Abstract
Objective
The Standardizing Care to Improve Outcomes in Pediatric End Stage Renal Disease (SCOPE) collaborative seeks to reduce hemodialysis (HD) catheter-associated blood stream infections (CA-BSI) by increasing implementation of standardized HD catheter care bundles. We report HD catheter care practices and HD CA-BSI rates from SCOPE.
Methods
Catheter care practices and infection events were collected prospectively during the study period, from collaborative implementation in June 2013 through May 2017. For comparative purposes, historical data, including patient demographics and HD CA-BSI events, were collected from the 12 months prior to implementation. Catheter care bundle compliance in 5 care bundle categories was monitored across the post-implementation reporting period at each center via monthly care observation forms. CA-BSI rates were calculated monthly, and reported as number of infections per 100 patient months. Changes in CA-BSI rates were assessed using generalized linear mixed model (GLMM) techniques.
Results
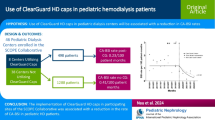
Three hundred twenty-five patients with tunneled HD catheters [median (IQR) age 12 years (6, 16), M 53%, F 47%] at 15 centers were included. A total of 3996 catheter care observations over 4170 patient months were submitted with a median (IQR) 5 (2, 14) observations per patient. Overall bundle compliance was high at 87.6%, with a significant and progressive increase (p < 0.001) in compliance for 4/5 bundle categories over the 48-month study period. The adjusted CA-BSI rate significantly decreased over time from 3.3/100 patient months prior to implementation of the care bundles to 0.8/100 patient months 48 months after care bundle implementation (p < 0.001).
Conclusions
Using quality improvement methodology, SCOPE has demonstrated a significant increase in compliance with a majority of HD catheter care practices and a significant reduction in the rate of CA-BSI among children maintained on HD.



Similar content being viewed by others
References
2018 USRDS Annual Data Report, Volume 2: ESRD in the United States: Chapter 7: ESRD among children, adolescents and young, adults, https://www.usrds.org/2018/view/v2_07.aspx.
Nguyen DB, Shugart A, Lines C, Shah AB, Edwards J, Pollock D, Sievert D, Patel PR (2017) National Healthcare Safety Network (NHSN) dialysis event surveillance report for 2014. CJASN 12(7):1139–1146
Ullman AJ, Marsh N, Mihala G, Cooke M, Rickard CM (2015) Complications of central venous access devices: a systematic review. Pediatrics 136(5):e1331–e1344
Shroff R, Calder F, Bakkalo S et al (2019) Vascular access in children requiring maintenance haemodialysis: a consensus document by the European Society for Paediatric Nephrology Dialysis Working Group. Nephrol Dial Transplant. https://doi.org/10.1093/ndt/gfz011 [Epub ahead of print]
Patel PR, Brinsley-Rainisch K (2018) The making dialysis safer for patients coalition: a new partnership to prevent hemodialysis-related infections. Clin J Am Soc Nephrol 13:175–181
Neu AM, Miller MR, Stuart J, Lawlor J, Richardson T, Martz K, Rosenberg C, Newland J, McAfee N, Begin B, Warady BA, Collaborative Participants SCOPE (2014) Design of the standardizing care to improve outcomes in pediatric end stage renal disease collaborative. Pediatr Nephrol 29(9):1477–1484
Sethna CB, Bryant K, Munshi R, Warady BA, Richardson T, Lawlor J, Newland JG, Neu A, SCOPEInvestigators (2016) Risk factors for and outcomes of catheter-associated peritonitis in children: the SCOPE collaborative. Clin J Am Soc Nephrol 11(9):1590–1596
Neu AM, Richardson T, Lawlor J, Stuart J, Newland J, McAfee N, Warady BA, Collaborative Participants SCOPE (2016) Implementation of standardized follow-up care significantly reduces peritonitis in children on chronic peritoneal dialysis. Kidney Int 89(6):1346–1354
Yi SH, Kallen AJ, Hess S, Bren VR, Lincoln ME, Downham G, Kelley K, Booth SL, Weirich H, Shugart A, Lines C, Melville A, Jernigan JA, Kleinbaum DG, Patel PR (2016) Sustained infection reduction in outpatient hemodialysis centers participating in a collaborative bloodstream infection prevention Effort. Infect Control Hosp Epidemiol 37(7):863–866
