Abstract
Aims
This study was designed to answer the question whether surgery due to newly diagnosed cancer may modify quality of diabetes’ management, as suggested by current guidelines.
Methods
Adherence to guideline composite indicator (GCI), a process indicator including one annual assessment of HbA1c and at least two among eye examination, serum lipids measurement and microalbuminuria, was evaluated between years 2011–2012 and 2014–2015 in 158,069 diabetic patients living in Tuscany, Italy, on 1 January 2011 and surviving on 31 December 2015, of whom 661 were hospitalized in index year 2013 for a surgery procedure due to a newly incident cancer. Difference in GCI modification (DELTA_GCI) of these patients was compared with that of diabetic people without cancer, strictly matched for main confounders by means of a propensity score.
Results
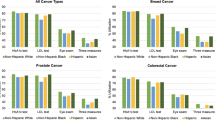
In diabetic patients with cancer, GCI adherence increased by about 8 % between years 2011–2012 and 2014–2015. When compared with controls, DELTA_GCI increased by 6 % in cancer group compared with controls (p < 0.05), but any significance was lost after matching the groups by propensity score (3 %; p = NS).
Conclusions
Our study suggests that a hospitalization for a surgical procedure due to a newly diagnosed cancer does not influence the compliance to a quality process indicator of diabetes care such as GCI.

Similar content being viewed by others
References
Inoue M, Iwasaki M, Otani T, Sasazuki S, Noda M, Tsugane S (2006) Diabetes mellitus and the risk of cancer: results from a large-scale population-based cohort study in Japan. Arch Intern Med 166:1871–1877
Jee SH, Ohrr H, Sull JW, Yun JE, Ji M, Samet JM (2005) Fasting serum glucose level and cancer risk in Korean men and women. JAMA 293:194–202
Stattin P, Björ O, Ferrari P, Lukanova A, Lenner P, Lindahl B et al (2007) Prospective study of hyperglycemia and cancer risk. Diabetes Care 30:561–567
Rousseau MC, Parent ME, Pollak MN, Siemiatycki J (2006) Diabetes mellitus and cancer risk in a population-based case-control study among men from Montreal, Canada. Int J Cancer 118:2105–2109
Giovannucci E, Harlan DM, Archer MC, Bergenstal RM, Gapstur SM, Habel LA et al (2010) Diabetes and cancer: a consensus report. CA Cancer J Clin 60:207–221
Monami M, Dicembrini I, Mannucci E (2014) Thiazolidinediones and cancer: results of a meta-analysis of randomized clinical trials. Acta Diabetol 51:91–101
García-Esquinas E, Guinó E, Castaño-Vinyals G, Pérez-Gómez B, Llorca J et al (2016) Association of diabetes and diabetes treatment with incidence of breast cancer. Acta Diabetol 53:99–107
Zanders MM, van Herk-Sukel MP, Herings RM, van de Poll-Franse LV, Haak HR (2016) Impact of cancer diagnosis and treatment on glycaemic control among individuals with colorectal cancer using glucose-lowering drugs. Acta Diabetol [Epub ahead of print] PubMed PMID: 27087004
Jacob P, Chowdhury TA (2015) Management of diabetes in patients with cancer. QJM 108:443–448
Keating NL, O’Malley AJ, Smith MR (2006) Diabetes and cardiovascular disease during androgen deprivation therapy for prostate cancer. J Clin Oncol 24:4448–4456
Derweesh IH, Diblasio CJ, Kincade MC, Malcolm JB, Lamar KD, Patterson AL et al (2007) Risk of new-onset diabetes mellitus and worsening glycaemic variables for established diabetes in men undergoing androgen-deprivation therapy for prostate cancer. BJU Int 100:1060–1065
Nguyen NP, Vos P, Vinh-Hung V, Borok TL, Dutta S, Karlsson U et al (2007) Altered glucose metabolism during chemoradiation for head and neck cancer. Anticancer Res 29:4683–4687
Feng JP, Yuan XL, Li M, Fang J, Xie T, Zhou Y et al (2013) Secondary diabetes associated with 5-fluorouracil-based chemotherapy regimens in non-diabetic patients with colorectal cancer: results from a single-centre cohort study. Colorectal Dis 15:27–33
Poulson J (1997) The management of diabetes in patients with advanced cancer. J Pain Symptom Manag 13:339–346
McCoubrie R, Jeffrey D, Paton C, Dawes L (2005) Managing diabetes mellitus in patients with advanced cancer: a case note audit and guidelines. Eur J Cancer Care (Engl) 14:244–248
Gini R, Francesconi P, Mazzaglia G, Cricelli I, Pasqua A, Gallina P et al (2013) Chronic disease prevalence from Italian administrative databases in the VALORE project: a validation through comparison of population estimates with general practice databases and national survey. BMC Public Health 13:15
Giorda C, Picariello R, Nada E et al (2012) The impact of adherence to screening guidelines and of diabetes clinics referral on morbidity and mortality in diabetes. PLoS One 7:e33839
Bezzini D, Policardo L, Meucci G et al (2016) Prevalence of multiple sclerosis in Tuscany (Central Italy): a study based on validated administrative data. Neuroepidemiology 46:37–42
