1987; 57: 71–7.
Szatrowski TP, Nathan CF. Production of large amounts of hydrogen peroxide by human tumor cells. Cancer Res 1991; 51: 7948.
Ben-Yoseph O, Ross BD. Oxidation therapy: The use of a reactive oxygen species-generating enzyme system for tumour treatment. Br J Cancer 1994; 70: 1131–5.
Fang J, Sawa T, Akaike T et al. Tumor-targeted delivery of polyethylene glycol-conjugated D-amino acid oxidase for antitumor therapy via enzymatic generation of hydrogen peroxide. Cancer Res 2002; 62: 3138–43.
Jessup JM, Battle P, Waller H et al. Reactive nitrogen and oxygen radicals formed during hepatic ischemia-reperfusion kill weakly metastatic colorectal cancer cells. Cancer Res 1999; 59: 1825–9.
Mavier P, Guigui B, Preaux AM et al. In vitrotoxicity of hydrogen peroxide against normal vs. tumor rat hepatocytes: Role of catalase and of the glutathione redox cycle. Hepatology 1988; 8: 1673–8.
Van Driel BE, Van Noorden CJ. Oxygen insensitivity of the histochemical assay of glucose-6-phosphate dehydrogenase activity for the discrimination between nonmalignant and malignant cells. J Histochem Cytochem 1999; 47: 575–82.
Malafa M, Margenthaler J, Webb B et al. MnSOD expression is increased in metastatic gastric cancer. J Surg Res 2000; 88: 130–134.
Nonaka Y, Iwagaki H, Kimura T et al. Effect of reactive oxygen intermediates on the in vitroinvasive capacity of tumor cells and liver metastasis in mice. Int J Cancer 1993; 54: 983–6.
Yoshizaki N, Mogi Y, Muramatsu H et al. Suppressive effect of recombinant human Cu, Zn-superoxide dismutase on lung metastasis of murine tumor cells. Int J Cancer 1994; 57: 287–92.
Fujita T, Nishikawa M, Tamaki C et al. Targeted delivery of human recombinant superoxide dismutase by chemical modification with mono-and polysaccharide derivatives. J Pharmacol Exp Ther 1992; 263: 971–8.
Yabe Y, Koyama Y, Nishikawa M et al. Hepatocyte-specific distribution of catalase and its inhibitory effect on hepatic ischemia/reperfusion injury in mice. Free Radic Res 1999; 30: 265–74.
Nishikawa M, Ohtsubo Y, Ohno J et al. Pharmacokinetics of receptormediated hepatic uptake of glycosylated albumin in mice. Int J Pharm 1992; 85: 75–85.
Takakura Y, Fujita T, Furitsu H et al. Pharmacokinetics of succinylated proteins and dextran sulfate in mice: Implications for hepatic targeting of protein drugs by direct succinylation via scavenger receptors. Int J Pharm 1994; 105: 19–29.
Fujita T, Furitsu H, Nishikawa M et al. Therapeutic effects of superoxide dismutase derivatives modified with mono-or polysaccharides on hepatic injury induced by ischemia/reperfusion. Biochem Biophys Res Commun 1992; 189: 191–6.
Yabe Y, Nishikawa M, Tamada A et al. Targeted delivery and improved therapeutic potential of catalase by chemical modification: combination with superoxide dismutase derivatives. J Pharmacol Exp Ther 1999; 289: 1176–84.
Mihara K, Oka Y, Sawai K et al. Improvement of therapeutic effect of human recombinant superoxide dismutase on ischemic acute renal failure in the rat via cationization and conjugation with polyethylene glycol. J Drug Target 1994; 2: 317–21.
Yabe Y, Kobayashi N, Nishihashi T et al. Prevention of neutrophilmediated hepatic ischemia/reperfusion injury by SOD and catalase derivatives. J Pharmacol Exp Ther 2001; 298: 894–9.
Nishikawa M, Tamada A, Kumai H et al. Inhibition of experimental pulmonary metastasis by controlling biodistribution of catalase in mice. Int J Cancer 2002; 99: 474–9.
Miyahara T, Samejima T. Effects of halide ions on porcine kidney catalase. J Biochem 1982; 91: 525–35.
