Abstract
Objectives
To evaluate the effect of photobiomodulation with low-level laser therapy (PBM-LLLT) combined with 5% potassium nitrate (KNO3) on controlling tooth sensitivity (TS) after in-office tooth bleaching.
Materials and methods
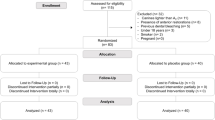
Fifty volunteers were selected based on the inclusion and exclusion criteria and were randomly allocated into four groups: G1 (control): placebo gel application, 35% hydrogen peroxide bleaching (HP35) and mock PBM-LLLT without light emission; G2: placebo gel application, bleaching with HP35 and PBM-LLLT; G3: application of KNO3, bleaching with HP35 and mock PBM-LLLT; and G4: application of KNO3, bleaching with HP35 and PBM-LLLT. A pain assessment questionnaire was used to evaluate TS during the 21 days of treatment. The Friedman test was used for intragroup analysis, and the Wilcoxon and Mann-Whitney tests were used for intergroup comparisons.
Results
The intragroup evaluation showed significant differences among the evaluation times in all groups (p ≤ 0.05). The highest pain sensitivity levels were recorded on the 1st, 8th, and 15th days. In G1, TS manifested for up to 3 days after each bleaching session, while G2, G3, and G4 presented TS only on the days of the bleaching sessions. Intergroup analysis showed that TS manifestation differed significantly between G1 and the other groups (p ≤ 0.05) but did not differ significantly among G2, G3, and G4 (p ≥ 0.05).
Conclusion
PBM-LLLT and KNO3 are effective at reducing pain sensitivity after tooth bleaching, but no synergistic effect between these treatments was observed for the different evaluation periods.
Clinical relevance
The effect of PBM-LLLT combined with KNO3 on post-bleaching tooth sensitivity is similar to their individual use alone.

Similar content being viewed by others
References
Roberson TM, Heymann HO, Swift EJ (2002) Sturdevants art and science of operative dentistry, 4th edn. Elsevier, Missouri, pp 605–612
Tin-Oo MM, Saddki N, Hassan N (2011) Factors influencing patient satisfaction with dental appearance and treatments they desire to improve aesthetics. BMC Oral Health 23:11–16. https://doi.org/10.1186/1472-6831-11-6
Kwon SR, Wertz PW (2015) Review of the mechanism of tooth whitening. J Esthet Restor Dent 27:240–257. https://doi.org/10.1111/jerd.12152
Kawamoto K, Tsujimoto Y (2004) Effects of the hydroxyl radical and hydrogen peroxide on tooth bleaching. J Endod 30:45–50. https://doi.org/10.1097/00004770-200401000-00010
Patri G, Agnihotri Y, Rao SR et al (2013) An in-vitro spectrophotometric analysis of the penetration of bleaching agent into the pulp chamber of intact and restored teeth. J Clin Diagn Res 7:3057–3059. https://doi.org/10.7860/JCDR/2013/7589.3852
Benetti F, Gomes-Filho JE, Ferreira LL, Ervolino E, Briso ALF, Sivieri-Araújo G, Dezan-Júnior E, Cintra LTA (2017) Hydrogen peroxide induces cell proliferation and apoptosis in pulp of rats after dental bleaching in vivo. Arch Oral Biol 81:103–109. https://doi.org/10.1016/j.archoralbio.2017.04.013
Cintra LT, Benetti F, Facundo ACS et al (2013) The number of bleaching sessions influences pulp tissue damage in rat teeth. J Endod 39:1576–1580. https://doi.org/10.1016/j.joen.2013.08.007
Cintra LT, Benetti F, Ferreira LL et al (2016) Penetration capacity color alteration and biological response of two in office bleaching protocols. Braz Dent J 27:169–175. https://doi.org/10.1590/0103-6440201600329
Soares DG, Basso FG, Hebling J, de Souza Costa CA (2015) Immediate and late analysis of dental pulp stem cells viability after indirect exposition to alternative in office bleaching strategies. Clin Oral Investig 19:1013–1020. https://doi.org/10.1007/s00784-014-1321-3
Costa CA, Riehl H, Kina JF et al (2010) Human pulp responses to in-office tooth bleaching. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109:59–64. https://doi.org/10.1016/j.tripleo.2009.12.002
Roderjan DA, Stanislawczuk R, Hebling J et al (2014) Histopathological features of dental pulp tissue from bleached mandibular incisors. Mater Sci Eng B 4:178–185. https://doi.org/10.17265/2161-6221/2014.06.006
