Abstract
Purpose
Early integration of palliative care (PC) is recommended. The determination of predictors for patients’ request for PC may guide implementation in clinical practice. Toward this end, we analyzed the symptom burden and distress of cancer patients in outpatient care and examined their need and request for PC.
Methods
Between October 2013 and March 2016, 705 patients receiving outpatient cancer treatment took part in the survey. We used the new MInimal DOcumentation System to detect symptom clusters. Additionally, patients’ request for palliative and psychosocial support was assessed. Groups of patients with PC request were compared to patients without PC request regarding their symptom clusters. Logistic regression analysis was applied to discover significant predictors for the requested inclusion of PC.
Results
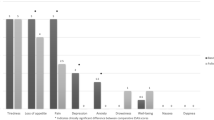
A total of 159 patients (25.5%) requested additional support by PC. Moderate and severe tiredness (40.3%), weakness (37.9%), pain (25.0%), loss of appetite (22.3%), and dyspnea (19.1%) were the most frequent symptoms. The group of patients requesting PC differed significantly in terms of pain, nausea, dyspnea, constipation, weakness, loss of appetite, tiredness, depression, and anxiety from patients without request for PC (p < .01). The perceived need for PC was identified by the significant predictors “depression,” “anxiety,” and “weakness” with an explained variance of 22%.
Conclusion
Combining a standardized screening questionnaire and the assessment of patients’ request for PC allows systematic monitoring for patients’ need for PC in a large Medical Oncology clinic. Depression, anxiety, and weakness are predictors of requesting PC service by patients receiving outpatient cancer treatment.



Similar content being viewed by others
References
Munkres A, Oberst MT, Hughes SH (1992) Appraisal of illness, symptom distress, self-care burden, and mood states in patients receiving chemotherapy for initial and recurrent cancer. Oncol Nurs Forum 19(8):1201–1209
Whitmer KM, Pruemer JM, Nahleh ZA, Jazieh AR (2006) Symptom management needs of oncology outpatients. J Palliat Med 9(3):628–630
Rugno FC, Ribeiro Paiva BS, Paiva CE (2014) Early integration of palliative care facilitates the discontinuation of anticancer treatment in women with advanced breast or gynecologic cancers. Gynecol Oncol 135:249–254
Dong ST, Butow PN, Agar M, Lovell MR, Boyle F, Stockler M, Forster BC, Tong A (2016) Clinicians' perspectives on managing symptom clusters in advanced cancer: a semi-structured interview study. J Pain Symptom Manag 51:706–717.e5. https://doi.org/10.1016/j.jpainsymman.2015.11.021
Temel JS, Greer JA, Muzikansky A, Gallagher ER, Admane S, Jackson VA, Dahlin CM, Blinderman CD, Jacobsen J, Pirl WF, Billings JA, Lynch TJ (2010) Early palliative care for patients with metastatic non-small lung cancer. N Engl J Med 363:733–742
World Health Organization (2016) Palliative care definition http://www.who.int/cancer/palliative/definition/en/
Fadul N, Elsayem A, Palmer JL, Del Fabbro E, Swint K, Li Z, Poulter V, Bruera E (2009) Supportive versus palliative care: what's in a name. Cancer 115:2013–2021
Lesnock JL, Arnold RM, Meyn LA, Buss MK, Quimper M, Krivak TC, Edwards RP, Chang JC (2013) Palliative care education in gynecologic oncology: a survey of the fellows. Gynecol Oncol 130:431–435
Bakitas M, Doyle Lyons K, Hegel MT, Ahles T (2013) Oncologists’ perspectives on concurrent palliative care in an NCI-designated Comprehensive Cancer Center. Palliat Support Care 11(5):415–423
Hui D, Meng YC, Bruera S, Geng Y, Hutchins R, Mori M, Strasser F, Bruera E (2016) Referral criteria for outpatient palliative cancer care: a systematic review. Oncologist 21(7):895–901. https://doi.org/10.1634/theoncologist.2016-0006