Thakur ML, Coleman RE, Welch MJ. Indium-111-labeled leukocytes for the localization of abscesses: Preparation, analysis, tissue distribution, and comparison with gallium-67 citrate in dogs. J Lab Clin Med 1977; 89: 217–28.
Safford SE, Oberley TD, Urano M et al. Suppression of fibrosarcoma metastasis by elevated expression of manganese superoxide dismutase. Cancer Res 1994; 54: 4261–5.
Anasagasti MJ, Alvarez A, Martin JJ et al. Sinusoidal endothelium release of hydrogen peroxide enhances very late antigen-4-mediated melanoma cell adherence and tumor cytotoxicity during interleukin-1 promotion of hepatic melanoma metastasis in mice. Hepatology 1997; 25: 840–6.
Kogawa K, Muramatsu H, Tanaka M et al. Enhanced inhibition of experimental metastasis by the combination chemotherapy of Cu-Zn SOD and adriamycin. Clin Exp Metast 1999; 17: 239–44.
Tanaka M, Kogawa K, Nishihori Y et al. Suppression of intracellular Cu-Zn SOD results in enhanced motility and metastasis of Meth A sarcoma cells. Int J Cancer 1997; 73: 187–92.
Takenaga M, Igarashi R, Ochiai A, Mizushima Y. Effect of lecithinized superoxide dismutase (PC-SOD) on experimental pulmonary metastasis in mice. Free Radic Biol Med 1999; 26: 1117–25.
Blood CH, Zetter BR. Tumor interactions with the vasculature: Angiogenesis and tumor metastasis. Biochim Biophys Acta 1990; 1032: 89–118.
Pearson HJ, Anderson J, Chamberlain J et al. The effect of Kupffer cell stimulation or depression on the development of liver metastases in the rat. Cancer Immunol Immunother 1986; 23: 214–6.
Bayon LG, Izquierdo MA, Sirovich I et al. Role of Kupffer cells in arresting circulating tumor cells and controlling metastatic growth in the liver. Hepatology 1996; 23: 1224–31.
Phillips NC. Kupffer cells and liver metastasis. Optimization and limitation of activation of tumoricidal activity. Cancer Metast Rev 1989; 8: 231–52.
Rushfeldt C, Sveinbjornsson B, Seljelid R et al. Early events of hepatic metastasis formation in mice: Role of Kupffer and NK-cells in natural and interferon-gamma-stimulated defense. J Surg Res 1999; 82: 209–15.
Nathan CF. Secretory products of macrophages. J Clin Invest 1987; 79: 319–26.
Curran S, Murray GI. Matrix metalloproteinases: Molecular aspects of their roles in tumour invasion and metastasis. Eur J Cancer 2000; 36: 1621–30.
Wenk J, Brenneisen P, Wlaschek M et al. Stable overexpression of manganese superoxide dismutase in mitochondria identifies hydrogen peroxide as amajor oxidant in the AP-1-mediated induction of matrixdegrading metalloprotease-1. J Biol Chem 1999; 274: 25869–76.
Nelson KK, Ranganathan AC, Mansouri J et al. Elevated sod2 activity augments matrix metalloproteinase expression: Evidence for the involvement of endogenous hydrogen peroxide in regulating metastasis.Clin Cancer Res 2003; 9: 424–32.
Tamura Y, Watanabe F, Nakatani T et al. Highly selective and orally active inhibitors of type IV collagenase (MMP-9 and MMP-2): Nsulfonylamino acid derivatives. J Med Chem. 1998; 41: 640–9.
Haruyama T, Ajioka I, Akaike T et al. Regulation and significance of hepatocyte-derived matrix metalloproteinases in liver remodeling. Biochem Biophys Res Commun 2000; 272: 681–6.
Rights and permissions
About this article
Cite this article
Nishikawa, M., Tamada, A., Hyoudou, K. et al. Inhibition of experimental hepatic metastasis by targeted delivery of catalase in mice. Clin Exp Metastasis 21, 213–221 (2004). https://doi.org/10.1023/B:CLIN.0000037706.13747.5e
Issue Date:
DOI: https://doi.org/10.1023/B:CLIN.0000037706.13747.5e