Abstract
Consumption of fish containing ciguatera toxins or ciguatoxins (CTXs) causes ciguatera fish poisoning (CFP). In some patients, CFP recurrence occurs even years after exposure related to CTXs accumulation. Pacific CTX-1 (P-CTX-1) is one of the most potent natural substances known that causes predominantly neurological symptoms in patients; however, the underlying pathogenies of CFP remain unknown. Using clinically relevant neurobehavioral tests and electromyography (EMG) to assess effects of P-CTX-1 during the 4 months after exposure, recurrent motor strength deficit occurred in mice exposed to P-CTX-1. We detected irreversible motor strength deficits accompanied by reduced EMG activity, demyelination, and slowing of motor nerve conduction, whereas control unexposed mice fully recovered in 1 month after peripheral nerve injury. Finally, to uncover the mechanism underlying CFP, we detected reduction of spontaneous firing rate of motor cortical neurons even 6 months after exposure and increased number of glial fibrillary acidic protein (GFAP)-immunoreactive astrocytes. Increased numbers of motor cortical neuron apoptosis were detected by dUTP-digoxigenin nick end labeling assay along with activation of caspase 3. Taken together, our study demonstrates that persistence of P-CTX-1 in the nervous system induces irreversible motor deficit that correlates well with excitotoxicity and neurodegeneration detected in the motor cortical neurons.








Similar content being viewed by others
References
Dickey RW, Plakas SM (2010) Ciguatera: A public health perspective. Toxicon : Off J Int Soc Toxinology 56(2):123–136. https://doi.org/10.1016/j.toxicon.2009.09.008
Bourdy G, Cabalion P, Amade P, Laurent D (1992) Traditional remedies used in the Western Pacific for the treatment of ciguatera poisoning. J Ethnopharmacol 36(2):163–174. https://doi.org/10.1016/0378-8741(92)90017-L
Banner AH (1976) Ciguatera: A disease from coral reef fish. Biol Geol Coral Reef 3:177–213
Randall JE (1958) A review of ciguatera, tropical fish poisoning, with a tentative explanation of its cause. Bull Mar Sci 8(3):236–267
De Fouw J, Van Egmond H, Speijers GJA (2001) Ciguatera fish poisoning: A review.
Radke EG, Reich A, Morris JG, Jr. (2015) Epidemiology of Ciguatera in Florida. Am J Trop Med Hyg 93 (2):425–432. doi:https://doi.org/10.4269/ajtmh.14-0400
Lewis RJ (2000) Ciguatera management. SPC Live Reef Fish Information Bulletin 7:11–13
Barton ED, Tanner P, Turchen SG, Tunget CL, Manoguerra A, Clark RF (1995) Ciguatera fish poisoning. A southern California epidemic. West J Med 163(1):31–35
Chan TY (1998) Lengthy persistence of ciguatoxin in the body. Trans R Soc Trop Med Hyg 92(6):662. https://doi.org/10.1016/S0035-9203(98)90803-3
Hamilton B, Whittle N, Shaw G, Eaglesham G, Moore MR, Lewis RJ (2010) Human fatality associated with Pacific ciguatoxin contaminated fish. Toxicon 56(5):668–673. https://doi.org/10.1016/j.toxicon.2009.06.007
Au NP, Kumar G, Asthana P, Tin C, Mak YL, Chan LL, Lam PK, Ma CH (2016) Ciguatoxin reduces regenerative capacity of axotomized peripheral neurons and delays functional recovery in pre-exposed mice after peripheral nerve injury. Sci Rep 6(1):26809. https://doi.org/10.1038/srep26809
