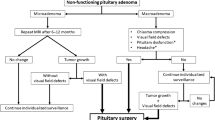
Abstract
There is a lack of evidence on timing, frequency, and duration of postoperative endocrine, radiologic, and ophthalmologic assessments that should be performed after pituitary surgery (PS). However, it is known that careful optimization of treatment and follow-up strategies as well as a multidisciplinary approach may have a significant impact on long-term outcomes, improving surgical results, minimize complications and facilitate their correct treatment if occurring, and optimize the hormonal, ophthalmological, and radiological reassessment throughout the follow-up. Considering that there are no specific guidelines on the postoperative management of patients with pituitary tumors (PT), we present our protocol for the postoperative management of patients with PT. It has been elaborated by the multidisciplinary team of a Spanish Pituitary Tumor Center of Excellence (PTCE) that includes at least one neurosurgeon, ENT, neuroradiologist, neuro-ophthalmologist, endocrine pathologist and endocrinologist specialized in pituitary diseases. We elaborated this guideline with the aim of sharing our experience with other centers involved in the management of PT thereby facilitating the postoperative management of patients submitted to PS.

Similar content being viewed by others
References
W.A. Hall, M.G. Luciano, J.L. Doppman, N.J. Patronas, E.H. Oldfield, Pituitary magnetic resonance imaging in normal human volunteers: occult adenomas in the general population. Ann. Intern. Med. 120(10), 817–820 (1994)
P.U. Freda, A.M. Beckers, L. Katznelson, M.E. Molitch, V.M. Montori, K.D. Post et al. Pituitary incidentaloma: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 96(4), 894–904 (2011). https://doi.org/10.1210/jc.2010-1048
G. Zada, R. Du, E.R. Laws, Defining the ‘edge of the envelope’: patient selection in treating complex sellar-based neoplasms via transsphenoidal versus open craniotomy. J. Neurosurg. 114(2), 286–300 (2011). https://doi.org/10.3171/2010.8.JNS10520. Epub 2010 Sep 3
A. Tabaee, A. Anand, V.K. Barrón, Y. Hiltzik, D.D.H. Brown, M. Seth et al. Endoscopic pituitary surgery: a systematic review and meta-analysis. J. Neurosurg. 2009. https://doi.org/10.3171/2007.12.17635
M. Ammirati, L. Wei, I. Ciric, Short-term outcome of endoscopic versus microscopic pituitary adenoma surgery: a systematic review and meta-analysis. J. Neurol. Neurosurg. Psychiatry 84(8), 843–849 (2013). https://doi.org/10.1136/jnnp-2012-303194. Epub 2012 Dec 15
R.D. Almutairi, I.S. Muskens, D.J. Cote, M.D. Dijkman, V.K. Kavouridis, E. Crocker et al. Gross total resection of pituitary adenomas after endoscopic vs. microscopic transsphenoidal surgery: a meta-analysis. Acta Neurochir. 160(5), 1005–1021 (2018). https://doi.org/10.1007/s00701-017-3438-z. Epub 2018 Jan 6
Y. Gao, C. Zhong, Y. Wang, S. Xu, Y. Guo, C. Dai et al. Endoscopic versus microscopic transsphenoidal pituitary adenoma surgery: a meta-analysis. World J. Surg. Oncol. 12(4), 94 (2014). https://doi.org/10.1186/1477-7819-12-94
M.E. Molitch, Diagnosis and treatment of pituitary adenomas: a review. JAMA 317(5), 516–524 (2017). https://doi.org/10.1001/jama.2016.19699
D.J. Cote, A. Alzarea, M.A. Acosta, M.M. Hulou, K.T. Huang, H. Almutairi et al. Predictors and rates of delayed symptomatic hyponatremia after transsphenoidal surgery: asystemastic review. World Neurosurg. 88, 1–6 (2016). https://doi.org/10.1016/j.wneu.2016.01.022. Epub 2016 Jan 22
