Abstract
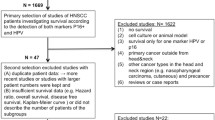
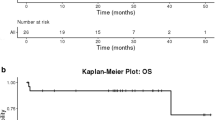
Data indicate a better prognosis for human papillomavirus (HPV)-associated head and neck squamous cell carcinoma (HNSCC). HPV and p16 detection are established markers for HPV-related HNSCC. Both are accepted as survival-independent predictors. Previous studies investigating the survival in HNSCC patients depending on HPV+/− and p16+/− status consistently found discordant results with p16−/HPV+ and p16+/HPV−. However, no meta-analysis regarding the survival according to combined HPV/p16 status has been performed yet. The objective of this study was to discriminate the impact of combined HPV+/− and p16+/− status on survival. Data sources were identification and review of publications assessing survival of the distinct subgroups with both p16 and HPV investigated in HNSCC until February, 2015. A meta-analysis was performed to classify survival and clinical outcomes. 18 out of 397 articles (4424 patients) were eligible for the meta-analysis. The percent proportion of the subgroups was 25 % for HPV+/p16+, 61.2 % for HPV−/p16−, 7.1 % for HPV−/p16+ and 6.8 % for HPV+/P16−. The meta-analysis showed a significantly improved 5-year overall survival (OS), 5-year disease-free survival and their corresponding hazard ratio for HPV+/p16+ HNSCC in comparison to HPV−/p16−, HPV+/p16− and HPV−/p16+. The 5-year OS of the HPV−/p16+ subgroup was intermediate while HPV+/p16− and HPV−/p16− HNSCC had the shortest survival. With current therapeutic strategies, survival of patients with HNSCC is better if associated with HPV+/p16+ or HPV−/p16+. Clinical trials are needed to confirm the distinct survival pattern and to investigate possible differences in survival for HPV+/p16− and HPV−/p16+ HNSCC. To further differentiate p16+ HNSCC, HPV testing may be advisable.



Similar content being viewed by others
References
Albers AE, Chen C, Koberle B et al (2012) Stem cells in squamous head and neck cancer. Crit Rev Oncol Hematol 81:224–240
Ang KK, Harris J, Wheeler R et al (2010) Human papillomavirus and survival of patients with oropharyngeal cancer. N Engl J Med 363:24–35
Begum S, Cao D, Gillison M et al (2005) Tissue distribution of human papillomavirus 16 DNA integration in patients with tonsillar carcinoma. Clin Cancer Res 11:5694–5699
Bossi P, Orlandi E, Miceli R et al (2014) Treatment-related outcome of oropharyngeal cancer patients differentiated by HPV dictated risk profile: a tertiary cancer centre series analysis. Ann Oncol 25:694–699
Bottley G, Watherston OG, Hiew YL et al (2008) High-risk human papillomavirus E7 expression reduces cell-surface MHC class I molecules and increases susceptibility to natural killer cells. Oncogene 27:1794–1799
Braakhuis BJ, Brakenhoff RH, Meijer CJ et al (2009) Human papilloma virus in head and neck cancer: the need for a standardised assay to assess the full clinical importance. Eur J Cancer 45:2935–2939
Braakhuis BJ, Rietbergen MM, Buijze M et al (2014) TP53 mutation and human papilloma virus status of oral squamous cell carcinomas in young adult patients. Oral Dis 20:602–608
Cerezo L, Lopez C, De La Torre A et al (2014) Incidence of human papillomavirus-related oropharyngeal cancer and outcomes after chemoradiation in a population of heavy smokers. Head Neck 36:782–786
Chai RC, Lambie D, Verma M et al (2015) Current trends in the etiology and diagnosis of HPV-related head and neck cancers. Cancer Med
Chaturvedi AK, Engels EA, Pfeiffer RM et al (2011) Human papillomavirus and rising oropharyngeal cancer incidence in the United States. J Clin Oncol 29:4294–4301