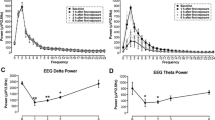
Kumar G, Au NP, Lei EN, Mak YL, Chan LL, Lam MH, Lam PK, Ma CH (2016) Acute exposure to Pacific ciguatoxin reduces electroencephalogram activity and disrupts neurotransmitter metabolic pathways in motor cortex. Mol Neurobiol 54(7):5590–5603. https://doi.org/10.1007/s12035-016-0093-y
Wang J, Cao B, Yang X, Wu J, Chan LL, Li Y (2017) Chronic ciguatoxin poisoning causes emotional and cognitive dysfunctions in rats. Toxicol Res 6(2):179–187. https://doi.org/10.1039/C5TX00475F
Bottein Dechraoui MY, Wang Z, Turquet J, Chinain M, Darius T, Cruchet P, Radwan FF, Dickey RW et al (2005) Biomonitoring of ciguatoxin exposure in mice using blood collection cards. Toxicon : Off J Int Soc Toxinology 46(3):243–251. https://doi.org/10.1016/j.toxicon.2005.03.014
Benoit E, Juzans P, Legrand AM, Molgo J (1996) Nodal swelling produced by ciguatoxin-induced selective activation of sodium channels in myelinated nerve fibers. Neuroscience 71(4):1121–1131. https://doi.org/10.1016/0306-4522(95)00506-4
Mattei C, Dechraoui MY, Molgo J, Meunier FA, Legrand AM, Benoit E (1999) Neurotoxins targetting receptor site 5 of voltage-dependent sodium channels increase the nodal volume of myelinated axons. J Neurosci Res 55(6):666–673. https://doi.org/10.1002/(SICI)1097-4547(19990315)55:6<666::AID-JNR2>3.0.CO;2-H
Hogg RC, Lewis RJ, Adams DJ (2002) Ciguatoxin-induced oscillations in membrane potential and action potential firing in rat parasympathetic neurons. Eur J Neurosci 16(2):242–248. https://doi.org/10.1046/j.1460-9568.2002.02071.x
Inserra MC, Israel MR, Caldwell A, Castro J, Deuis JR, Harrington AM, Keramidas A, Garcia-Caraballo S et al (2017) Multiple sodium channel isoforms mediate the pathological effects of Pacific ciguatoxin-1. Sci Rep 7:42810. https://doi.org/10.1038/srep42810
Babiloni C, Lizio R, Marzano N, Capotosto P, Soricelli A, Triggiani AI, Cordone S, Gesualdo L et al (2016) Brain neural synchronization and functional coupling in Alzheimer's disease as revealed by resting state EEG rhythms. Int J Psychophysiol 103:88–102. https://doi.org/10.1016/j.ijpsycho.2015.02.008
Foerster BR, Pomper MG, Callaghan BC, Petrou M, Edden RA, Mohamed MA, Welsh RC, Carlos RC et al (2013) An imbalance between excitatory and inhibitory neurotransmitters in amyotrophic lateral sclerosis revealed by use of 3-T proton magnetic resonance spectroscopy. JAMA Neurol 70(8):1009–1016. https://doi.org/10.1001/jamaneurol.2013.234
Kehrer C, Maziashvili N, Dugladze T, Gloveli T (2008) Altered excitatory-inhibitory balance in the NMDA-hypofunction model of schizophrenia. Front Mol Neurosci 1:6. https://doi.org/10.3389/neuro.02.006.2008
Ni Y, Su M, Lin J, Wang X, Qiu Y, Zhao A, Chen T, Jia W (2008) Metabolic profiling reveals disorder of amino acid metabolism in four brain regions from a rat model of chronic unpredictable mild stress. FEBS Lett 582(17):2627–2636. https://doi.org/10.1016/j.febslet.2008.06.040
Rubenstein JL, Merzenich MM (2003) Model of autism: Increased ratio of excitation/inhibition in key neural systems. Genes Brain Behav 2(5):255–267. https://doi.org/10.1034/j.1601-183X.2003.00037.x
