Abstract
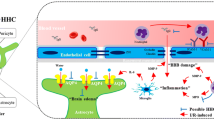
Curcumin and nano-curcumin both exhibit neuroprotective effects in early brain injury (EBI) after experimental subarachnoid hemorrhage (SAH). However, the mechanism that whether curcumin and its nanoparticles affect the blood–brain barrier (BBB) following SAH remains unclear. This study investigated the effect of curcumin and the poly(lactide-co-glycolide) (PLGA)-encapsulated curcumin nanoparticles (Cur-NPs) on BBB disruption and evaluated the possible mechanism underlying BBB dysfunction in EBI using the endovascular perforation rat SAH model. The results indicated that Cur-NPs showed enhanced therapeutic effects than that of curcumin in improving neurological function, reducing brain water content, and Evans blue dye extravasation after SAH. Mechanically, Cur-NPs attenuated BBB dysfunction after SAH by preventing the disruption of tight junction protein (ZO-1, occludin, and claudin-5). Cur-NPs also up-regulated glutamate transporter-1 and attenuated glutamate concentration of cerebrospinal fluid following SAH. Moreover, inhibition of inflammatory response and microglia activation both contributed to Cur-NPs’ protective effects. Additionally, Cur-NPs markedly suppressed SAH-mediated oxidative stress and eventually reversed SAH-induced cell apoptosis in rats. Our findings revealed that the strategy of using Cur-NPs could be a promising way in improving neurological function in EBI after experimental rat SAH.







Similar content being viewed by others
References
Macdonald RL (2014) Delayed neurological deterioration after subarachnoid haemorrhage. Nat Rev Neurol 10(1):44–58. doi:10.1038/nrneurol.2013.246
Sehba FA, Hou J, Pluta RM, Zhang JH (2012) The importance of early brain injury after subarachnoid hemorrhage. Prog Neurobiol 97(1):14–37. doi:10.1016/j.pneurobio.2012.02.003
Fujii M, Yan J, Rolland WB, Soejima Y, Caner B, Zhang JH (2013) Early brain injury, an evolving frontier in subarachnoid hemorrhage research. Transl Stroke Res 4(4):432–446. doi:10.1007/s12975-013-0257-2
Chen S, Feng H, Sherchan P, Klebe D, Zhao G, Sun X, Zhang J, Tang J et al (2014) Controversies and evolving new mechanisms in subarachnoid hemorrhage. Prog Neurobiol 115:64–91. doi:10.1016/j.pneurobio.2013.09.002
Wu CT, Wen LL, Wong CS, Tsai SY, Chan SM, Yeh CC, Borel CO, Cherng CH (2011) Temporal changes in glutamate, glutamate transporters, basilar arteries wall thickness, and neuronal variability in an experimental rat model of subarachnoid hemorrhage. Anesth Analg 112(3):666–673. doi:10.1213/ANE.0b013e318207c51f
Lai TW, Zhang S, Wang YT (2014) Excitotoxicity and stroke: identifying novel targets for neuroprotection. Prog Neurobiol 115:157–188. doi:10.1016/j.pneurobio.2013.11.006
Ayer RE, Zhang JH (2008) Oxidative stress in subarachnoid haemorrhage: significance in acute brain injury and vasospasm. Acta Neurochi Suppl 104:33–41
Miller BA, Turan N, Chau M, Pradilla G (2014) Inflammation, vasospasm, and brain injury after subarachnoid hemorrhage. BioMed Res Int 2014:384342. doi:10.1155/2014/384342
Noorafshan A, Ashkani-Esfahani S (2013) A review of therapeutic effects of curcumin. Curr Pharm Des 19(11):2032–2046