Chung CH, Zhang Q, Kong CS, Harris J, Fertig EJ, Harari PM, Wang D, Redmond KP, Shenouda G, Trotti A, Raben D, Gillison ML, Jordan RC, Le QT (2014) p16 protein expression and human papillomavirus status as prognostic biomarkers of nonoropharyngeal head and neck squamous cell carcinoma. J Clin Oncol 32(35):3930–3938. doi:10.1200/JCO.2013.54.5228
Dayyani F, Etzel CJ, Liu M et al (2010) Meta-analysis of the impact of human papillomavirus (HPV) on cancer risk and overall survival in head and neck squamous cell carcinomas (HNSCC). Head Neck Oncol 2:15
Deng Z, Hasegawa M, Aoki K et al (2014) A comprehensive evaluation of human papillomavirus positive status and p16INK4a overexpression as a prognostic biomarker in head and neck squamous cell carcinoma. Int J Oncol 45:67–76
Dreyer JH, Hauck F, Oliveira-Silva M et al (2013) Detection of HPV infection in head and neck squamous cell carcinoma: a practical proposal. Virchows Arch 462:381–389
Evans M, Newcombe R, Fiander A, Powell J, Rolles M, Thavaraj S, Robinson M, Powell N (2013) Human Papillomavirus-associated oropharyngeal cancer: an observational study of diagnosis, prevalence and prognosis in a UK population. BMC Cancer 13:220. doi:10.1186/1471-2407-13-220
Fakhry C, Westra WH, Li S et al (2008) Improved survival of patients with human papillomavirus-positive head and neck squamous cell carcinoma in a prospective clinical trial. J Natl Cancer Inst 100:261–269
Flavill E, Fang YV, Miles B et al (2014) Induction chemotherapy followed by concurrent chemoradiotherapy for advanced stage oropharyngeal squamous cell carcinoma with HPV and P16 testing. Ann Otol Rhinol Laryngol 123:365–373
Garland SM, Hernandez-Avila M, Wheeler CM et al (2007) Quadrivalent vaccine against human papillomavirus to prevent anogenital diseases. N Engl J Med 356:1928–1943
Geiger JL, Lazim AF, Walsh FJ et al (2014) Adjuvant chemoradiation therapy with high-dose versus weekly cisplatin for resected, locally-advanced HPV/p16-positive and negative head and neck squamous cell carcinoma. Oral Oncol 50:311–318
Granata R, Miceli R, Orlandi E et al (2012) Tumor stage, human papillomavirus and smoking status affect the survival of patients with oropharyngeal cancer: an Italian validation study. Ann Oncol 23:1832–1837
Greenlee RT, Hill-Harmon MB, Murray T et al (2001) Cancer statistics, 2001. CA Cancer J Clin 51:15–36
Guirat-Dhouib N, Baccar Y, Mustapha IB et al (2012) Oral HPV infection and MHC class II deficiency (A study of two cases with atypical outcome). Clin Mol Allergy CMA 10:6
Hammarstedt L, Lindquist D, Dahlstrand H et al (2006) Human papillomavirus as a risk factor for the increase in incidence of tonsillar cancer. Int J Cancer 119:2620–2623
Haraf DJ, Nodzenski E, Brachman D et al (1996) Human papilloma virus and p53 in head and neck cancer: clinical correlates and survival. Clin Cancer Res 2:755–762
Heath S, Willis V, Allan K, Purdie K, Harwood C, Shields P, Simcock R, Williams T, Gilbert DC (2012) Clinically significant human papilloma virus in squamous cell carcinoma of the head and neck in UK practice. Clin Oncol 24(1):e18–e23. doi:10.1016/j.clon.2011.05.007
Heiduschka G, Grah A, Oberndorfer F, Kadletz L, Altorjai G, Kornek G, Wrba F, Thurnher D, Selzer E (2014) Improved survival in HPV/p16-positive oropharyngeal cancer patients treated with postoperative radiotherapy. Strahlenther Onkol. doi:10.1007/s00066-014-0753-7
Hoffmann M, Ihloff AS, Gorogh T et al (2010) p16(INK4a) overexpression predicts translational active human papillomavirus infection in tonsillar cancer. Int J Cancer 127:1595–1602
