Abstract
Hepatocellular carcinoma (HCC) is the most common form of liver cancer, occurring primarily in regions where viral hepatitis infections are common. Unfortunately, most HCC cases remain undiagnosed until late stages of the disease when patient outcome is poor, typically limiting survival from a few months to a year after initial diagnosis. In order to better care for HCC patients, new target-specific approaches are needed to improve early detection and therapeutic intervention. In this work, polymeric nanoparticles functionalized with a HCC-specific aptamer were examined as potential targeted drug delivery vehicles. Specifically, doxorubicin-loaded nanoparticles were prepared via nanoprecipitation of blends of poly(lactic-co-glycolic acid)-b-poly(ethylene glycol). These particles were further functionalized with the HCC-specific TLS11a aptamer. The in vitro interaction and therapeutic efficacy of the aptamer and aptamer-functionalized nanoparticles were characterized in a hepatoma cell line. Nanoparticles were found to be spherical in shape, roughly 100–125 nm in diameter, with a low polydispersity (≤0.2) and slightly negative surface potential. Doxorubicin was encapsulated within the particles at ~40 % efficiency. Drug release was found to occur through anomalous transport influenced by diffusion and polymer relaxation, releasing ~50 % doxorubicin in the first 10 h and full release occurring within 36 h. Confocal microscopy confirmed binding and attachment of aptamer-targeted nanoparticles to the cell surface of cultured HCC cells. Efficacy studies demonstrated a significant improvement in doxorubicin delivery and cell-killing capacity using the aptamer-functionalized, drug-loaded nanoparticles versus controls further supporting use of aptamer nanoparticles as a targeted drug delivery system for HCC tumors.

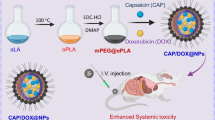
In this work, polymeric nanoparticles functionalized with a liver cancer-specific aptamer were examined as potential targeted drug delivery vehicles. The aptamer-functionalized nanoparticles were found to significantly improve doxorubicin drug delivery and cell-killing capacity in vitro versus non-targeted controls, supporting their use as a targeted treatment toward liver cancer tumors.






Similar content being viewed by others
References
American Cancer Society (2016) Cancer facts & figures 2016.
Attwa MH (2015) Guide for diagnosis and treatment of hepatocellular carcinoma world. J Hepatol 7:1632–1632. doi:10.4254/wjh.v7.i12.1632
Avgoustakis K (2004) Pegylated poly(lactide) and poly(lactide-co-glycolide) nanoparticles: preparation, properties and possible applications in drug delivery. Curr Drug Deliv 1:321–333
Bareford LM, Swaan PW (2007) Endocytic mechanisms for targeted drug delivery. Adv Drug Deliv Rev 59:748–758. doi:10.1016/j.addr.2007.06.008
Betancourt T, Brown B, Brannon-Peppas L (2007) Doxorubicin-loaded PLGA nanoparticles by nanoprecipitation: preparation, characterization and in vitro evaluation. Nanomedicine (Lond) 2:219–232. doi:10.2217/17435889.2.2.219
Betancourt T et al (2009) PEGylation strategies for active targeting of PLA/PLGA nanoparticles. J Biomed Mater Res A 91:263–276. doi:10.1002/jbm.a.32247
Bruix J et al (2015) Adjuvant sorafenib for hepatocellular carcinoma after resection or ablation (STORM): a phase 3, randomised, double-blind, placebo-controlled trial. The Lancet Oncology 16:1344–1354. doi:10.1016/S1470-2045(15)00198-9
Byrne JD, Betancourt T, Brannon-Peppas L (2008) Active targeting schemes for nanoparticle systems in cancer therapeutics. Adv Drug Deliv Rev 60:1615–1626. doi:10.1016/j.addr.2008.08.005
Danhier F, Feron O, Préat V (2010) To exploit the tumor microenvironment: passive and active tumor targeting of nanocarriers for anti-cancer drug delivery. 148. doi:10.1016/j.jconrel.2010.08.027
Danquah MK, Zhang XA, Mahato RI (2011) Extravasation of polymeric nanomedicines across tumor vasculature. Adv Drug Deliv Rev 63:623–639. doi:10.1016/j.addr.2010.11.005
Dhanasekaran R, Limaye A, Cabrera R (2012) Hepatocellular carcinoma: current trends in worldwide epidemiology, risk factors, diagnosis, and therapeutics. Hepatic medicine : evidence and research 4:19–37. doi:10.2147/HMER.S16316
Dhar S, Gu FX, Langer R, Farokhzad OC, Lippard SJ (2008) Targeted delivery of cisplatin to prostate cancer cells by aptamer functionalized Pt(IV) prodrug-PLGA-PEG nanoparticles. Proc Natl Acad Sci U S A 105:17356–17361. doi:10.1073/pnas.0809154105