Tsai YM, Chien CF, Lin LC, Tsai TH (2011) Curcumin and its nano-formulation: the kinetics of tissue distribution and blood–brain barrier penetration. Int J Pharm 416(1):331–338. doi:10.1016/j.ijpharm.2011.06.030
Xie X, Tao Q, Zou Y, Zhang F, Guo M, Wang Y, Wang H, Zhou Q et al (2011) PLGA nanoparticles improve the oral bioavailability of curcumin in rats: characterizations and mechanisms. J Agric Food Chem 59(17):9280–9289. doi:10.1021/jf202135j
Khalil NM, do Nascimento TC, Casa DM, Dalmolin LF, de Mattos AC, Hoss I, Romano MA, Mainardes RM (2013) Pharmacokinetics of curcumin-loaded PLGA and PLGA-PEG blend nanoparticles after oral administration in rats. Colloids Surf B: Biointerfaces 101:353–360. doi:10.1016/j.colsurfb.2012.06.024
Wakade C, King MD, Laird MD, Alleyne CH Jr, Dhandapani KM (2009) Curcumin attenuates vascular inflammation and cerebral vasospasm after subarachnoid hemorrhage in mice. Antioxid Redox Signal 11(1):35–45. doi:10.1089/ars.2008.2056
Kuo CP, Lu CH, Wen LL, Cherng CH, Wong CS, Borel CO, Ju DT, Chen CM et al (2011) Neuroprotective effect of curcumin in an experimental rat model of subarachnoid hemorrhage. Anesthesiology 115(6):1229–1238. doi:10.1097/ALN.0b013e31823306f0
Chang CZ, Wu SC, Lin CL, Kwan AL (2015) Curcumin, encapsulated in nano-sized PLGA, down-regulates nuclear factor kappaB (p65) and subarachnoid hemorrhage induced early brain injury in a rat model. Brain Res 1608:215–224. doi:10.1016/j.brainres.2015.02.039
Sugawara T, Ayer R, Jadhav V, Zhang JH (2008) A new grading system evaluating bleeding scale in filament perforation subarachnoid hemorrhage rat model. J Neurosci Methods 167(2):327–334. doi:10.1016/j.jneumeth.2007.08.004
Peng SF, Lee CY, Hour MJ, Tsai SC, Kuo DH, Chen FA, Shieh PC, Yang JS (2014) Curcumin-loaded nanoparticles enhance apoptotic cell death of U2OS human osteosarcoma cells through the Akt-Bad signaling pathway. Int J Oncol 44(1):238–246. doi:10.3892/ijo.2013.2175
Doggui S, Sahni JK, Arseneault M, Dao L, Ramassamy C (2012) Neuronal uptake and neuroprotective effect of curcumin-loaded PLGA nanoparticles on the human SK-N-SH cell line. J Alzheimer's Dis: JAD 30(2):377–392. doi:10.3233/JAD-2012-112141
Tiwari SK, Agarwal S, Seth B, Yadav A, Nair S, Bhatnagar P, Karmakar M, Kumari M et al (2014) Curcumin-loaded nanoparticles potently induce adult neurogenesis and reverse cognitive deficits in Alzheimer's disease model via canonical Wnt/beta-catenin pathway. ACS Nano 8(1):76–103. doi:10.1021/nn405077y
Zhang ZY, Sun BL, Liu JK, Yang MF, Li DW, Fang J, Zhang S, Yuan QL et al (2015) Activation of mGluR5 attenuates microglial activation and neuronal apoptosis in early brain injury after experimental subarachnoid hemorrhage in rats. Neurochem Res 40(6):1121–1132. doi:10.1007/s11064-015-1572-7
Zhang ZY, Yang MF, Wang T, Li DW, Liu YL, Zhang JH, Sun BL (2015) Cysteamine alleviates early brain injury via reducing oxidative stress and apoptosis in a rat experimental subarachnoid hemorrhage model. Cell Mol Neurobiol 35(4):543–553. doi:10.1007/s10571-014-0150-x
Kooijman E, Nijboer CH, van Velthoven CT, Mol W, Dijkhuizen RM, Kesecioglu J, Heijnen CJ (2014) Long-term functional consequences and ongoing cerebral inflammation after subarachnoid hemorrhage in the rat. PLoS ONE 9(6), e90584. doi:10.1371/journal.pone.0090584
