Abstract
Background and Purpose
This study aimed at developing a radiomics signature (R score) as prognostic biomarkers based on penumbra quantification and to validate the radiomics nomogram to predict the clinical outcomes for thrombolysis for acute ischemic stroke (AIS) patients.
Methods
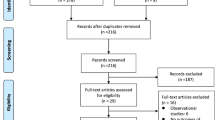
In total, 168 patients collected from seven centers were retrospectively included. A score of mismatch was defined as MIS. Based on a short-term clinical label, 456 radiomics features were evaluated with feature selection methods. R score was constructed with the selected features. To compare the predictive capabilities of the clinical factors, MIS, and R score, three nomograms were developed and evaluated, according to the short-term clinical assessment on day 7. Finally, the radiomics nomogram was validated by predicting the 3-month clinical outcomes of AIS patients, in an external cohort.
Results
R scores were found to be significantly higher in patients with favorable clinical outcomes in both training and validation datasets. The predictive value of the radiomics nomogram estimating favorable clinical outcomes was modest, with a concordance index (C-index) of 0.695 [95% confidence interval (CI) 0.667–0.723) in an external validation dataset. In addition, the area under curve (AUC) of the radiomics nomogram predicting favorable clinical outcome reached 0.886 (95% CI 0.809–0.963) on day 7 and 0.777 (95% CI 0.666–0.888) at 3 months.
Conclusions
The radiomics signature is an independent biomarker for estimating the clinical outcomes in AIS patients. By improving the individualized prediction of the clinical outcome for AIS patients 3 months after onset, the radiomics nomogram adds more value to the current clinical decision-making process.




Similar content being viewed by others
References
Wang H et al (2016) Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 388(10053):1459–1544. https://doi.org/10.1016/S0140-6736(16)31012-1
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL, American Heart Association Stroke C (2018) 2018 Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 49(3):e46–e110. https://doi.org/10.1161/STR.0000000000000158
Davis S, Donnan GA (2014) Time is Penumbra: imaging, selection and outcome. The Johann jacob wepfer award 2014. Cerebrovasc Dis 38(1):59–72. https://doi.org/10.1159/000365503
Ma H, Campbell BCV, Parsons MW, Churilov L, Levi CR, Hsu C, Kleinig TJ, Wijeratne T, Curtze S, Dewey HM, Miteff F, Tsai CH, Lee JT, Phan TG, Mahant N, Sun MC, Krause M, Sturm J, Grimley R, Chen CH, Hu CJ, Wong AA, Field D, Sun Y, Barber PA, Sabet A, Jannes J, Jeng JS, Clissold B, Markus R, Lin CH, Lien LM, Bladin CF, Christensen S, Yassi N, Sharma G, Bivard A, Desmond PM, Yan B, Mitchell PJ, Thijs V, Carey L, Meretoja A, Davis SM, Donnan GA, Investigators E (2019) Thrombolysis guided by perfusion imaging up to 9 hours after onset of stroke. New Engl J Med 380(19):1795–1803. https://doi.org/10.1056/NEJMoa1813046
Thomalla G, Simonsen CZ, Boutitie F, Andersen G, Berthezene Y, Cheng B, Cheripelli B, Cho T-H, Fazekas F, Fiehler J (2018) MRI-guided thrombolysis for stroke with unknown time of onset. New Engl J Med 379(7):611–622
Astrup J, Siesjo BK, Symon L (1981) Thresholds in cerebral ischemia - the ischemic penumbra. Stroke 12(6):723–725
Hacke W, Kaste M, Bluhmki E, Brozman M, Davalos A, Guidetti D, Larrue V, Lees KR, Medeghri Z, Machnig T, Schneider D, von Kummer R, Wahlgren N, Toni D, Investigators E (2008) Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. New Engl J Med 359(13):1317–1329. https://doi.org/10.1056/NEJMoa0804656