Sun B, Halabisky B, Zhou Y, Palop JJ, Yu G, Mucke L, Gan L (2009) Imbalance between GABAergic and glutamatergic transmission impairs adult neurogenesis in an animal model of Alzheimer's disease. Cell Stem Cell 5(6):624–633. https://doi.org/10.1016/j.stem.2009.10.003
Aosaki T, Miura M, Suzuki T, Nishimura K, Masuda M (2010) Acetylcholine-dopamine balance hypothesis in the striatum: An update. Geriatr Gerontol Int 10(Suppl 1):S148–S157. https://doi.org/10.1111/j.1447-0594.2010.00588.x
Dong XX, Wang Y, Qin ZH (2009) Molecular mechanisms of excitotoxicity and their relevance to pathogenesis of neurodegenerative diseases. Acta Pharmacol Sin 30(4):379–387. https://doi.org/10.1038/aps.2009.24
Beal MF (1992) Mechanisms of excitotoxicity in neurologic diseases. FASEB J: Off Publ Fed Am Soc Exp Biol 6(15):3338–3344
Shaw PJ (1994) Excitotoxicity and motor neurone disease: A review of the evidence. J Neurol Sci 124(Suppl):6–13. https://doi.org/10.1016/0022-510X(94)90170-8
Beal MF (1998) Excitotoxicity and nitric oxide in Parkinson's disease pathogenesis. Ann Neurol 44(3 Suppl 1):S110–S114. https://doi.org/10.1002/ana.410440716
Wu JJ, Mak YL, Murphy MB, Lam JC, Chan WH, Wang M, Chan LL, Lam PK (2011) Validation of an accelerated solvent extraction liquid chromatography-tandem mass spectrometry method for Pacific ciguatoxin-1 in fish flesh and comparison with the mouse neuroblastoma assay. Anal Bioanal Chem 400(9):3165–3175. https://doi.org/10.1007/s00216-011-4977-4
Chan WH, Mak YL, JJ W, Jin L, Sit WH, Lam JC, Sadovy de Mitcheson Y, Chan LL et al (2011) Spatial distribution of ciguateric fish in the Republic of Kiribati. Chemosphere 84(1):117–123. https://doi.org/10.1016/j.chemosphere.2011.02.036
Bottein MY, Wang Z, Ramsdell JS (2011) Toxicokinetics of the ciguatoxin P-CTX-1 in rats after intraperitoneal or oral administration. Toxicology 284(1–3):1–6. https://doi.org/10.1016/j.tox.2011.02.005
Kumar G, Au NP, Lei EN, Mak YL, Chan LL, Lam MH, Chan LL, Lam PK et al (2016) Acute exposure to Pacific ciguatoxin reduces electroencephalogram activity and disrupts neurotransmitter metabolic pathways in motor cortex. Mol Neurobiol 54(7):5590–5603. https://doi.org/10.1007/s12035-016-0093-y
Ma CH, Brenner GJ, Omura T, Samad OA, Costigan M, Inquimbert P, Niederkofler V, Salie R et al (2011) The BMP coreceptor RGMb promotes while the endogenous BMP antagonist noggin reduces neurite outgrowth and peripheral nerve regeneration by modulating BMP signaling. J Neurosci 31(50):18391–18400. https://doi.org/10.1523/JNEUROSCI.4550-11.2011
Ma CH, Omura T, Cobos EJ, Latremoliere A, Ghasemlou N, Brenner GJ, van Veen E, Barrett L et al (2011) Accelerating axonal growth promotes motor recovery after peripheral nerve injury in mice. J Clin Invest 121(11):4332–4347. https://doi.org/10.1172/JCI58675
Inserra MM, Bloch DA, Terris DJ (1998) Functional indices for sciatic, peroneal, and posterior tibial nerve lesions in the mouse. Microsurgery 18(2):119–124. https://doi.org/10.1002/(SICI)1098-2752(1998)18:2<119::AID-MICR10>3.0.CO;2-0