Zhang ZY, Sun BL, Yang MF, Li DW, Fang J, Zhang S (2015) Carnosine attenuates early brain injury through its antioxidative and anti-apoptotic effects in a rat experimental subarachnoid hemorrhage model. Cell Mol Neurobiol 35(2):147–157. doi:10.1007/s10571-014-0106-1
Claassen J, Carhuapoma JR, Kreiter KT, Du EY, Connolly ES, Mayer SA (2002) Global cerebral edema after subarachnoid hemorrhage: frequency, predictors, and impact on outcome. Stroke; J Cereb Circ 33(5):1225–1232
Wu C, Hu Q, Chen J, Yan F, Li J, Wang L, Mo H, Gu C et al (2013) Inhibiting HIF-1alpha by 2ME2 ameliorates early brain injury after experimental subarachnoid hemorrhage in rats. Biochem Biophys Res Commun 437(3):469–474. doi:10.1016/j.bbrc.2013.06.107
Chen J, Chen G, Li J, Qian C, Mo H, Gu C, Yan F, Yan W et al (2014) Melatonin attenuates inflammatory response-induced brain edema in early brain injury following a subarachnoid hemorrhage: a possible role for the regulation of pro-inflammatory cytokines. J Pineal Res 57(3):340–347. doi:10.1111/jpi.12173
Scholler K, Trinkl A, Klopotowski M, Thal SC, Plesnila N, Trabold R, Hamann GF, Schmid-Elsaesser R et al (2007) Characterization of microvascular basal lamina damage and blood–brain barrier dysfunction following subarachnoid hemorrhage in rats. Brain Res 1142:237–246. doi:10.1016/j.brainres.2007.01.034
Boyko M, Melamed I, Gruenbaum BF, Gruenbaum SE, Ohayon S, Leibowitz A, Brotfain E, Shapira Y et al (2012) The effect of blood glutamate scavengers oxaloacetate and pyruvate on neurological outcome in a rat model of subarachnoid hemorrhage. Neurotherapeutics: J Am Soc Exp NeuroTherapeutics 9(3):649–657. doi:10.1007/s13311-012-0129-6
Divito CB, Underhill SM (2014) Excitatory amino acid transporters: roles in glutamatergic neurotransmission. Neurochem Int 73:172–180. doi:10.1016/j.neuint.2013.12.008
Lin CL, Kwan AL, Dumont AS, Su YF, Kassell NF, Wang CJ, Wu SC, Kuo CL et al (2007) Attenuation of experimental subarachnoid hemorrhage-induced increases in circulating intercellular adhesion molecule-1 and cerebral vasospasm by the endothelin-converting enzyme inhibitor CGS 26303. J Neurosurg 106(3):442–448. doi:10.3171/jns.2007.106.3.442
Oshiro EM, Hoffman PA, Dietsch GN, Watts MC, Pardoll DM, Tamargo RJ (1997) Inhibition of experimental vasospasm with anti-intercellular adhesion molecule-1 monoclonal antibody in rats. Stroke; Cereb Circ 28(10):2031–2037, discussion 2037–2038
Lu H, Shi JX, Chen HL, Hang CH, Wang HD, Yin HX (2009) Expression of monocyte chemoattractant protein-1 in the cerebral artery after experimental subarachnoid hemorrhage. Brain Res 1262:73–80. doi:10.1016/j.brainres.2009.01.017
Ayer R, Jadhav V, Sugawara T, Zhang JH (2011) The neuroprotective effects of cyclooxygenase-2 inhibition in a mouse model of aneurysmal subarachnoid hemorrhage. Acta Neurochir Suppl 111:145–149. doi:10.1007/978-3-7091-0693-8_24
Zheng B, Zheng T, Wang L, Chen X, Shi C, Zhao S (2010) Aminoguanidine inhibition of iNOS activity ameliorates cerebral vasospasm after subarachnoid hemorrhage in rabbits via restoration of dysfunctional endothelial cells. J Neurol Sci 295(1–2):97–103. doi:10.1016/j.jns.2010.04.012