Baldacci F, Policardo L, Rossi S, Ulivelli M, Ramat S, Grassi E et al (2015) Reliability of administrative data for the identification of Parkinson’s disease cohorts. Neurol Sci 36:783–786
Buja A, Damiani G, Gini R, Visca M, Federico B, Donato D et al (2014) Systematic age-related differences in chronic disease management in a population-based cohort study: a new paradigm of primary care is required. PLoS One 9:e91340
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Vissers PA, Falzon L, van de Poll-Franse LV, Pouwer F, Thong MS (2016) The impact of having both cancer and diabetes on patient-reported outcomes: a systematic review and directions for future research. J Cancer Surviv 10:406–415
Swerdlow AJ, Laing SP, Qiao Z, Slater SD, Burden AC, Botha JL et al (2005) Cancer incidence and mortality in patients with insulin-treated diabetes: a UK cohort study. Br J Cancer 92:2070–2075
Lipscombe LL, Goodwin PJ, Zinman B, McLaughlin JR, Husx JE (2008) The impact of diabetes on survival following breast cancer. Breast Cancer Res Treat 109:389–395
Stein KB, Snyder CF, Barone BB, Yeh HC, Peairs KS, Derr RL et al (2010) Colorectal cancer outcomes, recurrence, and complications in persons with and without diabetes mellitus: a systematic review and meta-analysis. Dig Dis Sci 55:1839–1851
Barone BB, Yeh HC, Snyder CF, Peairs KS, Stein KB, Derr RL et al (2008) Long-term all-cause mortality in cancer patients with pre-existing diabetes mellitus: a systematic review and metaanalysis. JAMA 300:2754–2764
Hershey DS, Given B, Given C et al (2012) Diabetes and cancer: impact on health-related quality of life. Oncol Nurs Forum 39:449–457
Mols F, Aquarius AE, Essink-Bot ML et al (2008) Does diabetes mellitus as a comorbid condition affect the health-related quality of life in prostate cancer survivors? Results of a population-based observational study. BJU Int 102:1594–1600
Onitilo AA, Donald M, Stankowski RV et al (2013) Breast and prostate cancer survivors in a diabetic cohort: results from the living with diabetes study. Clin Med Res 11:210–218
Bowker SL, Pohar SL, Johnson JA (2006) A cross-sectional study of health-related quality of life deficits in individuals with comorbid diabetes and cancer. Health Qual Life Outcomes 4:17
Vissers PA, Thong MS, Pouwer F et al (2014) The individual and combined effect of colorectal cancer and diabetes on health-related quality of life and sexual functioning: results from the PROFILES registry. Support Care Cancer 22:3071–3079
Gallo M, Gentile L, Arvat E, Bertetto O, Clemente G (2016) Diabetology and oncology meet in a network model: union is strength. Acta Diabetol 53:515–524
Relazione Sanitaria. Agenzia regionale di Sanità Toscana. https://www.ars.toscana.it/it/pubblicazioni/relazioni-sanitarie-regionali/2009-2013/3230-relazione-sanitaria-regionale-2009-2013.html. Accessed 17 July 2016
Giorda C, Petrelli A, Gnavi R, Regional Board for Diabetes Care of Piemonte (2006) The impact of second-level specialized care on hospitalization in persons with diabetes: a multilevel population-based study. Diabet Med 23:377–383
Giorda CB, Picariello R, Nada E et al (2014) Comparison of direct costs of type 2 diabetes care: different care models with different outcomes. Nutr Metab Cardiovasc Dis 24:717–724
Gnavi R, Picariello R, la Karaghiosoff L et al (2009) Determinants of quality in diabetes care process: the population-based Torino Study. Diabetes Care 32:1986–1992
Seghieri C, Policardo L, Francesconi P, Seghieri G (2016) Gender differences in the relationship between diabetes process of care indicators and cardiovascular outcomes. Eur J Public Health 26:219–224
Author contribution
L.P. researched/analysed data and wrote part of the manuscript. She is moreover the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis; A.B. researched data and reviewed the manuscript; P.F. researched data and reviewed the manuscript; G.S. reviewed/researched data and wrote the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Human and animal rights disclosure
This article does not contain any studies with human or animal subjects performed by any of the author and its design does not allow to disclose patients' identity or other sensitive data. For this reason no approval by an Ethics Committee was required.
Informed consent disclosure
Each patient was assigned a unique identifier that was the same for all administrative databases. This identifier does not allow to disclose the patient’s identity and other sensitive data, and therefore, no informed consent was required from all patients for being included in the study.
Additional information
Managed by Antonio Secchi.
Rights and permissions
About this article
Cite this article
Policardo, L., Barchielli, A., Seghieri, G. et al. Does the hospitalization after a cancer diagnosis modify adherence to process indicators of diabetes care quality?. Acta Diabetol 53, 1009–1014 (2016). https://doi.org/10.1007/s00592-016-0898-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-016-0898-1