Painter MW, Brosius Lutz A, Cheng YC, Latremoliere A, Duong K, Miller CM, Posada S, Cobos EJ et al (2014) Diminished Schwann cell repair responses underlie age-associated impaired axonal regeneration. Neuron 83(2):331–343. https://doi.org/10.1016/j.neuron.2014.06.016
Zhang X, Cao B, Wang J, Liu J, Tung VO, Lam PK, Chan LL, Li Y (2013) Neurotoxicity and reactive astrogliosis in the anterior cingulate cortex in acute ciguatera poisoning. NeuroMolecular Med 15(2):310–323. https://doi.org/10.1007/s12017-013-8220-7
Pearn J (2001) Neurology of ciguatera. J Neurol Neurosurg Psychiatry 70(1):4–8. https://doi.org/10.1136/jnnp.70.1.4
Bagnis R, Kuberski T, Laugier S (1979) Clinical observations on 3,009 cases of ciguatera (fish poisoning) in the South Pacific. Am J Trop Med Hyg 28(6):1067–1073. https://doi.org/10.4269/ajtmh.1979.28.1067
Derouiche F, Cohen E, Rodier G, Boulay C, Courtois S (2000) Ciguatera and peripheral neuropathy: A case report. Rev Neurol (Paris) 156(5):514–516
Sozzi G, Marotta P, Aldeghi D, Tredici G, Calvi L (1988) Polyneuropathy secondary to ciguatoxin poisoning. Ital J Neurol Sci 9(5):491–495. https://doi.org/10.1007/BF02337168
Deber CM, Reynolds SJ (1991) Central nervous system myelin: Structure, function, and pathology. Clin Biochem 24(2):113–134. https://doi.org/10.1016/0009-9120(91)90421-A
Weil MT, Mobius W, Winkler A, Ruhwedel T, Wrzos C, Romanelli E, Bennett JL, Enz L et al (2016) Loss of myelin basic protein function triggers myelin breakdown in models of demyelinating diseases. Cell Rep 16(2):314–322. https://doi.org/10.1016/j.celrep.2016.06.008
Purves D, Augustine G, Fitzpatrick D, Katz L, LaMantia A, McNamara J, Williams S (2001) Increased conduction velocity as a result of myelination. Neuroscience
Huxley C, Passage E, Robertson AM, Youl B, Huston S, Manson A, Saberan-Djoniedi D, Figarella-Branger D et al (1998) Correlation between varying levels of PMP22 expression and the degree of demyelination and reduction in nerve conduction velocity in transgenic mice. Hum Mol Genet 7(3):449–458. https://doi.org/10.1093/hmg/7.3.449
Lim EF, Nakanishi ST, Hoghooghi V, Eaton SE, Palmer AL, Frederick A, Stratton JA, Stykel MG et al (2017) AlphaB-crystallin regulates remyelination after peripheral nerve injury. Proc Natl Acad Sci U S A 114(9):E1707–E1716. https://doi.org/10.1073/pnas.1612136114
Tsodyks M, Kenet T, Grinvald A, Arieli A (1999) Linking spontaneous activity of single cortical neurons and the underlying functional architecture. Science 286(5446):1943–1946. https://doi.org/10.1126/science.286.5446.1943
Philips T, Robberecht W (2011) Neuroinflammation in amyotrophic lateral sclerosis: Role of glial activation in motor neuron disease. Lancet Neurol 10(3):253–263. https://doi.org/10.1016/S1474-4422(11)70015-1
O'Callaghan JP, Sriram K (2005) Glial fibrillary acidic protein and related glial proteins as biomarkers of neurotoxicity. Expert Opin Drug Saf 4(3):433–442. https://doi.org/10.1517/14740338.4.3.433
Carron SF, Yan EB, Alwis DS, Rajan R (2016) Differential susceptibility of cortical and subcortical inhibitory neurons and astrocytes in the long term following diffuse traumatic brain injury. J Comp Neurol 524(17):3530–3560. https://doi.org/10.1002/cne.24014