Zhang B, Sun XJ, Ju CH (2011) Thrombolysis with alteplase 4.5 to 6 hours after acute ischemic stroke. Eur Neurol 65(3):170–174. https://doi.org/10.1159/000324291
Davis SM, Donnan GA, Parsons MW, Levi C, Butcher KS, Peeters A, Barber PA, Bladin C, De Silva DA, Byrnes G, Chalk JB, Fink JN, Kimber TE, Schultz D, Hand PJ, Frayne J, Hankey G, Muir K, Gerraty R, Tress BM, Desmond PM, Investigators E (2008) Effects of alteplase beyond 3 h after stroke in the Echoplanar Imaging Thrombolytic Evaluation Trial (EPITHET): a placebo-controlled randomised trial. Lancet Neurol 7(4):299–309. https://doi.org/10.1016/S1474-4422(08)70044-9
Lansberg MG, Straka M, Kemp S, Mlynash M, Wechsler LR, Jovin TG, Wilder MJ, Lutsep HL, Czartoski TJ, Bernstein RA, Chang CW, Warach S, Fazekas F, Inoue M, Tipirneni A, Hamilton SA, Zaharchuk G, Marks MP, Bammer R, Albers GW, Investigators Ds (2012) MRI profile and response to endovascular reperfusion after stroke (DEFUSE 2): a prospective cohort study. Lancet Neurol 11(10):860–867. https://doi.org/10.1016/S1474-4422(12)70203-X
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL (2019) Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 50:211. https://doi.org/10.1161/str.0000000000000211
Feng R, Badgeley M, Mocco J, Oermann EK (2018) Deep learning guided stroke management: a review of clinical applications. J Neurointerv Surg 10(4):358–362. https://doi.org/10.1136/neurintsurg-2017-013355
Campbell BCV, Majoie C, Albers GW, Menon BK, Yassi N, Sharma G, van Zwam WH, van Oostenbrugge RJ, Demchuk AM, Guillemin F, White P, Davalos A, van der Lugt A, Butcher KS, Cherifi A, Marquering HA, Cloud G, Macho Fernandez JM, Madigan J, Oppenheim C, Donnan GA, Roos Y, Shankar J, Lingsma H, Bonafe A, Raoult H, Hernandez-Perez M, Bharatha A, Jahan R, Jansen O, Richard S, Levy EI, Berkhemer OA, Soudant M, Aja L, Davis SM, Krings T, Tisserand M, San Roman L, Tomasello A, Beumer D, Brown S, Liebeskind DS, Bracard S, Muir KW, Dippel DWJ, Goyal M, Saver JL, Jovin TG, Hill MD, Mitchell PJ, Collaborators H (2019) Penumbral imaging and functional outcome in patients with anterior circulation ischaemic stroke treated with endovascular thrombectomy versus medical therapy: a meta-analysis of individual patient-level data. Lancet Neurol 18(1):46–55. https://doi.org/10.1016/S1474-4422(18)30314-4
Tang TY, Jiao Y, Cui Y, Zeng CH, Zhao DL, Zhang Y, Peng CY, Yin XD, Gao PY, Yang YJ, Ju SH, Teng GJ (2018) Development and validation of a penumbra-based predictive model for thrombolysis outcome in acute ischemic stroke patients. EBioMedicine 35:251–259. https://doi.org/10.1016/j.ebiom.2018.07.028
Park H, Lim Y, Ko ES, Cho HH, Lee JE, Han BK, Ko EY, Choi JS, Park KW (2018) Radiomics signature on magnetic resonance imaging: association with disease-free survival in patients with invasive breast cancer. Clin Cancer Res 24(19):4705–4714. https://doi.org/10.1158/1078-0432.CCR-17-3783
Limkin EJ, Sun R, Dercle L, Zacharaki EI, Robert C, Reuze S, Schernberg A, Paragios N, Deutsch E, Ferte C (2017) Promises and challenges for the implementation of computational medical imaging (radiomics) in oncology. Ann Oncol 28(6):1191–1206. https://doi.org/10.1093/annonc/mdx034
Hosny A, Parmar C, Coroller TP, Grossmann P, Zeleznik R, Kumar A, Bussink J, Gillies RJ, Mak RH, Aerts H (2018) Deep learning for lung cancer prognostication: a retrospective multi-cohort radiomics study. PLoS Med 15(11):e1002711. https://doi.org/10.1371/journal.pmed.1002711