Riechelmann RP, Krzyzanowska MK, O'Carroll A, Zimmermann C (2007) Symptom and medication profiles among cancer patients attending a palliative care clinic. Support Care Cancer 15(12):1407–1412
Körner P, Ehrmann K, Hartmannsgruber J, Metz M, Steigerwald S, Flentje M, van Oorschot B (2017) Patient-reported symptoms during radiotherapy : clinically relevant symptom burden in patients treated with palliative and curative intent. Strahlenther Onkol 193(7):570–577. https://doi.org/10.1007/s00066-017-1146-5
Radbruch L, Sabatowski R, Loick G, Jonen-Thielemann I, Elsner F, Hormann E (2000) MIDOS-validation of a minimal documentation system for palliative medicine. Schmerz 14(4):231–239
Stiel S, Matthes ME, Bertram L, Ostgathe C, Elsner F, Radbruch L (2010) Validation of the new version of the minimal documentation system (MIDOS) for patients in palliative care: the German version of the Edmonton Symptom Assessment Scale (ESAS). Schmerz 24(6):596–604
Cohen J (1988) Statistical power analysis for the behavioral sciences. L. Erlbaum Associates, Hillsdale
Gaertner J, Wuerstlein R, Ostgathe C, Mallmann P, Harbeck N, Voltz R (2011) Facilitating early integration of palliative care into breast Cancer therapy. Promoting disease-specific guidelines. Breast Care 6:240–244
Wentlandt K, Krzyzanowska MK, Swami N, Rodin GM, Le LW, Zimmermann C (2012) Referral practices of oncologists to specialized palliative care. J Clin Oncol 30(35):4380–4386. https://doi.org/10.1200/JCO.2012.44.0248
Hui D, Bruera E (2016) Integrating palliative care into the trajectory of cancer care. Nat Rev Clin Oncol 13:159–171
Hui D, Bruera E (2017) The Edmonton Symptom Assessment System 25 years later: past, present, and future developments. J Pain Symptom Manag 53(3):630–643. https://doi.org/10.1016/j.jpainsymman.2016.10.370
Morita T, Fujimoto K, Namba M, Sasaki N, Ito T, Yamada C, Ohba A, Hiroyoshi M, Niwa H, Yamada T, Noda (2008) Palliative care needs of cancer outpatients receiving chemotherapy: an audit of a clinical screening project. Support Care Cancer 16(1):101–107
Hui D, Mori M, Watanabe SM, Caraceni A, Strasser F, Saarto T, Cherny N, Glare P, Kaasa S, Bruera E (2016) Referral criteria for outpatient specialty palliative cancer care: an international consensus. Lancet Oncol 17(12):e552–e559. https://doi.org/10.1016/S1470-2045(16)30577-0
Levy M, Smith T, Alvarez-Perez A, Back A, Baker JN, Beck AC, Block S, Dalal S, Dans M, Fitch TR, Kapo J, Kutner JS, Kvale E, Misra S, Mitchell W, Portman DG, Sauer TM, Spiegel D, Sutton L, Szmuilowicz E, Taylor RM, Temel J, Tickoo R, Urba SG, Weinstein E (2016) Palliative Care Version 1.2016. J Natl Compr Cancer Netw 14(1):82–113
Schenker Y, Park SY, Maciasz R, Arnold RM (2014) Do Patients with advanced cancer and unmet palliative care needs have an interest in receiving palliative care services? J Palliat Med 17(6):667–672. https://doi.org/10.1089/jpm.2013.0537
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008. The local ethical review committee of the University of Essen approved the data analysis (16-6800-BO). Informed consent was obtained from all patients for being included in the study. This article does not contain any studies with human or animal subjects.
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 20 kb)
Rights and permissions
About this article
Cite this article
Tewes, M., Rettler, T., Wolf, N. et al. Predictors of outpatients’ request for palliative care service at a medical oncology clinic of a German comprehensive cancer center. Support Care Cancer 26, 3641–3647 (2018). https://doi.org/10.1007/s00520-018-4245-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4245-7