Faiz M, Sachewsky N, Gascon S, Bang KW, Morshead CM, Nagy A (2015) Adult neural stem cells from the subventricular zone give rise to reactive astrocytes in the cortex after stroke. Cell Stem Cell 17(5):624–634. https://doi.org/10.1016/j.stem.2015.08.002
Jeong HK, Ji KM, Min KJ, Choi I, Choi DJ, Jou I, Joe EH (2014) Astrogliosis is a possible player in preventing delayed neuronal death. Mol Cells 37(4):345–355. https://doi.org/10.14348/molcells.2014.0046
Buffo A, Rite I, Tripathi P, Lepier A, Colak D, Horn AP, Mori T, Gotz M (2008) Origin and progeny of reactive gliosis: A source of multipotent cells in the injured brain. Proc Natl Acad Sci U S A 105(9):3581–3586. https://doi.org/10.1073/pnas.0709002105
RAGELIS EP (1984) Ciguatera seafood poisoning: Overview. In. ACS Publications,
Skinner MP, Brewer TD, Johnstone R, Fleming LE, Lewis RJ (2011) Ciguatera fish poisoning in the Pacific Islands (1998 to 2008). PLoS Negl Trop Dis 5(12):e1416. https://doi.org/10.1371/journal.pntd.0001416
Lehane L, Lewis RJ (2000) Ciguatera: Recent advances but the risk remains. Int J Food Microbiol 61(2–3):91–125. https://doi.org/10.1016/S0168-1605(00)00382-2
Lewis RJ, Sellin M (1992) Multiple ciguatoxins in the flesh of fish. Toxicon : Off J Int Soc Toxinology 30(8):915–919. https://doi.org/10.1016/0041-0101(92)90390-Q
Katz AR, Terrell-Perica S, Sasaki DM (1993) Ciguatera on Kauai: Investigation of factors associated with severity of illness. Am J Trop Med Hyg 49(4):448–454. https://doi.org/10.4269/ajtmh.1993.49.448
Bailey S (2014) Withers T (2014) ciguatera poisoning in the Cook Islands. BMJ Case Rep 2014(jun25 1):bcr2014204847. https://doi.org/10.1136/bcr-2014-204847
Boada LD, Zumbado M, Luzardo OP, Almeida-Gonzalez M, Plakas SM, Granade HR, Abraham A, Jester EL et al (2010) Ciguatera fish poisoning on the West Africa Coast: An emerging risk in the Canary Islands (Spain). Toxicon : Off J Int Soc Toxinology 56(8):1516–1519. https://doi.org/10.1016/j.toxicon.2010.07.021
Chateau-Degat ML, Beuter A, Vauterin G, Nguyen NL, Chinain M, Darius T, Legrand AM, Chansin R et al (2007) Neurologic signs of ciguatera disease: Evidence of their persistence. Am J Trop Med Hyg 77(6):1170–1175
McKee DB, Fleming L, Tamer R, Weisman R, Blythe D (2001) Physician diagnosis and reporting of ciguatera fish poisoning in an endemic area. Harmful Algal Blooms 2000:451–453
Terao K, Ito E, Oarada M, Ishibashi Y, Legrand AM, Yasumoto T (1991) Light and electron microscopic studies of pathologic changes induced in mice by ciguatoxin poisoning. Toxicon : Off J Int Soc Toxinology 29(6):633–643. https://doi.org/10.1016/0041-0101(91)90056-W
Tunstall RJ, Mehan KA, Wadley GD, Collier GR, Bonen A, Hargreaves M, Cameron-Smith D (2002) Exercise training increases lipid metabolism gene expression in human skeletal muscle. Am J Physiol Endocrinol Metab 283(1):E66–E72. https://doi.org/10.1152/ajpendo.00475.2001
Lange WR, Snyder FR, Fudala PJ (1992) Travel and ciguatera fish poisoning. Arch Intern Med 152(10):2049–2053. https://doi.org/10.1001/archinte.1992.00400220075013
Nicholson GM, Lewis RJ (2006) Ciguatoxins: Cyclic polyether modulators of voltage-gated Iion channel function. Marine Drugs 4(3):82–118
Bagnis R (1993) Ciguatera fish poisoning.