W.W. Woodmansee, J. Carmichael, D. Kelly, L. Katznelson, American association of clinical endocrinologists and american college of endocrinology disease state clinical review: postoperative management following pituitary surgery. Endocr. Pract. 21(7), 832–838 (2015). https://doi.org/10.4158/EP14541.DSCR
J. Estrada, J. García-Uría, C. Lamas, J. Alfaro, T. Lucas, S. Diez et al. The complete normalization of the adrenocortical function as the criterion of cure after transsphenoidal surgery for Cushing’s disease. J. Clin. Endocrinol. Metab. 86(12), 5695–5699 (2001)
J. Newell-Price, Transsphenoidal surgery for Cushing’s disease: defining cure and following outcome. Clin. Endocrinol. 56(1), 19–21 (2002)
L.B. Yap, H.E. Turner, C.B.T. Adams, J.A.H. Wass, Undetectable postoperative cortisol does not always predict long-term remission in Cushing’s disease: a single centre audit. Clin. Endocrinol. 56(1), 25–31 (2002)
L. Katznelson, E.R. Laws Jr, S. Melmed, M.E. Molitch, M.H. Murad, A. Utz et al. Acromegaly: an endocrine society clinical practice guidelinesummary of recommendations. J. Clin. Endocrinol. Metab. 99(11), 3933–3951 (2014). https://doi.org/10.1210/jc.2014-2700. Epub 2014 Oct 30
E.H. Kim, M.C. Oh, E.J. Lee, S.H. Kim, Predicting long-term remission by measuring immediate postoperative growth hormone levels and oral glucose tolerance test in acromegaly. Neurosurgery 70(5), 1106–1113 (2012). https://doi.org/10.1227/NEU.0b013e31823f5c16. discussion 1113
A. Jahangiri, J. Wagner, S.W. Han, M.T. Tran, L.M. Miller, M.W. Tom et al. Rate and time course of improvement in endocrine function after more than 1000 pituitary operations. Neurosurgery 61(Suppl 1), 163–166 (2014). https://doi.org/10.1227/NEU.0000000000000405
F.F. Casanueva, A.L. Barkan, M. Buchfelder, A. Klibanski, E.R. Laws, J.S. Loeffler et al. Criteria for the definition of Pituitary Tumor Centers of Excellence (PTCOE): a Pituitary Society statement. Pituitary 20(5), 489–498 (2017). https://doi.org/10.1007/s11102-017-0838-2
I. Ciric, A. Ragin, C. Baumgartner, D. Pierce, Complications of transsphenoidal surgery: Results of a national survey, review of the literature, and personal experience. Neurosurgery 40(2), 225–236 (1997)
F.G. Barker, A. Klibanski, B. Swearingen, Transsphenoidal surgery for pituitary tumors in the United States, 1996-2000: mortality, morbidity, and the effects of hospital and surgeon volume. J. Clin. Endocrinol. Metab. 88(10), 4709–4719 (2003)
K. Shahlaie, N. McLaughlin, A.B. Kassam, D.F. Kelly, The role of outcomes data for assessing the expertise of a pituitary surgeon. Curr. Opin. Endocrinol. Diabetes Obes. 17(4), 369–376 (2010). https://doi.org/10.1097/MED.0b013e32833abcba
P. Iglesias, V. Rodríguez Berrocal, J.J. Díez, Giant pituitary adenoma: histological types, clinical features and therapeutic approaches. Endocrine 61(3), 407–421 (2018). https://doi.org/10.1007/s12020-018-1645-x. Epub 2018 Jun 16
T.R. Deklotz, S.H. Chia, W. Lu, K.H. Makambi, E. Aulisi, Z. Deeb, Meta-analysis of endoscopic versus sublabial pituitary surgery. Laryngoscope 122(3), 511–518 (2012). https://doi.org/10.1002/lary.22479. Epub 2012 Jan 17
S. Dhandapani, H. Singh, H.M. Negm, S. Cohen, V.K. Anand, T.H. Schwartz, Cavernous sinus invasion in pituitary adenomas: systematic review and pooled data meta-analysis of radiologic criteria and comparison of endoscopic and microscopic surgery. World Neurosurg. 96, 36–46 (2016). https://doi.org/10.1016/j.wneu.2016.08.088. Epub 2016 Aug 30
B. Rotenberg, S. Tam, W.H.A. Ryu, N. Duggal, Microscopic versus endoscopic pituitary surgery: a systematic review. Laryngoscope 120(7), 1292–1297 (2010). https://doi.org/10.1002/lary.20949
