Abstract
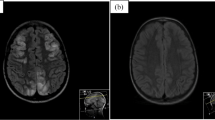
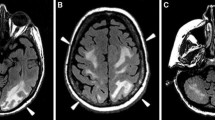
Posterior reversible encephalopathy syndrome (PRES) is characterized clinically by headaches, seizures, vomiting, nausea, visual abnormalities, and altered mental function and is often (but not invariably) accompanied by parieto-occipital imaging features. The aim of this study is to describe the clinical and radiological features and outcome following PRES in a paediatric cohort. From a retrospectively identified cohort, case records were studied to confirm a diagnosis of PRES. Neuroimaging was reviewed again to assign to recently described radiological subtypes parieto-occipital pattern, holohemispheric watershed pattern, dominant superior frontal sulcus pattern, and asymmetrical or partial expression of the three primary patterns (A/P). Patient outcome was measured by the modified Rankin scale (mRS) scores. Nine boys and three girls with mean age of 12 were identified. Hypertensive episodes (n = 11), tacrolimus toxicity (n = 4), and autoimmunity (n = 1) were identified as potential risk factors/etiologies. Their median mRS at the peak of illness was 2 (range 2–5); three children required intensive care support. After mean follow-up of 35 months (median 37 months; range 3–60 months), all patients improved significantly with mean mRS of 1 (median 1; range 0–1). Conclusion: PRES is easily recognizable by the clinical and radiological features. Although severe at presentation, the outcome from this condition is favorable.



Similar content being viewed by others
Abbreviations
- AI:
-
Autoimmune
- A/P:
-
Atypical or partial expression
- CNI:
-
Calcineurin Inhibitors
- CKD:
-
Chronic kidney disease
- DWI:
-
Diffusion-weighted imaging
- EEG:
-
Electroencephalogram
- ESRF:
-
End stage renal failure
- FLAIR:
-
Fluid-attenuated inversion recovery
- HSP:
-
Henoch-Scholein purpura
- HbSS:
-
Sickle cell anemia
- HH:
-
Holohemispheric
- HT:
-
Hypertension
- MRI:
-
Magnetic resonance imaging
- mRS:
-
Modified Rankin scale
- Non T:
-
Non-transplant
- PO:
-
Parieto-occipital
- PRES:
-
Posterior reversible encephalopathy syndrome
- SFS:
-
Superior frontal sulcus
- SLE:
-
Systemic lupus erythematosus
- TT:
-
Tacrolimus toxicity
References
Aboian MS, Junna MR, Krecke KN, Wirrell EC (2009) Mesial temporal sclerosis after posterior reversible encephalopathy syndrome. Pediatr Neurol 41(3):226–228
Auntunes NL, Small TN, George D (1999) Posterior leukoencephalopathy syndrome may not be reversible. Pediatric Neurol 20(3):241–243
Bartynski W (2008) Posterior reversible encephalopathy syndrome, part 1: fundamental imaging and clinical feature. Am J Neuroradiol 29:1036–1042
Bartynski WS, Boardman JF et al (2006) Posterior reversible encephalopathy syndrome in infection, sepsis, and shock. Ajnr: Am J Neuroradiol 27(10):2179–2190
Bartynski WS, Tan HP et al (2008) Posterior reversible encephalopathy syndrome after solid organ transplantation. AJNR Am J Neuroradiol 29(5):924–930
Bigi S, Fischer U et al (2011) Acute ischemic stroke in children versus young adults. Ann Neurol 70(2):245–254
Covarrubias DJ, Luetmer PH et al (2002) Posterior reversible encephalopathy syndrome: prognostic utility of quantitative diffusion-weighted MR images. Am J Neuroradiol 23(6):1038–1048
Dinsdale HB, Robertson DM, Chiang TY, Mukherjee SK (1971) Hypertensive cerebral microinfarction and cerebrovascular reactivity. Eur Neurol 6:29–33
Fugate JE, Claassen DO et al (2010) Posterior reversible encephalopathy syndrome: associated clinical and radiologic findings. Mayo Clin Proc 85(5):427–432
Group, N. H. B. P. E. P. W. (2005) National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents. The Fourth Report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 114:555–576
Hinchey J, Chaves C, Appignani B, Breen J, Pao L, Wang A, Pessin M, Lamy C, Mas J, Caplan L (1996) A reversible leukoencephalopathy syndrome. N Engl J Med 334:494–500
Onder AM, Lopez R et al (2007) Posterior reversible encephalopathy syndrome in the pediatric renal population. Pediatr Nephrol 22(11):1921–1929
Port JD, Beauchamp N (1998) Reversible intracerebral pathologic entities mediated by vascular autoregulatory dysfunction. Radiographics 18(2):353–367
Pula JH, Eggenberger E (2008) Posterior reversible encephalopathy syndrome. Curr Opin Ophthalmol 19(6):479–484
Rodgers GM, Taylor RN, Roberts JM (1988) Pre-eclampsia is associated with a serum factor cytotoxic to human endothelial cells. Am J Obstet Gynecol 159:908–914
Schwartz RB, Bravo SM, Kulfas RA, Hsu L, Branes PD (1995) Calcineurin neurotoxicity and its relationship to hypertensive encephalopathy: CT and MRI finding in 16 cases. AjNR Am J Roentgenol 165:627–631
Zeppa P, Fonio P et al (2012) Posterior reversible encephalopathy syndrome: description of a case in the setting of severe infection. Recenti Prog Med 103(11):526–530
Acknowledgments
The authors MDS and ML acknowledges financial support from the Department of Health via the National Institute for Health Research (NIHR) comprehensive Biomedical Research Centre award to Guy’s and St Thomas’ NHS Foundation Trust in partnership with King’s College London and King’s College Hospital NHS Foundation Trust.
Disclosure
ML receives research grants from Action Medical Research and MS Society, receives research support grants from the London Clinical Research Network and Evelina Appeal, has received consultation fees from CSL Behring, received travel grants from Merck Serono, and awarded educational grants to organize meetings by Novartis, Biogen Idec, Merck Serono, and Bayer.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Communicated by Peter de Winter
PRES in children
NO MS helped collecting data and preparing initial draft. NO, SW, and MS reviewed the data and helped in preparing the initial draft, and MS helped in subsequent reviews. AS and JU reviewed all the images independently. AS, JU, RS, and ML reviewed all the images to reach to a consensus. ML, MS, and RS assigned mRS scoring and in preparing the final draft and submission.
What is known about this condition and what is new?
PRES is a reversible condition, and there has been no report of quantitative measurement of outcome in this group of children at the time of illness and on complete recovery. We report that irrespective of the lesion load and distribution of lesion, the outcome on modified Rankin scale (mRS) is good.
Rights and permissions
About this article
Cite this article
Singh, R.R., Ozyilmaz, N., Waller, S. et al. A study on clinical and radiological features and outcome in patients with posterior reversible encephalopathy syndrome (PRES). Eur J Pediatr 173, 1225–1231 (2014). https://doi.org/10.1007/s00431-014-2301-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-014-2301-y