Gillespie NC, Lewis RJ, Pearn JH, Bourke AT, Holmes MJ, Bourke JB, Shields WJ (1986) Ciguatera in Australia. Occurrence, clinical features, pathophysiology and management. Med J Aust 145(11–12):584–590
Glaziou P, Martin PM (1993) Study of factors that influence the clinical response to ciguatera fish poisoning. Toxicon 31(9):1151–1154. https://doi.org/10.1016/0041-0101(93)90130-B
Benoit E, Mattei C, Ouanounou G, Meunier FA, Suput D, Le Gall F, Marquais M, Dechraoui MY et al (2002) Ionic mechanisms involved in the nodal swelling of myelinated axons caused by marine toxins. Cell Mol Biol Lett 7(2):317–321
Allsop JL, Martini L, Lebris H, Pollard J, Walsh J, Hodgkinson S (1986) Neurologic manifestations of ciguatera. 3 cases with a neurophysiologic study and examination of one nerve biopsy. Rev Neurol (Paris) 142(6–7):590–597
Nawaz S, Kippert A, Saab AS, Werner HB, Lang T, Nave KA, Simons M (2009) Phosphatidylinositol 4,5-bisphosphate-dependent interaction of myelin basic protein with the plasma membrane in oligodendroglial cells and its rapid perturbation by elevated calcium. J Neurosci 29(15):4794–4807. https://doi.org/10.1523/JNEUROSCI.3955-08.2009
Hidalgo J, Liberona JL, Molgo J, Jaimovich E (2002) Pacific ciguatoxin-1b effect over Na+ and K+ currents, inositol 1,4,5-triphosphate content and intracellular Ca2+ signals in cultured rat myotubes. Br J Pharmacol 137(7):1055–1062. https://doi.org/10.1038/sj.bjp.0704980
Molgo J, Shimahara T, Legrand AM (1993) Ciguatoxin, extracted from poisonous morays eels, causes sodium-dependent calcium mobilization in NG108-15 neuroblastoma x glioma hybrid cells. Neurosci Lett 158(2):147–150. https://doi.org/10.1016/0304-3940(93)90250-O
Ryan JC, Morey JS, Bottein MY, Ramsdell JS, Van Dolah FM (2010) Gene expression profiling in brain of mice exposed to the marine neurotoxin ciguatoxin reveals an acute anti-inflammatory, neuroprotective response. BMC Neurosci 11(1):107. https://doi.org/10.1186/1471-2202-11-107
Farooqui AA, Horrocks LA (1994) Involvement of glutamate receptors, lipases, and phospholipases in long-term potentiation and neurodegeneration. J Neurosci Res 38(1):6–11. https://doi.org/10.1002/jnr.490380103
Ribeiro FM, Vieira LB, Pires RG, Olmo RP, Ferguson SS (2017) Metabotropic glutamate receptors and neurodegenerative diseases. Pharmacol Res 115:179–191. https://doi.org/10.1016/j.phrs.2016.11.013
Butterfield DA, Pocernich CB (2003) The glutamatergic system and Alzheimer's disease: Therapeutic implications. CNS Drugs 17(9):641–652. https://doi.org/10.2165/00023210-200317090-00004
Litim N, Morissette M, Di Paolo T (2017) Metabotropic glutamate receptors as therapeutic targets in Parkinson's disease: An update from the last 5 years of research. Neuropharmacology 115:166–179. https://doi.org/10.1016/j.neuropharm.2016.03.036
Rossi DJ, Oshima T, Attwell D (2000) Glutamate release in severe brain ischaemia is mainly by reversed uptake. Nature 403(6767):316–321. https://doi.org/10.1038/35002090
Pitt D, Werner P, Raine CS (2000) Glutamate excitotoxicity in a model of multiple sclerosis. Nat Med 6(1):67–70. https://doi.org/10.1038/71555
Barker-Haliski M, White HS (2015) Glutamatergic mechanisms associated with seizures and epilepsy. Cold Spring Harb Perspect Med 5(8):a022863. https://doi.org/10.1101/cshperspect.a022863
Eulenburg V, Gomeza J (2010) Neurotransmitter transporters expressed in glial cells as regulators of synapse function. Brain Res Rev 63(1–2):103–112. https://doi.org/10.1016/j.brainresrev.2010.01.003
Lenk K, Raisanen E, Hyttinen JA (2016) Understanding the role of astrocytic GABA in simulated neural networks. Conf Proc IEEE Eng Med Biol Soc 2016:6121–6124. https://doi.org/10.1109/EMBC.2016.7592125
