Abstract
Study design
This is a retrospective study.
Purpose
To compare the morphometric parameters of the psoas major and lumbar multifidus muscles in lumbar spinal stenosis (LSS) patients exhibiting different functional performance.
Summary of background data
LSS refers to symptoms related to size reduction of the lumbar spinal canal; however, the degree of stenosis is poorly related to symptom severity and functional impairments. Morphometric changes in the paraspinal muscles have been correlated with chronic lower back pain in previous studies. However, correlations between the functional performance of LSS patients and the morphometric changes in paraspinal muscles have seldom been reported.
Methods
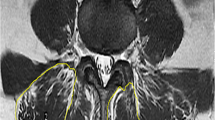
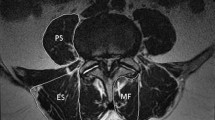
Sixty-six LSS patients without mechanical back pain or segmental instability were enrolled in the study. A review of their medical records and MRI images was performed. Morphometric parameters, including the fatty infiltration (FI) of the lumbar multifidus muscle as well as the relative cross-sectional area (RCSA) of the psoas major and lumbar multifidus muscles, were measured. Subjects were divided into high and low functional performance groups according to their Japanese Orthopedic Association (JOA) scores.
Results
The male LSS patients exhibited a larger psoas RCSA than the female patients, whereas the older patients exhibited a smaller psoas RCSA and higher multifidus FI than the younger patients. LSS patients in the high functional performance group exhibited a significantly larger psoas RCSA and lower multifidus FI.
Conclusion
The psoas RCSA and multifidus FI can be used as predictive factors for functional performance in LSS patients.

Similar content being viewed by others
References
Backstrom KM, Whitman JM, Flynn TW (2011) Lumbar spinal stenosis—diagnosis and management of the aging spine. Man Ther 16:308–317. doi:10.1016/j.math.2011.01.010
Johnsson KE, Rosen I, Uden A (1992) The natural course of lumbar spinal stenosis. Clin Orthop Relat Res 279:82–86
Brish A, Lerner MA, Braham J (1964) Intermittent claudication from compression of cauda equina by a narrowed spinal canal. J Neurosurg 21:207–211. doi:10.3171/jns.1964.21.3.0207
Porter RW, Ward D (1992) Cauda equina dysfunction. The significance of two-level pathology. Spine (Phila Pa 1976) 17:9–15
Hanai K, Kawai K, Itoh Y, Satake T, Fujiyoshi F, Abematsu N (1985) Simultaneous measurement of intraosseous and cerebrospinal fluid pressures in lumbar region. Spine (Phila Pa 1976) 10:64–68
Sullivan MS (1989) Back support mechanisms during manual lifting. Phys Ther 69:38–45
Kaariainen TLV, Taimela S, Aalto T, Kroger H, Herno A, Turunen V, Savolainen S, Kankaanpaa M, Airaksinen O (2013) Lumbar paraspinal and biceps brachii muscle function and movement perception in lumbar spinal stenosis. Eur Spine J 22:788–793
Hides JA, Stokes MJ, Saide M, Jull GA, Cooper DH (1994) Evidence of lumbar multifidus muscle wasting ipsilateral to symptoms in patients with acute/subacute low back pain. Spine (Phila Pa 1976) 19:165–172
Laasonen EM (1984) Atrophy of sacrospinal muscle groups in patients with chronic, diffusely radiating lumbar back pain. Neuroradiology 26:9–13
Demoulin C, Crielaard JM, Vanderthommen M (2007) Spinal muscle evaluation in healthy individuals and low-back-pain patients: a literature review. Jt Bone Spine 74:9–13. doi:10.1016/j.jbspin.2006.02.013
Mattila M, Hurme M, Alaranta H, Paljarvi L, Kalimo H, Falck B, Lehto M, Einola S, Jarvinen M (1986) The multifidus muscle in patients with lumbar disc herniation. A histochemical and morphometric analysis of intraoperative biopsies. Spine (Phila Pa 1976) 11:732–738
Rantanen J, Hurme M, Falck B, Alaranta H, Nykvist F, Lehto M, Einola S, Kalimo H (1993) The lumbar multifidus muscle five years after surgery for a lumbar intervertebral disc herniation. Spine (Phila Pa 1976) 18:568–574
Nachemson A (1968) The possible importance of the psoas muscle for stabilization of the lumbar spine. Acta Orthop Scand 39:47–57
Kamath S, Venkatanarasimha N, Walsh MA, Hughes PM (2008) MRI appearance of muscle denervation. Skeletal Radiol 37:397–404. doi:10.1007/s00256-007-0409-0
McLoughlin RF, D’Arcy EM, Brittain MM, Fitzgerald O, Masterson JB (1994) The significance of fat and muscle areas in the lumbar paraspinal space: a CT study. J Comput Assist Tomogr 18:275–278
Gibbons LE, Latikka P, Videman T, Manninen H, Battie MC (1997) The association of trunk muscle cross-sectional area and magnetic resonance image parameters with isokinetic and psychophysical lifting strength and static back muscle endurance in men. J Spinal Disord 10:398–403
Ward SR, Kim CW, Eng CM, Gottschalk A, Tomiya CM, Garfin SR, Lieber RL (2009) Architectural analysis and intraoperative measurements demonstrate the unique design of the multifidus muscle for lumbar spine stability. J Bone Jt Surg Am 91:176–185. doi:10.2106/jbjs.g.01311
Lee HI, Song J, Lee HS, Kang JY, Kim M, Ryu JS (2011) Association between cross-sectional areas of lumbar muscles on magnetic resonance imaging and chronicity of low back pain. Ann Rehabil Med 35:852–859. doi:10.5535/arm.2011.35.6.852