Durymanov MO, Rosenkranz AA, Sobolev AS (2015) Current approaches for improving intratumoral accumulation and distribution of nanomedicines. Theranostics 5:1007–1020. doi:10.7150/thno.11742
Ellington AD, Szostak JW (1990) In vitro selection of RNA molecules that bind specific ligands. Nature 346:818–822. doi:10.1038/346818a0
Farokhzad OC et al (2006) Targeted nanoparticle-aptamer bioconjugates for cancer chemotherapy in vivo. Proc Natl Acad Sci U S A 103:6315–6320. doi:10.1073/pnas.0601755103
Farokhzad OC, Jon S, Khademhosseini A, Tran TN, Lavan DA, Langer R (2004) Nanoparticle-aptamer bioconjugates: a new approach for targeting prostate cancer cells. Cancer Res 64:7668–7672. doi:10.1158/0008-5472.CAN-04-2550
Ferlay J et al (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136:E359–E386. doi:10.1002/ijc.29210
Forner A, Llovet JM, Bruix J (2012) Hepatocellular carcinoma. Lancet 379:1245–1255. doi:10.1016/S0140-6736(11)61347-0
Gewirtz DA (1999) A critical evaluation of the mechanisms of action proposed for the antitumor effects of the anthracycline antibiotics adriamycin and daunorubicin. Biochem Pharmacol 57:727–741
Gref R et al (2000) “Stealth” corona-core nanoparticles surface modified by polyethylene glycol (PEG): influences of the corona (PEG chain length and surface density) and of the core composition on phagocytic uptake and plasma protein adsorption. Colloids Surf B Biointerfaces 18:301–313
Hainfeld JF, O'Connor MJ, Dilmanian FA, Slatkin DN, Adams DJ, Smilowitz HM (2011) Micro-CT enables microlocalisation and quantification of Her2-targeted gold nanoparticles within tumour regions. Br J Radiol 84:526–533. doi:10.1259/bjr/42612922
Huang HS, Hainfeld JF (2013) Intravenous magnetic nanoparticle cancer hyperthermia. Int J Nanomedicine 8:2521–2532. doi:10.2147/IJN.S43770
Jiang J, Chen H, Yu C, Zhang Y, Chen M, Tian S, Sun C (2015) The promotion of salinomycin delivery to hepatocellular carcinoma cells through EGFR and CD133 aptamers conjugation by PLGA nanoparticles. Nanomedicine (Lond) 10:1863–1879. doi:10.2217/nnm.15.43
Kamaly N, Xiao Z, Valencia PM, Radovic-Moreno AF, Farokhzad OC (2012) Targeted polymeric therapeutic nanoparticles: design, development and clinical translation. Chem Soc Rev 41:2971–3010. doi:10.1039/c2cs15344k
Kashefi-Kheyrabadi L, Mehrgardi MA, Wiechec E, Turner APF, Tiwari A (2014) Ultrasensitive detection of human liver hepatocellular carcinoma cells using a label-free aptasensor. Anal Chem 86:4956–4960. doi:10.1021/ac500375p
Kaszuba M, Corbett J, Watson FM, Jones A (2010) High-concentration zeta potential measurements using light-scattering techniques. Philos Trans A Math Phys Eng Sci 368:4439–4451. doi:10.1098/rsta.2010.0175
Knox JJ, Cleary SP, Dawson LA (2015) Localized and systemic approaches to treating hepatocellular carcinoma. Journal of clinical oncology : official journal of the American Society of Clinical Oncology 33:1835–1844. doi:10.1200/JCO.2014.60.1153
Llovet JM et al (2008) Sorafenib in advanced hepatocellular carcinoma. N Engl J Med 359:378–390. doi:10.1056/NEJMoa0708857
Maeda H, Nakamura H, Fang J (2013) The EPR effect for macromolecular drug delivery to solid tumors: improvement of tumor uptake, lowering of systemic toxicity, and distinct tumor imaging in vivo. Adv Drug Deliv Rev 65:71–79. doi:10.1016/j.addr.2012.10.002
McDonald DM, Baluk P (2002) Significance of blood vessel leakiness in cancer. Cancer Res 62:5381–5385
Mehvar R (2000) Modulation of the pharmacokinetics and pharmacodynamics of proteins by polyethylene glycol conjugation. J Pharm Pharm Sci 3:125–136
Meng HM, Fu T, Zhang XB, Tan W (2015) Cell-SELEX-based aptamer-conjugated nanomaterials for cancer diagnosis and therapy. National Science Review 2:71–84. doi:10.1093/nsr/nwv001
Meng L, Yang L, Zhao X, Zhang L, Zhu H, Liu C, Tan W (2012) Targeted delivery of chemotherapy agents using a liver cancer-specific aptamer. PLoS One 7:e33434. doi:10.1371/journal.pone.0033434
Minotti G, Menna P, Salvatorelli E, Cairo G, Gianni L (2004) Anthracyclines: molecular advances and pharmacologic developments in antitumor activity and cardiotoxicity. Pharmacol Rev 56:185–229. doi:10.1124/pr.56.2.6
Onda N, Kemmochi S, Morita R, Ishihara Y, Shibutani M (2013) In vivo imaging of tissue-remodeling activity involving infiltration of macrophages by a systemically administered protease-activatable probe in colon cancer tissues. Transl Oncol 6:628–637