K. Phan, J. Xu, R. Reddy, P. Kalakoti, A. Nanda, J. Fairhall, Endoscopic endonasal versus microsurgical transsphenoidal approach for growth hormone–secreting pituitary adenomas—systematic review and meta-analysis. World Neurosurg. 97, 398–406 (2017). https://doi.org/10.1016/j.wneu.2016.10.029. Epub 2016 Oct 15
L.H.A. Broersen, N.R. Biermasz, W.R. van Furth, F. de Vries, M.J.T. Verstegen, O.M. Dekkers et al. “Endoscopic vs. microscopic transsphenoidal surgery for Cushing’s disease: a systematic review and meta-analysis. Pituitary 21(5), 524–534 (2018). https://doi.org/10.1007/s11102-018-0893-3
R.J. Komotar, R.M. Starke, D.M.S. Raper, V.K. Anand, T.H. Schwartz, Endoscopic endonasal compared with microscopic transsphenoidal and open transcranial resection of giant pituitary adenomas. Pituitary 15(2), 150–159 (2012). https://doi.org/10.1007/s11102-011-0359-3
Y. Esquenazi, W.I. Essayed, H. Singh, E. Mauer, M. Ahmed, P.J. Christos et al. Endoscopic endonasal versus microscopic transsphenoidal surgery for recurrent and/or residual pituitary adenomas. World Neurosurg. 101, 186–195 (2017). https://doi.org/10.1016/j.wneu.2017.01.110. Epub 2017 Feb 6
J.K. Goudakos, K.D. Markou, C. Georgalas, Endoscopic versus microscopic trans-sphenoidal pituitary surgery: a systematic review and meta-analysis. Clin. Otolaryngol. 36(3), 212–220 (2011). https://doi.org/10.1111/j.1749-4486.2011.02331.x
J. Strychowsky, S. Nayan, K. Reddy, F. Farrokhyar, D. Sommer, Purely endoscopic transsphenoidal surgery versus traditional microsurgery for resection of pituitary adenomas: systematic review. J. Otolaryngol. Head. Neck Surg. 40(2), 175–185 (2011)
J. Coburger, R. König, K. Seitz, U. Bäzner, C.R. Wirtz, M. Hlavac, Determining the utility of intraoperative magnetic resonance imaging for transsphenoidal surgery: a retrospective study. J. Neurosurg. 120(2), 346–356 (2014). https://doi.org/10.3171/2013.9.JNS122207. Epub 2013 Dec 13
S. Berkmann, S. Schlaffer, C. Nimsky, R. Fahlbusch, M. Buchfelder, Intraoperative high-field MRI for transsphenoidal reoperations of nonfunctioning pituitary adenoma. J. Neurosurg. 121(5), 1166–1175 (2014). https://doi.org/10.3171/2014.6.JNS131994. Epub 2014 Aug 15
D. Esposito, D.S. Olsson, O. Ragnarsson, M. Buchfelder, T. Skoglund, G. Johannsson, Non-functioning pituitary adenomas: indications for pituitary surgery and post-surgical management. Pituitary 22(4), 422–434 (2019). https://doi.org/10.1007/s11102-019-00960-0
W.W. Woodmansee, J. Carmichael, D. Kelly, L. Katznelson, American association of clinical endocrinologists and american college of endocrinology disease state clinical review: postoperative management following pituitary surgery. Endocr. Pract. 21(7), 832–838 (2015). https://doi.org/10.4158/EP14541.DSCR
C. Meco, G. Oberascher, E. Arrer, G. Moser, K. Albegger, β-trace protein test: new guidelines for the reliable diagnosis of cerebrospinal fluid fistula. Otolaryngol. Head. Neck Surg. 129(5), 508–517 (2003)
I. Singer, J.R. Oster, L.M. Fishman, The management of diabetes insipidus in adults. Arch. Intern. Med. 157(12), 1293–1301 (1997)
R. Pivonello, M. De Leo, A. Cozzolino, A. Colao, The treatment of cushing’s disease. Endocr. Rev. 36(4), 385–486 (2015). https://doi.org/10.1210/er.2013-1048. Epub 2015 Jun 11
E.C. Nemergut, Z. Zuo, J.A. Jane, E.R. Laws, Predictors of diabetes insipidus after transsphenoidal surgery: a review of 881 patients. J. Neurosurg. 103(3), 448–454 (2005)
J.A. Loh, J.G. Verbalis, Diabetes insipidus as a complication after pituitary surgery. Nat. Clin. Pract. Endocrinol. Metab. 3(6), 489–494 (2007)