Barca-Mayo O, Pons-Espinal M, Follert P, Armirotti A, Berdondini L, De Pietri Tonelli D (2017) Astrocyte deletion of Bmal1 alters daily locomotor activity and cognitive functions via GABA signalling. Nat Commun 8:14336. https://doi.org/10.1038/ncomms14336
Fattorini G, Melone M, Sanchez-Gomez MV, Arellano RO, Bassi S, Matute C, Conti F (2017) GAT-1 mediated GABA uptake in rat oligodendrocytes. Glia 65(3):514–522. https://doi.org/10.1002/glia.23108
Jo S, Yarishkin O, Hwang YJ, Chun YE, Park M, Woo DH, Bae JY, Kim T et al (2014) GABA from reactive astrocytes impairs memory in mouse models of Alzheimer's disease. Nat Med 20(8):886–896. https://doi.org/10.1038/nm.3639
Rothstein JD (2009) Current hypotheses for the underlying biology of amyotrophic lateral sclerosis. Ann Neurol 65 Suppl 1(S1):S3–S9. https://doi.org/10.1002/ana.21543
Lewerenz J, Maher P (2015) Chronic glutamate toxicity in neurodegenerative diseases-what is the evidence? Front Neurosci 9:469. https://doi.org/10.3389/fnins.2015.00469
Estrada Sanchez AM, Mejia-Toiber J, Massieu L (2008) Excitotoxic neuronal death and the pathogenesis of Huntington's disease. Arch Med Res 39(3):265–276. https://doi.org/10.1016/j.arcmed.2007.11.011
Caudle WM, Zhang J (2009) Glutamate, excitotoxicity, and programmed cell death in Parkinson disease. Exp Neurol 220(2):230–233. https://doi.org/10.1016/j.expneurol.2009.09.027
Hynd MR, Scott HL, Dodd PR (2004) Glutamate-mediated excitotoxicity and neurodegeneration in Alzheimer's disease. Neurochem Int 45(5):583–595. https://doi.org/10.1016/j.neuint.2004.03.007
Rattray M, Bendotti C (2006) Does excitotoxic cell death of motor neurons in ALS arise from glutamate transporter and glutamate receptor abnormalities? Exp Neurol 201(1):15–23. https://doi.org/10.1016/j.expneurol.2006.05.001
Tilleux S, Hermans E (2007) Neuroinflammation and regulation of glial glutamate uptake in neurological disorders. J Neurosci Res 85(10):2059–2070. https://doi.org/10.1002/jnr.21325
Colangelo AM, Alberghina L, Papa M (2014) Astrogliosis as a therapeutic target for neurodegenerative diseases. Neurosci Lett 565:59–64. https://doi.org/10.1016/j.neulet.2014.01.014
Eid T, Ghosh A, Wang Y, Beckstrom H, Zaveri HP, Lee TS, Lai JC, Malthankar-Phatak GH et al (2008) Recurrent seizures and brain pathology after inhibition of glutamine synthetase in the hippocampus in rats. Brain : a journal of neurology 131(Pt 8):2061–2070. https://doi.org/10.1093/brain/awn133
van Landeghem FK, Weiss T, Oehmichen M, von Deimling A (2006) Decreased expression of glutamate transporters in astrocytes after human traumatic brain injury. J Neurotrauma 23(10):1518–1528. https://doi.org/10.1089/neu.2006.23.1518
Knyazeva MG, Jalili M, Brioschi A, Bourquin I, Fornari E, Hasler M, Meuli R, Maeder P et al (2010) Topography of EEG multivariate phase synchronization in early Alzheimer's disease. Neurobiol Aging 31(7):1132–1144. https://doi.org/10.1016/j.neurobiolaging.2008.07.019
Han CX, Wang J, Yi GS, Che YQ (2013) Investigation of EEG abnormalities in the early stage of Parkinson's disease. Cogn Neurodyn 7(4):351–359. https://doi.org/10.1007/s11571-013-9247-z
Vieregge P, Wauschkuhn B, Heberlein I, Hagenah J, Verleger R (1999) Selective attention is impaired in amyotrophic lateral sclerosis–a study of event-related EEG potentials. Brain research. Cogn Brain Res 8(1):27–35. https://doi.org/10.1016/S0926-6410(99)00004-X
Chaturvedi M, Hatz F, Gschwandtner U, Bogaarts JG, Meyer A, Fuhr P, Roth V (2017) Quantitative EEG (QEEG) measures differentiate Parkinson's disease (PD) patients from healthy controls (HC). Front Aging Neurosci 9:3. https://doi.org/10.3389/fnagi.2017.00003