Roderjan DA, Stanislawczuk R, Hebling J, Costa CAS, Reis A, Loguercio AD (2015) Response of human pulps to different in-office bleaching techniques: preliminary findings. Braz Dent J 26:242–248 https://doi.org/10.1590/0103-6440201302282
Bonafé E, Bacovis CL, Lesen S et al (2013) Tooth sensitivity and efficacy of in-office bleaching in restored teeth. J Dent 41:363–369. https://doi.org/10.1016/j.jdent.2013.01.007
Soares DG, Ribeiro AP, Vargas FS et al (2013) Efficacy and cytotoxicity of a bleaching gel after short application times on dental enamel. Clin Oral Investig 17:1901–1910. https://doi.org/10.1007/s00784-012-0883-1
Sato C, Rodrigues FA, Garcia D et al (2013) Tooth bleaching increases dentinal protease activity. J Dent Res 92:187–192. https://doi.org/10.1177/0022034512470831
Trindade FZ, Ribeiro AP, Sacono NT et al (2009) Trans-enamel and trans-dentinal cytotoxic effects of a 35% H2O2 bleaching gel on cultured odontoblast cell lines after consecutive applications. Int Endod J 42:516–524. https://doi.org/10.1111/j.1365-2591.2009.01544.x
Cook SP, McCleskey EW (2002) Cell damage excites nociceptors through release of cytosolic ATP. Pain 95:41–47. https://doi.org/10.1016/S0304-3959(01)00372-4
Bowles WR, Withrow JC, Lepinski AM et al (2003) Tissue levels of immunoreactive substance P are increased in patients with irreversible pulpitis. J Endod 29:265–267. https://doi.org/10.1097/00004770-200304000-00009
Huynh MP, Yagiela JA (2003) Current concepts in acute pain management. J Calif Dent Assoc 31:419–427
Cecarini V, Gee J, Fioretti E, Amici M, Angeletti M, Eleuteri AM, Keller JN (2007) Protein oxidation and cellular homeostasis: emphasis on metabolism. Biochim Biophys Acta 1773:93–104. https://doi.org/10.1016/j.bbamcr.2006.08.039
Kossatz S, Martins G, Loguercio AD, Reis A (2012) Tooth sensitivity and bleaching effectiveness associated with use of a calcium-containing in-office bleaching gel. J Am Dent Assoc 143:81–87. https://doi.org/10.14219/jada.archive.2012.0075
Tang B, Millar BJ (2010) Effect of chewing gum on tooth sensitivity following whitening. Br Dent J 208:571–577. https://doi.org/10.1038/sj.bdj.2010.500
Basting RT, Amaral FL, França FM, Flório FM (2012) Clinical comparative study of the effectiveness of and tooth sensitivity to 10% and 20% carbamide peroxide home-use and 35% and 38% hydrogen peroxide in-office bleaching materials containing desensitizing agents. Oper Dent 37:464–473. https://doi.org/10.2341/11-337-C
Palé M, Mayoral JR, Llopis J, Vallès M, Basilio J, Roig M (2014) Evaluation of the effectiveness of an in-office bleaching system and the effect of potassium nitrate as a desensitizing agent. Odontology 102:203–210. https://doi.org/10.1007/s10266-013-0132-3
Markowitz K, Pashley DH (2008) Discovering new treatments for sensitive teeth: the long path from biology to therapy. J Oral Rehabil 35:300–315. https://doi.org/10.1111/j.1365-2842.2007.01798.x
Ladalardo TC, Pinheiro A, Campos RA et al (2004) Laser therapy in the treatment of dentine hypersensitivity. Braz Dent J 15:144–150. https://doi.org/10.1590/S0103-64402004000200011
Wakabayashi H, Hamba M, Matsumoto K, Tachibana H (1993) Effect of irradiation by semiconductor laser on responses evoked in trigeminal caudal neurons by tooth pulp stimulation. Lasers Surg Med 13:605–610. https://doi.org/10.1002/lsm.1900130603
Favaro–Pipi E, Ribeiro DA, Ribeiro JU et al (2011) Low level laser therapy induces differential expression of osteogenic genes during bone repair in rats. Photomed Laser Surg 29:311–317. https://doi.org/10.1089/pho.2010.2841
Silveira PC, Silva LA, Freitas TP et al (2011) Effects of low-power laser irradiation (LPLI) at different wavelengths and doses on oxidative stress and fibrogenesis parameters in an animal model of wound healing. Lasers Med Sci 26:125–131. https://doi.org/10.1007/s10103-010-0839-0
Kimura Y, Wilder-Smith P, Yonaga K, Matsumoto K (2000) Treatment of dentine hypersensitivity by lasers: a review. J Clin Periodontol 27(10):715–721. https://doi.org/10.1034/j.1600-051x.2000.027010715.x
Tay LY, Kose C, Loguercio AD, Reis A (2009) Assessing the effect of a desensitizing agent used before in-office tooth bleaching. J Am Dent Assoc 140:1245–1251. https://doi.org/10.14219/jada.archive.2009.0047