J. Hensen, A. Henig, R. Fahlbusch, M. Meyer, M. Boehnert, M. Buchfelder, Prevalence, predictors and patterns of postoperative polyuria and hyponatraemia in the immediate course after transsphenoidal surgery for pituitary adenomas. Clin. Endocrinol. 50(4), 431–439 (1999)
K. Eguchi, T. Uozumi, K. Arita, K. Kurisu, T. Yano, M. Sumida et al. Pituitary function in patients with rathke’s cleft cyst: significance of surgical management. Endocr. J. 41(5), 535–540 (1994)
P. Mortini, M. Losa, G. Pozzobon, R. Barzaghi, M. Riva, S. Acerno et al. Neurosurgical treatment of craniopharyngioma in adults and children: early and long-term results in a large case series. J. Neurosurg. 114(5), 1350–1359 (2011). https://doi.org/10.3171/2010.11.JNS10670. Epub 2011 Jan 7
I. Halac, D. Zimmerman, Endocrine manifestations of craniopharyngioma. Childs Nerv. Syst. 21(8–9), 640–648 (2005). Epub 2005 Jul 27
W. Fenske, B. Allolio, Current state and future perspectives in the diagnosis of diabetes insipidus: a clinical review. J. Clin. Endocrinol. Metab. 97(10), 3426–3437 (2012). https://doi.org/10.1210/jc.2012-1981. Epub 2012 Aug 1
J.A. Loh, J.G. Verbalis, Disorders of water and salt metabolism associated with pituitary disease. Endocrinol. Metab. Clin. North Am. 37(1), 213–234 (2008). https://doi.org/10.1016/j.ecl.2007.10.008
B.R. Olson, D. Rubino, J. Gumowski, E.H. Oldfield, Isolated hyponatremia after transsphenoidal pituitary surgery. J. Clin. Endocrinol. Metab. 80(1), 85–91 (1995)
S. Barber, B. Liebelt, D. Baskin, Incidence, etiology and outcomes of hyponatremia after transsphenoidal surgery: experience with 344 consecutive patients at a Single Tertiary Center. J. Clin. Med. 3(4), 1199–1219 (2014). https://doi.org/10.3390/jcm3041199
G. Spasovski, R. Vanholder, B. Allolio, D. Annane, S. Ball, D. Bichet et al. Clinical practice guideline on diagnosis and treatment of hyponatraemia. Nephrol. Dial. Transplant. 29(Suppl 2), i1–i39 (2014). https://doi.org/10.1093/ndt/gfu040. Epub 2014 Feb 25
W.T. Burke, D.J. Cote, S.I. Iuliano, H.A. Zaidi, E.R. Laws, A practical method for prevention of readmission for symptomatic hyponatremia following transsphenoidal surgery. Pituitary 21(1), 25–31 (2018)
C.E. Taplin, C.T. Cowell, M. Silink, G.R. Ambler, Fludrocortisone therapy in cerebral salt wasting. Pediatrics 118(6), e1904–e1908 (2006). Epub 2006 Nov 13
R. Guerrero, A. Pumar, A. Soto, M.A. Pomares, S. Palma, M.A. Mangas et al. Early hyponatraemia after pituitary surgery: Cerebral salt-wasting syndrome. Eur. J. Endocrinol. 156(6), 611–616 (2007)
S.L. Atkin, A.M. Coady, M.C. White, B. Mathew, Hyponatraemia secondary to cerebral salt wasting syndrome following routine pituitary surgery. Eur. J. Endocrinol. 135(2), 245–247 (1996)
M. Fleseriu, I.A. Hashim, N. Karavitaki, S. Melmed, M.H. Murad, R. Salvatori et al. Hormonal replacement in hypopituitarism in adults: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 101(11), 3888–3921 (2016). Epub 2016 Oct 13
A.C. Lo, A.F. Howard, A. Nichol, K. Sidhu, F. Abdulsatar, H. Hasan et al. Long-term outcomes and complications in patients with craniopharyngioma: The British Columbia cancer agency experience. Int J. Radiat. Oncol. Biol. Phys. 88(5), 1011–1018 (2014). https://doi.org/10.1016/j.ijrobp.2014.01.019
F. Roelfsema, N.R. Biermasz, A.M. Pereira, Clinical factors involved in the recurrence of pituitary adenomas after surgical remission: a structured review and meta-analysis. Pituitary 15(1), 71–83 (2012). https://doi.org/10.1007/s11102-011-0347-7
J.F. Bonneville, F. Bonneville, F. Cattin, S. Nagi, MRI of the pituitary gland:indications and results in gynaecology and in obstetrics. Gynecol. Obstet. Fertil. 33(3), 147–153 (2005)