Wang Y, Liao X, Zhao X, Wang C, Liu L, Zhou Y, Wang C, Xue J, Gao P, Dong K, Ji X, Wang Y (2009) Imaging-based thrombolysis trial in acute ischemic stroke-II (ITAIS-II). Int J Stroke 4(1):49–53. https://doi.org/10.1111/j.1747-4949.2009.00245.x
Woolrich MW, Jbabdi S, Patenaude B, Chappell M, Makni S, Behrens T, Beckmann C, Jenkinson M, Smith SM (2009) Bayesian analysis of neuroimaging data in FSL. NeuroImage 45(1 Suppl):S173–186. https://doi.org/10.1016/j.neuroimage.2008.10.055
Smith SM, Jenkinson M, Woolrich MW, Beckmann CF, Behrens TE, Johansen-Berg H, Bannister PR, De Luca M, Drobnjak I, Flitney DE, Niazy RK, Saunders J, Vickers J, Zhang Y, De Stefano N, Brady JM, Matthews PM (2004) Advances in functional and structural MR image analysis and implementation as FSL. NeuroImage 23(Suppl 1):S208–219. https://doi.org/10.1016/j.neuroimage.2004.07.051
Wu O, Ostergaard L, Weisskoff RM, Benner T, Rosen BR, Sorensen AG (2003) Tracer arrival timing-insensitive technique for estimating flow in MR perfusion-weighted imaging using singular value decomposition with a block-circulant deconvolution matrix. Magn Reson Med 50(1):164–174
Zhang S, Tang H, Yu YN, Yan SQ, Parsons MW, Lou M (2015) Optimal magnetic resonance perfusion thresholds identifying ischemic penumbra and infarct core: a Chinese population-based study. CNS Neurosci Ther 21(3):289–295. https://doi.org/10.1111/cns.12367
Lansberg MG, Lee J, Christensen S, Straka M, De Silva DA, Mlynash M, Campbell BC, Bammer R, Olivot JM, Desmond P, Davis SM, Donnan GA, Albers GW (2011) RAPID automated patient selection for reperfusion therapy: a pooled analysis of the Echoplanar Imaging Thrombolytic Evaluation Trial (EPITHET) and the Diffusion and Perfusion Imaging Evaluation for Understanding Stroke Evolution (DEFUSE) Study. Stroke 42(6):1608–1614. https://doi.org/10.1161/STROKEAHA.110.609008
van Griethuysen JJM, Fedorov A, Parmar C, Hosny A, Aucoin N, Narayan V, Beets-Tan RGH, Fillion-Robin JC, Pieper S, Aerts H (2017) Computational radiomics system to decode the radiographic phenotype. Cancer Res 77(21):e104–e107. https://doi.org/10.1158/0008-5472.CAN-17-0339
Xu X, Zhang H-L, Liu Q-P, Sun S-W, Zhang J, Zhu F-P, Yang G, Yan X, Zhang Y-D, Liu X-S, Joh J (2019) Radiomic analysis of contrast-enhanced CT predicts microvascular invasion and outcome in hepatocellular carcinoma. J Hepatol 70(6):1133–1144. https://doi.org/10.1016/j.jhep.2019.02.023
Newson R (2006) Confidence intervals for rank statistics: Somers’ D and extensions. Stata J 6(3):309–334
De Long ER, De Long DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44(3):837–845
Ovbiagele B, Saver JL (2010) Day-90 acute ischemic stroke outcomes can be derived from early functional activity level. Cerebrovasc Dis 29(1):50–56. https://doi.org/10.1159/000255974
Gumbinger C, Reuter B, Stock C, Sauer T, Wietholter H, Bruder I, Rode S, Kern R, Ringleb P, Hennerici MG, Hacke W, Schlaganfall AG (2014) Time to treatment with recombinant tissue plasminogen activator and outcome of stroke in clinical practice: retrospective analysis of hospital quality assurance data with comparison with results from randomised clinical trials. BMJ 348:g3429. https://doi.org/10.1136/bmj.g3429
Huang Y, Liu Z, He L, Chen X, Pan D, Ma Z, Liang C, Tian J, Liang C (2016) Radiomics signature: a potential biomarker for the prediction of disease-free survival in early-stage (I or II) non-small cell lung cancer. Radiology 281(3):947–957. https://doi.org/10.1148/radiol.2016152234