Thiesen CH, Filho R, Prates LH et al (2013) The influence of desensitizing dentifrices on pain induced by in-office bleaching. Braz Oral Res 27:517–523. https://doi.org/10.1590/S1806-83242013000600012
Wang Y, Gao J, Jiang T, Liang S, Zhou Y, Matis BA (2015) Evaluation of the efficacy of potassium nitrate and sodium fluoride as desensitizing agents during tooth bleaching treatment – a systematic review and meta-analysis. J Dent 43:913–923. https://doi.org/10.1016/j.jdent.2015.03.015
Nanjundassetty J, Ashrafulla M (2016) Efficacy of desensitizing agents on postoperative sensitivity following an in-office vital tooth bleaching: a randomized controlled clinical trial. J Conserv Dent 19:207–211 http://www.jcd.org.in/text.asp?2016/19/3/207/181927
Schulz KF, Altman DG, Moher D (2010) Consort 2010 statement: updated guidelines for reporting parallel group randomized trials. BMJ 340:698–702. https://doi.org/10.1136/bmj.c332
World Medical Association (2013) World medical association declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA 27:2191–2194. https://doi.org/10.1001/jama.2013.281053
Abrams AP, Thompson LA (2014) Physiology of aging of older adults: systemic and oral health considerations. Dent Clin N Am 58:729–738. https://doi.org/10.1016/j.cden.2014.06.002
Farac RV, Morgental RD, De Pontes Lima RK et al (2012) Pulp sensibility test in elderly patients. Gerodontology 29:135–139. https://doi.org/10.1111/j.1741-2358.2012.00623.x
Moosavi H, Arjmand N, Ahrari F, Zakeri M, Maleknejad F (2016) Effect of low-level laser therapy on tooth sensitivity induced by in-office bleaching. Lasers Med Sci 31:713–719. https://doi.org/10.1007/s10103-016-1913-z
Pintado-Palomino K, Tirapelli C (2015) The effect of home-use and in-office bleaching treatments combined with experimental desensitizing agents on enamel and dentin. Eur J Dent 9:66–73. https://doi.org/10.4103/1305-7456.149645
Eimar H, Siciliano R, Abdallah M et al (2012) Hydrogen peroxide whitens teeth by oxidizing the organic structure. J Dent 40:25–33. https://doi.org/10.1016/j.jdent.2012.08.008
Caviedes-Bucheli J, Ariza-Garcia G, Restrepo-Mendez S et al (2008) The effect of tooth bleaching on substance P expression in human dental pulp. J Endod 34:1462–1465. https://doi.org/10.1016/j.joen.2008.09.013
Vaz MM, Lopes LG, Cardoso PC, Souza JB, Batista AC, Costa NL, Torres ÉM, Estrela C (2016) Inflammatory response of human detal pulp to at-home and in-office tooth bleaching. J Appl Oral Sci 24:509–517. https://doi.org/10.1590/1678-775720160137
Karu TI (2003) Cellular mechanism of low power laser therapy. Lasers Med Dent 3:79–100. https://doi.org/10.1117/12.518686
Umana M, Heysselaer D, Tielemans M et al (2013) Dentinal tubules sealing by means of diode lasers (810 and 980 nm): a preliminary in vitro study. Photomed Laser Surg 31:307–314. https://doi.org/10.1089/pho.2012.3443
Pihlstrom BL, Barnett ML (2016) Design, operation, and interpretation of clinical trials. J Dent Res 89:759–772. https://doi.org/10.1177/0022034510374737
Yilmaz HG, Kurtulmus-Yilmaz S, Cengiz E, Bayindir H et al (2011) Clinical evaluation of Er, Cr: YSGG and GaAlAs a randomized controlled clinical trial of a laser therapy for treating dentine hypersensitivity: a randomized controlled clinical trial. J Dent 39:249–254
Pandis N, Walsh T, Polychronopoulou A, Katsaros C, Eliades T (2013) Split-mouth designs in orthodontics: an overview with applications to orthodontic clinical trials. Eur J Orthod 35:783–789
Kara HB, Cakan U, Yilmaz B et al (2016) Efficacy of diode laser and Gluma on post-preparation sensitivity: a randomized split-mouth clinical study. J Esthet Restor Dent 28:405–411
Femiano F, Femiano R, Lanza A et al (2013) Efficacy of diode laser in association to sodium fluoride vs Gluma desensitizer on treatment of cervical dentin hypersensitivity. A double blind controlled trial. Am J Dent 26:214–218
Dohi S, Jain S, Hegde R (2014) Effect of low-level laser therapy in reducing dentinal hypersensitivity and pain following periodontal flap surgery. Photomed Laser Surg 32:700–706