A. Wolf, A. Coros, J. Bierer, S. Goncalves, P. Cooper, S. Van Uum et al. Quantitative evaluation of vision-related and health-related quality of life after endoscopic transsphenoidal surgery for pituitary adenoma. J. Neurosurg. 127(2), 409–416 (2017). https://doi.org/10.3171/2016.7.JNS16200. Epub 2016 Oct 7
J.B. Kerrison, M.J. Lynn, C.A. Baer, S.A. Newman, V. Biousse, N.J. Newman, Stages of improvement in visual fields after pituitary tumor resection. Am. J. Ophthalmol. 130(6), 813–820 (2000)
Y.H. Kim, Y.H. Cho, S.H. Hong, J.H. Kim, M.S. Kim, S.K. Khang et al. Postoperative neurologic outcome in patients with pituitary apoplexy after transsphenoidal surgery. World Neurosurg. 111, e18–e23 (2018). https://doi.org/10.1016/j.wneu.2017.11.124. Epub 2017 Nov 28
C. Cortet-Rudelli, J.F. Bonneville, F. Borson-Chazot, L. Clavier, B. Coche Dequéant, R. Desailloud et al. Post-surgical management of non-functioning pituitary adenoma. Ann. Endocrinol. 76(3), 228–238 (2015). https://doi.org/10.1016/j.ando.2015.04.003. Epub 2015 Jun 23
A.W., D.F., Z.R., N.M., A.A., Endoscopic skull base reconstruction with the use of the nasoseptal flap: the tasmc experience. J. Neurol. Surg. B 77, FP-04-01 (2016). https://doi.org/10.1055/s-0036-1592452
L.X. Yin, C.M. Low, C.L. Puccinelli, E.K. O'Brien, J.K. Stokken, K.M. Van Abel et al. Olfactory outcomes after endoscopic skull base surgery: a systematic review and meta-analysis. Laryngoscope 129(9), 1998–2007 (2019). https://doi.org/10.1002/lary.28003. Epub 2019 Apr 29
S.L. Asa, O. Casar-Borota, P. Chanson, E. Delgrange, P. Earls, S. Ezzat et al. From pituitary adenoma to pituitary neuroendocrine tumor (pitnet): an international pituitary pathology club proposal. Endocr. Relat. Cancer 24(4), C5–C8 (2017). https://doi.org/10.1530/ERC-17-0004
R.V. Lloyd, R.Y. Osamura, G. Klöppel, J Rosai, Pathology and Genetics of Tumours of Endocrine Organs. Fourth edition. IARC WHO Classification of Tumours. Vol 10. (2017)
J. Trouillas, P. Roy, N. Sturm, E. Dantony, C. Cortet-Rudelli, G. Viennet et al. A new prognostic clinicopathological classification of pituitary adenomas: a multicentric case-control study of 410 patients with 8 years post-operative follow-up. Acta Neuropathol. 126(1), 123–135 (2013). https://doi.org/10.1007/s00401-013-1084-y. Epub 2013 Feb 12
C.P. Miermeister, S. Petersenn, M. Buchfelder, R. Fahlbusch, D.K. Lüdecke, A. Hölsken et al. Histological criteria for atypical pituitary adenomas—data from the German pituitary adenoma registry suggests modifications. Acta Neuropathol. Commun. 3, 50 (2015). https://doi.org/10.1186/s40478-015-0229-8
E. Manojlovic-Gacic, J. Bollerslev, and O. Casar-Borota. Invited Review: Pathology of pituitary neuroendocrine tumours: present status, modern diagnostic approach, controversies and future perspectives from a neuropathological and clinical standpoint. Neuropathol Appl Neurobiol. 2019. https://doi.org/10.1111/nan.12568
G. Raverot, P. Burman, A. McCormack, A. Heaney, S. Petersenn, V. Popovic et al. European society of endocrinology clinical practice guidelines for the management of aggressive pituitary tumours and carcinomas. Eur. J. Endocrinol. 178(1), G1–G24 (2018). https://doi.org/10.1530/EJE-17-0796. Epub 2017 Oct 18
P.J. Trainer, H.S. Lawrie, J. Verhelst, T.A. Howlett, D.G. Lowe, A.B. Grossman et al. Transsphenoidal resection in Cushing’s disease: undetectable serum cortisol as the definition of successful treatment. Clin. Endocrinol. 38(1), 73–78 (1993)
D.R. McCance, D.S. Gordon, T.F. Fannin, D.R. Hadden, L. Kennedy et al. Assessment of endocrine function after transsphenoidal surgery for Cushing’s disease. Clin. Endocrinol. 38(1), 79–86 (1993)