Qiu W, Kuang H, Nair J, Assis Z, Najm M, McDougall C, McDougall B, Chung K, Wilson AT, Goyal M, Hill MD, Demchuk AM, Menon BK (2019) Radiomics-based intracranial thrombus features on CT and CTA predict recanalization with intravenous alteplase in patients with acute ischemic stroke. AJNR Am J Neuroradiol 40(1):39–44. https://doi.org/10.3174/ajnr.A5918
Lees KR, Bluhmki E, von Kummer R, Brott TG, Toni D, Grotta JC, Albers GW, Kaste M, Marler JR, Hamilton SA, Tilley BC, Davis SM, Donnan GA, Hacke W, Ecass AN, Allen K, Mau J, Meier D, del Zoppo G, De Silva DA, Butcher KS, Parsons MW, Barber PA, Levi C, Bladin C, Byrnes G, Group Er-PS (2010) Time to treatment with intravenous alteplase and outcome in stroke: an updated pooled analysis of ECASS, ATLANTIS, NINDS, and EPITHET trials. Lancet 375(9727):1695–1703. https://doi.org/10.1016/S0140-6736(10)60491-6
Acknowledgements
The authors would like to acknowledge Pei-Yi Gao from the Beijing Tiantan Hospital for providing the validation dataset collected from the following institutes: the Beijing Tiantan Hospital, the First Affiliated Hospital of Wenzhou Medical University, the Guangdong Hospital of Traditional Chinese Medicine, the Shanghai Pudong New Area People's Hospital and the Tianjin Huanhu Hospital.
Funding
This work was funded by the National Natural Science Foundation for Distinguished Young Scholars of China (81525014), the National Key Research and Development Program of China (2017YFA0104302), the National Natural Science Foundation Innovation Research Group Project (61821002), the Key Research and Development Program of Jiangsu Province (BE2016782), the Natural Science Foundation of Jiangsu Province of China (BK20170704).
Author information
Authors and Affiliations
Contributions
SHJ was study chair and principal investigator; TYT drafted the initial manuscript, which was reviewed by all the other authors. TYT, SHJ, and GJT designed and carried out the study. TYT, YJ, XPM and WZ analyzed the MR data. YC, SHJ, and GJT provided extensive critical insights and revisions of all drafts of the manuscript. DLZ, ZY, YJY and XDY enrolled patients. YC and DLZ reviewed the image processing results. All authors contributed to the final version of the manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval
The research was conducted according to the principles of the Declaration of Helsinki and the study was approved by the Ethics Committees of all listed hospitals and informed consent was obtained.
Electronic supplementary material
Below is the link to the electronic supplementary material.
415_2020_9713_MOESM1_ESM.tif
Figure S1: Development and performance of the nomograms.Note: (A) clinical nomogram; (B) MIS nomogram. The nomograms were developed using the training dataset based on the clinical and radiological features. By adding all the corresponding points, the predicted possibility of FCO for an AIS patient was located on the total point axis. SBP=systolic blood pressure; NIHSS = National Institutes of Health Stroke Scale; MIS represents the mismatch ratio between the volume of penumbra and all impaired brain regions after onset. (TIF 1089 kb)
Rights and permissions
About this article
Cite this article
Tang, Ty., Jiao, Y., Cui, Y. et al. Penumbra-based radiomics signature as prognostic biomarkers for thrombolysis of acute ischemic stroke patients: a multicenter cohort study. J Neurol 267, 1454–1463 (2020). https://doi.org/10.1007/s00415-020-09713-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-09713-7