Ramage IJ, Bailie A, Tyerman KS, McColl JH, Pollard SG, Fitzpatrick MM (2005) Vascular access survival in children and young adults receiving long-term hemodialysis. Am J Kidney Dis 45(4):708–714
Sharma A, Zilleruelo G, Abitbol C, Montane B, Strauss J (1999) Survival and complications of cuffed catheters in children on chronic hemodialysis. Pediatr Nephrol 13(3):245–248
Borzych-Duzalka D, Shroff R, Ariceta G et al (2019) Vascular access, complications, and outcomes in children on maintenance hemodialysis: findings from the International Pediatric Hemodialysis Network (IPHN) Registry. Am J Kidney Dis 74(2):193–202
Stefanidis CJ (2009) Prevention of catheter-related bacteremia in children on hemodialysis: time for action. Pediatr Nephrol 24(11):2087–2095
Sucupira C, Abramczyk ML, de Abreu Carvalhaes JT, de Moraes-Pinto MI (2012) Surveillance system of hemodialysis-associated infections in a pediatric unit. Infect Control Hosp Epidemiol 33(5):521–523
Wang K, Wang P, Liang XH, Yuan FF (2015) Liu ZS (2015) Cuffed-tunneled hemodialysis catheter survival and complications in pediatric patients: a single-center data analysis in China. Int J Clin Exp Med 8(6):9765–9771
Stefanidis CJ (2010) Preventing catheter-related infections in children undergoing hemodialysis, Expert Rev. Anti Infect Ther 8(11):1239–1249
Baracco R, Mattoo T, Jain A, Kapur G, Valentini RP (2014) Reducing central venous catheters in chronic hemodialysis--a commitment to arteriovenous fistula creation in children. Pediatr Nephrol 29(10):2013–2020
Chotikanatis K, Suman N, Bäcker M, Paudyal B, Schoeneman M, Kohlhoff S, Hammerschlag MR (2015) Pediatric fistula initiative: reducing bloodstream infections in an outpatient pediatric hemodialysis center. J Pediatric Infect Dis Soc 4(4):363–366
Hayes WN, Watson AR, Callaghan N, Wright E, Stefanidis CJ, European Pediatric Dialysis Working Group (2012) Vascular access: choice and complications in European paediatric haemodialysis units. Pediatr Nephrol 27(6):999–1004
Patel PR, Yi SH, Booth S, Bren V, Downham G, Hess S, Kelley K, Lincoln M, Morrissette K, Lindberg C, Jernigan JA, Kallen AJ (2013) Bloodstream infection rates in outpatient hemodialysis facilities participating in a collaborative prevention effort: a quality improvement report. Am J Kidney Dis 62(2):322–330
Eisenstein I, Tarabeih M, Magen D, Pollack S, Kassis I, Ofer A, Engel A, Zelikovic I (2011) Low infection rates and prolonged survival times of hemodialysis catheters in infants and children. Clin J Am Soc Nephrol 6(4):793–798
Paglialonga F, Consolo S, Biasuzzi A, Assomou J, Gattarello E, Patricelli MG, Giannini A, Chidini G, Napolitano L, Edefonti A (2014) Reduction in catheter-related infections after switching from povidone-iodine to chlorhexidine for the exit-site care of tunneled central venous catheters in children on HD. Hemodial Int 18(Suppl 1):S13–S18
Hemmelgarn BR, Moist LM, Lok CE et al (2011) Prevention of dialysis catheter malfunction with recombinant tissue plasminogen activator. N Engl J Med 364:303–312
Beathard GA, Urbanes A (2008) Infection associated with tunneled hemodialysis catheters. Semin Dial 21(6):528–538
Brunelli SM, Van Wyck DB, Njord L, Ziebol RJ, Lynch LE, Killion DP (2018) Cluster-randomized trial of devices to prevent catheter-related bloodstream infection. J Am Soc Nephrol 29(4):1336–1343
NTDS: Promoting Infection Prevention in Dialysis Facilities 2017 ANNUAL REPORT, available at: https://www.asn-online.org/ntds
Onder AM, Chandar J, Coakley S, Abitbol C, Montane B, Zilleruelo G (2006) Predictors and outcome of catheter-related bacteremia in children on chronic hemodialysis. Pediatr Nephrol 21(10):1452–1458
Silver SA, Bell CM, Chertow GM, Shah PS, Shojania K, Wald R, Harel Z (2017) Effectiveness of quality improvement strategies for the management of CKD: a meta-analysis. Clin J Am Soc Nephrol 12(10):1601–1614
Acknowledgment
SCOPE partners with the CDC’s Making Dialysis Safer for Patients Coalition.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Marsenic, O., Rodean, J., Richardson, T. et al. Tunneled hemodialysis catheter care practices and blood stream infection rate in children: results from the SCOPE collaborative. Pediatr Nephrol 35, 135–143 (2020). https://doi.org/10.1007/s00467-019-04384-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-019-04384-7