Otsuka H, Nagasaki Y, Kataoka K (2003) PEGylated nanoparticles for biological and pharmaceutical applications. Adv Drug Deliv Rev 55:403–419
Pilapong C, Sitthichai S, Thongtem S, Thongtem T (2014) Smart magnetic nanoparticle-aptamer probe for targeted imaging and treatment of hepatocellular carcinoma. Int J Pharm 473:469–474. doi:10.1016/j.ijpharm.2014.07.036
Prencipe G et al (2009) PEG branched polymer for functionalization of nanomaterials with ultralong blood circulation. J Am Chem Soc 131:4783–4787. doi:10.1021/ja809086q
Qu L, Xu J, Tan X, Liu Z, Xu L, Peng R (2014) Dual-aptamer modification generates a unique Interface for highly sensitive and specific electrochemical detection of tumor cells. ACS Appl Mater Interfaces 6:7309–7315. doi:10.1021/am5006783
Ritger PL, Peppas NA (1987) A simple equation for description of solute release I. Fickian and non-fickian release from non-swellable devices in the form of slabs, spheres, cylinders or discs. J Control Release 5:23–36. doi:10.1016/0168-3659(87)90034-4
Shangguan D et al (2008) Identification of liver cancer-specific aptamers using whole live cells. Anal Chem 80:721–728. doi:10.1021/ac701962v
Siepmann J, Peppas NA (2001) Modeling of drug release from delivery systems based on hydroxypropyl methylcellulose (HPMC). Adv Drug Deliv Rev 48:139–157
Stoltenburg R, Reinemann C, Strehlitz B (2007) SELEX—a (r)evolutionary method to generate high-affinity nucleic acid ligands. Biomol Eng 24:381–403. doi:10.1016/j.bioeng.2007.06.001
Sun D, Lu J, Chen Z, Yu Y, Mo M (2015) A repeatable assembling and disassembling electrochemical aptamer cytosensor for ultrasensitive and highly selective detection of human liver cancer cells. Anal Chim Acta 885:166–173. doi:10.1016/j.aca.2015.05.027
Sun D, Lu J, Zhong Y, Yu Y, Wang Y, Zhang B, Chen Z (2016) Sensitive electrochemical aptamer cytosensor for highly specific detection of cancer cells based on the hybrid nanoelectrocatalysts and enzyme for signal amplification. Biosens Bioelectron 75:301–307. doi:10.1016/j.bios.2015.08.056
Sun H, Zhu X, Lu PY, Rosato RR, Tan W, Zu Y (2014) Oligonucleotide aptamers: new tools for targeted cancer therapy. Molecular therapy Nucleic acids 3:e182–e182. doi:10.1038/mtna.2014.32
Torchilin VP, Trubetskoy VS (1995) Which polymers can make nanoparticulate drug carriers long-circulating. Adv Drug Deliv Rev 16:141–155. doi:10.1016/0169-409x(95)00022-Y
Wang H, Wang F, Tao X, Cheng H (2012) Ammonia-containing dimethyl sulfoxide: an improved solvent for the dissolution of formazan crystals in the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl tetrazolium bromide (MTT) assay. Anal Biochem 421:324–326. doi:10.1016/j.ab.2011.10.043
Weigum SE, Sutton M, Barnes E, Miller S, Betancourt T (2014) Targeting hepatocellular carcinoma with aptamer-functionalized PLGA/PLA-PEG nanoparticles. 9166:916605–916605 doi:10.1117/12.2062283
Xu J et al (2015) Molecular recognition of human liver cancer cells using DNA aptamers generated via cell-SELEX. PLoS One 10:e0125863. doi:10.1371/journal.pone.0125863
Yu D, Zhang Y, Mao Z, Gao C (2013) Study of the selective uptake progress of aptamer-modified PLGA particles by liver cells. Macromol Biosci 13:1413–1421. doi:10.1002/mabi.201300165
Yu MK, Park J, Jon S (2012) Targeting strategies for multifunctional nanoparticles in cancer imaging and therapy. Theranostics 2:3–44. doi:10.7150/thno.3463
Zhang B, Luo Z, Liu J, Ding X, Li J, Cai K (2014) Cytochrome c end-capped mesoporous silica nanoparticles as redox-responsive drug delivery vehicles for liver tumor-targeted triplex therapy in vitro and in vivo. Journal of controlled release : official journal of the Controlled Release Society 192:192–201. doi:10.1016/j.jconrel.2014.06.037
Acknowledgments
This research was supported in part by the Texas Emergent Technology Fund (start-up funds to TB), the Robert A. Welch Foundation (AI-0045), NIGMS South Texas Doctoral Bridge Program (R25-GM102783) fellowship to C. Munoz, and Texas State University (start-up funds to SW).
Author information
Authors and Affiliations
Corresponding authors
Electronic supplementary material
ESM 1
(DOCX 1171 kb)
Rights and permissions
About this article
Cite this article
Weigum, S., McIvor, E., Munoz, C. et al. Targeted therapy of hepatocellular carcinoma with aptamer-functionalized biodegradable nanoparticles. J Nanopart Res 18, 341 (2016). https://doi.org/10.1007/s11051-016-3633-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11051-016-3633-5