D.R. McCance, M. Besser, A.B. Atkinson, Assessment of cure after transsphenoidal surgery for Cushing’s disease. Clin. Endocrinol. 44(1), 1–6 (1996)
B.M. Biller, A.B. Grossman, P.M. Stewart, S. Melmed, X. Bertagna, J. Bertherat et al. Treatment of adrenocorticotropin-dependent cushing’s syndrome: a consensus statement. J. Clin. Endocrinol. Metab. 93(7), 2454–2462 (2008). https://doi.org/10.1210/jc.2007-2734. Epub 2008 Apr 15
R. Pivonello, M.C. De Martino, M. De Leo, L. Tauchmanovà, A. Faggiano, G. Lombardi et al. Cushing’s syndrome: aftermath of the cure. Arq. Bras. Endocrinol. Metabol. 51(8), 1381–1391 (2007)
N.A. Tritos, B.M.K. Biller, B. Swearingen, Management of Cushing disease. Nat. Rev. Endocrinol. 7(5), 279–289 (2011). https://doi.org/10.1038/nrendo.2011.12. Epub 2011 Feb 8
C. Beauregard, G. Dickstein, A. Lacroix, Classic and recent etiologies of Cushing’s syndrome: diagnosis and therapy. Treat. Endocrinol. 1(2), 79–94 (2002)
M.A. Czepielewski, G.A.F.S. Rollin, A. Casagrande, N.P. Ferreira, Criteria of cure and remission in Cushing’s disease: an update. Arq. Bras. Endocrinol. Metabol. 51(8), 1362–1372 (2007)
A. Ayala, A.J. Manzano, Detection of recurrent Cushing’s disease: proposal for standardized patient monitoring following transsphenoidal surgery. J. Neurooncol. 119(2), 235–242 (2014). https://doi.org/10.1007/s11060-014-1508-0. Epub 2014 Jul 1
R.M. Salassa, E.R. Laws, P.C. Carpenter, R.C. Northcutt, Transsphenoidal removal of pituitary microadenoma in Cushing’s disease. Mayo Clin. Proc. 53(1), 24–28 (1978)
P.C. Carpenter, Cushing’s syndrome: update of diagnosis and management. Mayo Clin. Proc. 61(1), 49–58 (1986)
Z. Ram, L.K. Nieman, G.B. Cutler, G.P. Chrousos, J.L. Doppman, E.H. Oldfield, Early repeat surgery for persistent Cushing’s disease. J. Neurosurg. 80(1), 37–45 (1994)
F. Esposito, J.R. Dusick, P. Cohan, P. Moftakhar, D. McArthur, C. Wang et al. Clinical review: Early morning cortisol levels as a predictor of remission after transsphenoidal surgery for Cushing’s disease. J. Clin. Endocrinol. Metab. 91(1), 7–13 (2006). Epub 2005 Oct 18
D. Bochicchio, M. Losa, M. Buchfelder, Factors influencing the immediate and late outcome of Cushing’s disease treated by transsphenoidal surgery: a retrospective study by the European Cushing’s Disease Survey Group. J. Clin. Endocrinol. Metab. 80(11), 3114–3120 (1995)
A.M. Pereira, M.O. van Aken, H. van Dulken, P.J. Schutte, N.R. Biermasz, J.W. Smit et al. Long-term predictive value of postsurgical cortisol concentrations for cure and risk of recurrence in Cushing’s disease. J. Clin. Endocrinol. Metab. 88(12), 5858–5864 (2003)
A.L. Serban, E. Sala, G. Carosi, G. Del Sindaco, C. Giavoli, M. Locatelli et al. Recovery of adrenal function after pituitary surgery in patients with Cushing disease: persistent remission or recurrence? Neuroendocrinology 108(3), 211–218 (2019). https://doi.org/10.1159/000496846. Epub 2019 Jan 13
A.B. Atkinson, A. Kennedy, M.I. Wiggam, D.R. McCance, B. Sheridan, Long-term remission rates after pituitary surgery for Cushing’s disease: the need for long-term surveillance. Clin. Endocrinol. 63(5), 549–559 (2005)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Araujo-Castro, M., Pascual-Corrales, E., Martínez San Millan, J.S. et al. Postoperative management of patients with pituitary tumors submitted to pituitary surgery. Experience of a Spanish Pituitary Tumor Center of Excellence. Endocrine 69, 5–17 (2020). https://doi.org/10.1007/s12020-020-02247-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02247-y