Schmidt MT, Kanda PA, Basile LF, da Silva Lopes HF, Baratho R, Demario JL, Jorge MS, Nardi AE et al (2013) Index of alpha/theta ratio of the electroencephalogram: A new marker for Alzheimer's disease. Front Aging Neurosci 5:60. https://doi.org/10.3389/fnagi.2013.00060
Klassen BT, Hentz JG, Shill HA, Driver-Dunckley E, Evidente VG, Sabbagh MN, Adler CH, Caviness JN (2011) Quantitative EEG as a predictive biomarker for Parkinson disease dementia. Neurology 77(2):118–124. https://doi.org/10.1212/WNL.0b013e318224af8d
Westlake KP, Hinkley LB, Bucci M, Guggisberg AG, Byl N, Findlay AM, Henry RG, Nagarajan SS (2012) Resting state alpha-band functional connectivity and recovery after stroke. Exp Neurol 237(1):160–169. https://doi.org/10.1016/j.expneurol.2012.06.020
Bertram L, Tanzi RE (2005) The genetic epidemiology of neurodegenerative disease. J Clin Invest 115(6):1449–1457. https://doi.org/10.1172/JCI24761
Hatcher JM, Pennell KD, Miller GW (2008) Parkinson's disease and pesticides: A toxicological perspective. Trends Pharmacol Sci 29(6):322–329. https://doi.org/10.1016/j.tips.2008.03.007
Pan-Montojo F, Reichmann H (2014) Considerations on the role of environmental toxins in idiopathic Parkinson's disease pathophysiology. Transl Neurodegener 3(1):10. https://doi.org/10.1186/2047-9158-3-10
Cox PA, Davis DA, Mash DC, Metcalf JS, Banack SA (2016) Dietary exposure to an environmental toxin triggers neurofibrillary tangles and amyloid deposits in the brain. Proc Biol Sci 283(1823):20152397. https://doi.org/10.1098/rspb.2015.2397
Di Monte DA (2003) The environment and Parkinson's disease: Is the nigrostriatal system preferentially targeted by neurotoxins? Lancet Neurol 2(9):531–538. https://doi.org/10.1016/S1474-4422(03)00501-5
Caller T, Henegan P, Stommel E (2017) The potential role of BMAA in neurodegeneration. Neurotox Res 33(1):222–226. https://doi.org/10.1007/s12640-017-9752-7
Cox PA, Banack SA, Murch SJ (2003) Biomagnification of cyanobacterial neurotoxins and neurodegenerative disease among the Chamorro people of Guam. Proc Natl Acad Sci U S A 100(23):13380–13383. https://doi.org/10.1073/pnas.2235808100
Acknowledgements
This work is supported in part by The Health and Medical Research Fund (HMRF), Food and Health Bureau, Hong Kong Special Administrative Region Government (Ref. No: 01122016 and 12134101), GRF grants from the Research Grant Council of the Hong Kong Special Administrative Region Government (CityU 11100015 and CityU 160813), SRG (7004587) and ARG (9667149) grants from the City University of Hong Kong award to Chi Ma, and the Collaborative Research Fund, the Research Grant Council of Hong Kong (C1012-15G) award to Paul Lam.
Author information
Authors and Affiliations
Contributions
PA conducted in vivo electrophysiological study, NMJ and MBP quantification, performed sciatic nerve surgery and tissue harvest. NZ carried out the neurobehavioral assessments and data analysis with PA. GK performed single cell neuronal recording and GFAP staining. VBC and KKS performed experiments to confirm cell death. YLM performed P-CTX-1 extraction and tissue distribution analysis with expertise and resources provided by LLC and PKSL CHEM conceived the project and designed the study. PA, GK, and CHEM wrote the manuscript with inputs from all authors. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(PDF 700 kb)
Rights and permissions
About this article
Cite this article
Asthana, P., Zhang, N., Kumar, G. et al. Pacific Ciguatoxin Induces Excitotoxicity and Neurodegeneration in the Motor Cortex Via Caspase 3 Activation: Implication for Irreversible Motor Deficit. Mol Neurobiol 55, 6769–6787 (2018). https://doi.org/10.1007/s12035-018-0875-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-0875-5