Kooijman E, Nijboer CH, van Velthoven CT, Kavelaars A, Kesecioglu J, Heijnen CJ (2014) The rodent endovascular puncture model of subarachnoid hemorrhage: mechanisms of brain damage and therapeutic strategies. J Neuroinflammation 11:2. doi:10.1186/1742-2094-11-2
Nag S, Manias JL, Stewart DJ (2009) Pathology and new players in the pathogenesis of brain edema. Acta Neuropathol 118(2):197–217. doi:10.1007/s00401-009-0541-0
Manaenko A, Chen H, Kammer J, Zhang JH, Tang J (2011) Comparison Evans Blue injection routes: Intravenous versus intraperitoneal, for measurement of blood–brain barrier in a mice hemorrhage model. J Neurosci Methods 195(2):206–210. doi:10.1016/j.jneumeth.2010.12.013
Tso MK, Macdonald RL (2014) Subarachnoid hemorrhage: a review of experimental studies on the microcirculation and the neurovascular unit. Transl Stroke Res 5(2):174–189. doi:10.1007/s12975-014-0323-4
Shaikh J, Ankola DD, Beniwal V, Singh D, Kumar MN (2009) Nanoparticle encapsulation improves oral bioavailability of curcumin by at least 9-fold when compared to curcumin administered with piperine as absorption enhancer. Eur J Pharma Sci: Off J Eur Fed Pharm Sci 37(3–4):223–230. doi:10.1016/j.ejps.2009.02.019
Jung CS, Lange B, Zimmermann M, Seifert V (2013) CSF and serum biomarkers focusing on cerebral vasospasm and ischemia after subarachnoid hemorrhage. Stroke Res Treat 2013:560305. doi:10.1155/2013/560305
Germano A, Caffo M, Angileri FF, Arcadi F, Newcomb-Fernandez J, Caruso G, Meli F, Pineda JA et al (2007) NMDA receptor antagonist felbamate reduces behavioral deficits and blood–brain barrier permeability changes after experimental subarachnoid hemorrhage in the rat. J Neurotrauma 24(4):732–744. doi:10.1089/neu.2006.0181
Hanafy KA (2013) The role of microglia and the TLR4 pathway in neuronal apoptosis and vasospasm after subarachnoid hemorrhage. J Neuroinflammation 10:83. doi:10.1186/1742-2094-10-83
Tharakan B, Hunter FA, Smythe WR, Childs EW (2010) Curcumin inhibits reactive oxygen species formation and vascular hyperpermeability following haemorrhagic shock. Clin Exp Pharmacol Physiol 37(9):939–944. doi:10.1111/j.1440-1681.2010.05414.x
Fu XY, Yang MF, Cao MZ, Li DW, Yang XY, Sun JY, Zhang ZY, Mao LL et al (2014) Strategy to suppress oxidative damage-induced neurotoxicity in PC12 cells by curcumin: the role of ROS-mediated DNA damage and the MAPK and AKT pathways. Mol Neurobiol. doi:10.1007/s12035-014-9021-1
Acknowledgments
The national natural science foundation of China (NSFC) (nos.81301018, 81501106, and 81271275) and the China Postdoctoral Science Foundation Grant (2014 M560355) supported this work.
Contributors
ZZ, CF, and BS conceived the project and designed experiments. ZZ, MJ, JF, MY, ZS, YY, DL, FX, WK, HY, and LM performed the experiments; CF and BS analyzed the results. ZZ and CF wrote the manuscript. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Zong-yong Zhang, Ming Jiang and Jie Fang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Zhang, Zy., Jiang, M., Fang, J. et al. Enhanced Therapeutic Potential of Nano-Curcumin Against Subarachnoid Hemorrhage-Induced Blood–Brain Barrier Disruption Through Inhibition of Inflammatory Response and Oxidative Stress. Mol Neurobiol 54, 1–14 (2017). https://doi.org/10.1007/s12035-015-9635-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-015-9635-y