García-Delaney C, Abad-Sánchez D, Arnabat-Domínguez J et al (2017) Evaluation of the effectiveness of the photobiomodulation in the treatment of dentin hypersensitivity after basic therapy. A randomized clinical trial. J Clin Exp Dent 9:e694–e702
Dilsiz A, Canakci V, Ozdemir A, Kaya Y (2009) Clinical evaluation of Nd: YAG and 685-nm diode laser therapy for desensitization of teeth with gingival recession. Photomed Laser Surg 27:843–848
Farias RD, Closs LQ, Miguens SA Jr (2016) Evaluation of the use of low-level laser therapy in pain control in orthodontic patients: a randomized split-mouth clinical trial. Angle Orthod 86:193–198
Doshi-Mehta G, Bhad-Patil WA (2012) Efficacy of low-intensity laser therapy in reducing treatment time and orthodontic pain: a clinical investigation. Am J Orthod Dentofac Orthop 141:289–297
Haywood VB, Cordero R, Wright K et al (2005) Brushing with a potassium nitrate dentifrice to reduce bleaching sensitivity. J Clin Dent 16:17–22
Low SB, Allen EP, Kontogiorgos ED (2015) Reduction in dental hypersensitivity with Nano-hydroxyapatite, potassium nitrate, sodium monoflurophosphate and antioxidants. Open Dent J 9:92–97. https://doi.org/10.2174/1874364101509010092
Peacock JM, Orchardson R (1995) Effects of potassium ions on action potential conduction in A- and C-fibers of rat spinal nerves. J Dent Res 74:634–641. https://doi.org/10.1177/00220345950740020301
Diamanti I, Koletsi-Kounari H, Mamai-Homata E, Vougiouklakis G (2010) Effect of fluoride and of calcium sodium phosphosilicate toothpastes on pre-softened dentin demineralization and remineralization in vitro. J Dent 38:671–677. https://doi.org/10.1016/j.jdent.2010.05.010
Pinto SCS, Bandéca MC, Pinheiro MC, Cavassim R (2014) Preventive effect of a high fluoride toothpaste and arginine-carbonate toothpaste on dentinal tubules exposure followed by acid challenge: a dentine permeability evaluation. BMC Res Notes 7:385. https://doi.org/10.1186/1756-0500-7-385
Alencar CM, Silva RC, Araújo JLN et al (2017) A clinical, randomized, double-blind study on the use of toothpastes immediately after at-home tooth bleaching. Am J Dent 30:267–271
Alexandrino LD, Alencar CM, da Silveira ADS et al (2017) Randomized clinical trial of the effect of novamin and CPP-ACPF in combination with dental bleaching. J Appl Oral Sci 25:335–340. https://doi.org/10.1590/1678-7757-2016-0408
Brannstrom M, Linden LA, Johnson G (1968) Movement of dentinal and pupal fluid caused by clinical procedures. J Dent Res 47:679–682. https://doi.org/10.1177/00220345680470050201
Stead WJ, Orchardson R, Warren PB (1996) A mathematical model of potassium ion diffusion in dentinal tubules. Arch Oral Biol 41:679–687. https://doi.org/10.1016/S0003-9969(96)00073-8
Markowitz K, kim S (1985) The effects of various ionic solutions on pulpal nerve sensitivity. J Dent Res 64:309
Pirnat S (2007) Versatility of an 810 nm diode laser in dentistry: an overview. J Laser Health Acad 4:1–8
Borges A, Barcellos D, Gomes C (2012) Dentin hypersensitivity-etiology, treatment possibilities and other related factors: a literature review. World J Dent 3:60–67. https://doi.org/10.5005/jp-journals-10015-1129
Melzack R (1975) The McGill pain questionnaire: major properties and scoring methods. Pain 1:277–299. https://doi.org/10.1016/0304-3959(75)90044-5
Addy M, West N, Barlow A et al (2007) Dentine hypersensitivity: is there both stimulus and placebo responses in clinical trials? Int J Dent Hyg 5:53–59. https://doi.org/10.1111/j.1601-5037.2007.00228.x
Porto IC, Andrade AK, Montes MA (2009) Diagnosis and treatment of dentinal hypersensitivity. J Oral Sci 51:323–332. https://doi.org/10.2334/josnusd.51.323
Funding
The work was supported by the National Council for Scientific and Technological Development, Ministry of Science and Technology, Brazil.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
de Paula, B., Alencar, C., Ortiz, M. et al. Effect of photobiomodulation with low-level laser therapy combined with potassium nitrate on controlling post-bleaching tooth sensitivity: clinical, randomized, controlled, double-blind, and split-mouth study. Clin Oral Invest 23, 2723–2732 (2019). https://doi.org/10.1007/s00784-018-2715-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2715-4