Lee JC, Cha JG, Kim Y, Kim YI, Shin BJ (2008) Quantitative analysis of back muscle degeneration in the patients with the degenerative lumbar flat back using a digital image analysis: comparison with the normal controls. Spine (Phila Pa 1976) 33:318–325. doi:10.1097/BRS.0b013e318162458f
Lee HJ, Lim WH, Park JW, Kwon BS, Ryu KH, Lee JH, Park YG (2012) The Relationship between cross sectional area and strength of back muscles in patients with chronic low back pain. Ann Rehabil Med 36:173–181. doi:10.5535/arm.2012.36.2.173
Truumees E (2005) Spinal stenosis: pathophysiology, clinical and radiologic classification. Instr Course Lect 54:287–302
Lurie JD, Tosteson AN, Tosteson TD, Carragee E, Carrino JA, Kaiser J, Sequeiros RT, Lecomte AR, Grove MR, Blood EA, Pearson LH, Weinstein JN, Herzog R (2008) Reliability of readings of magnetic resonance imaging features of lumbar spinal stenosis. Spine (Phila Pa 1976) 33:1605–1610. doi:10.1097/BRS.0b013e3181791af3
Fortin M, Battie MC (2012) Quantitative paraspinal muscle measurements: inter-software reliability and agreement using OsiriX and ImageJ. Phys Ther 92:853–864. doi:10.2522/ptj.20110380
Ropponen A, Videman T, Battie MC (2008) The reliability of paraspinal muscles composition measurements using routine spine MRI and their association with back function. Man Ther 13:349–356. doi:10.1016/j.math.2007.03.004
Pao JL, Chen WC, Chen PQ (2009) Clinical outcomes of microendoscopic decompressive laminotomy for degenerative lumbar spinal stenosis. Eur Spine J 18:672–678. doi:10.1007/s00586-009-0903-2
Toyoda H, Nakamura H, Konishi S, Dohzono S, Kato M, Matsuda H (2011) Clinical outcome of microsurgical bilateral decompression via unilateral approach for lumbar canal stenosis: minimum five-year follow-up. Spine (Phila Pa 1976) 36:410–415. doi:10.1097/BRS.0b013e3181d25829
Kjaer P, Bendix T, Sorensen JS, Korsholm L, Leboeuf-Yde C (2007) Are MRI-defined fat infiltrations in the multifidus muscles associated with low back pain? BMC Med 5:2. doi:10.1186/1741-7015-5-2
Beneck GJ, Kulig K (2012) Multifidus atrophy is localized and bilateral in active persons with chronic unilateral low back pain. Arch Phys Med Rehabil 93:300–306. doi:10.1016/j.apmr.2011.09.017
Freeman MD, Woodham MA, Woodham AW (2010) The role of the lumbar multifidus in chronic low back pain: a review. PMR 2:142–146. doi:10.1016/j.pmrj.2009.11.006 (quiz 141 p following 167)
Kim WH, Lee SH, Lee DY (2011) Changes in the cross-sectional area of multifidus and psoas in unilateral sciatica caused by lumbar disc herniation. J Korean Neurosurg Soc 50:201–204. doi:10.3340/jkns.2011.50.3.201
Hicks GE, Simonsick EM, Harris TB, Newman AB, Weiner DK, Nevitt MA, Tylavsky FA (2005) Trunk muscle composition as a predictor of reduced functional capacity in the health, aging and body composition study: the moderating role of back pain. J Gerontol A Biol Sci Med Sci 60:1420–1424
Niemelainen R, Briand MM, Battie MC (2011) Substantial asymmetry in paraspinal muscle cross-sectional area in healthy adults questions its value as a marker of low back pain and pathology. Spine (Phila Pa 196) 36:2152–2157. doi:10.1097/BRS.0b013e318204b05a
Bouche KG, Vanovermeire O, Stevens VK, Coorevits PL, Caemaert JJ, Cambier DC, Verstraete K, Vanderstraeten GG, Danneels LA (2011) Computed tomographic analysis of the quality of trunk muscles in asymptomatic and symptomatic lumbar discectomy patients. BMC Musculoskelet Disord 12:65. doi:10.1186/1471-2474-12-65
May DA, Disler DG, Jones EA, Balkissoon AA, Manaster BJ (2000) Abnormal signal intensity in skeletal muscle at MR imaging: patterns, pearls, and pitfalls. Radiographics 20:S295–S315
Bogduk N, Pearcy M, Hadfield G (1992) Anatomy and biomechanics of psoas major. Clin Biomech 7:109–119
Nachemson A (1966) Electromyographic studies on the vertebral portion of the psoas muscle; with special reference to its stabilizing function of the lumbar spine. Acta Orthop Scand 37:177–190
Henderson LKG, Richarme D, Theumann N, Schizas C (2012) Is spinal stenosis assessment dependent on slice orientation? A magnetic resonance imaging study. Eur Spine J 21:S760–S764
Acknowledgments
This work was supported by the National Taiwan University (NTU-CDP-102R7835), and National Science Council (NSC101-2320-B002-004-MY3) in Taiwan. The authors acknowledge statistical assistance provided by National Translational Medicine and Clinical Trial Resource Center (supported by National Science Council of Taiwan; NSC101-2325-B-002-078).
Conflict of interest
This manuscript does not contain information about medical device(s)/drug(s). No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Ethical approval
The study has been approved and monitored by the Research Ethics Review Committee.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, YY., Pao, JL., Liaw, CK. et al. Image changes of paraspinal muscles and clinical correlations in patients with unilateral lumbar spinal stenosis. Eur Spine J 23, 999–1006 (2014). https://doi.org/10.1007/s00586-013-3148-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-013-3148-z