Hoffmann M, Tribius S, Quabius ES et al (2012) HPV DNA, E6*I-mRNA expression and p16INK4A immunohistochemistry in head and neck cancer—how valid is p16INK4A as surrogate marker? Cancer Lett 323:88–96
Holzinger D, Schmitt M, Dyckhoff G, Benner A, Pawlita M, Bosch FX (2012) Viral RNA patterns and high viral load reliably define oropharynx carcinomas with active HPV16 involvement. Cancer Res 72(19):4993–5003. doi:10.1158/0008-5472.CAN-11-3934
Huang H, Zhang B, Chen W, Zou SM, Xu ZG (2013) Relationship between HPV-DNA status and p16 protein expression in oropharyngeal squamous cell carcinoma and their clinical significance. Zhonghua Zhong Liu Za Zhi 35(9):684–688
Jones AS, Goodyear PW, Ghosh S et al (2011) Extensive neck node metastases (N3) in head and neck squamous carcinoma: is radical treatment warranted? Otolaryngol Head Neck Surg 144:29–35
Jung AC, Briolat J, Millon R et al (2010) Biological and clinical relevance of transcriptionally active human papillomavirus (HPV) infection in oropharynx squamous cell carcinoma. Int J Cancer 126:1882–1894
Klussmann JP, Gultekin E, Weissenborn SJ et al (2003) Expression of p16 protein identifies a distinct entity of tonsillar carcinomas associated with human papillomavirus. Am J Pathol 162:747–753
Kong CS, Narasimhan B, Cao H, Kwok S, Erickson JP, Koong A, Pourmand N, Le QT (2009) The relationship between human papillomavirus status and other molecular prognostic markers in head and neck squamous cell carcinomas. Int J Radiat Oncol Biol Phys 74(2):553–561. doi:10.1016/j.ijrobp.2009.02.015
Kreimer AR, Clifford GM, Boyle P et al (2005) Human papillomavirus types in head and neck squamous cell carcinomas worldwide: a systematic review. Cancer Epidemiol Biomarkers Prev 14:467–475
Liang C, Marsit CJ, McClean MD, Nelson HH, Christensen BC, Haddad RI, Clark JR, Wein RO, Grillone GA, Houseman EA, Halec G, Waterboer T, Pawlita M, Krane JF, Kelsey KT (2012) Biomarkers of HPV in head and neck squamous cell carcinoma. Cancer Res 72(19):5004–5013. doi:10.1158/0008-5472.CAN-11-3277
Lin J, Albers AE, Qin J et al (2014) Prognostic significance of overexpressed p16INK4a in patients with cervical cancer: a meta-analysis. PLoS One 9:e106384
Marur S, D’souza G, Westra WH et al (2010) HPV-associated head and neck cancer: a virus-related cancer epidemic. Lancet Oncol 11:781–789
Masterson L, Moualed D, Liu ZW et al (2014) De-escalation treatment protocols for human papillomavirus-associated oropharyngeal squamous cell carcinoma: a systematic review and meta-analysis of current clinical trials. Eur J Cancer 50:2636–2648
Mclaughlin-Drubin ME, Crum CP, Munger K (2011) Human papillomavirus E7 oncoprotein induces KDM6A and KDM6B histone demethylase expression and causes epigenetic reprogramming. Proc Natl Acad Sci USA 108:2130–2135
Mclaughlin-Drubin ME, Park D, Munger K (2013) Tumor suppressor p16INK4A is necessary for survival of cervical carcinoma cell lines. Proc Natl Acad Sci USA 110:16175–16180
Mehanna H, Beech T, Nicholson T et al (2013) Prevalence of human papillomavirus in oropharyngeal and nonoropharyngeal head and neck cancer–systematic review and meta-analysis of trends by time and region. Head Neck 35:747–755
Melkane AE, Auperin A, Saulnier P, Lacroix L, Vielh P, Casiraghi O, Msakni I, Drusch F, Temam S (2014) Human papillomavirus prevalence and prognostic implication in oropharyngeal squamous cell carcinomas. Head Neck 36(2):257–265. doi:10.1002/hed.23302
Ndiaye C, Mena M, Alemany L et al (2014) HPV DNA, E6/E7 mRNA, and p16INK4a detection in head and neck cancers: a systematic review and meta-analysis. Lancet Oncol 15:1319–1331
O’sullivan B, Huang SH, Siu LL et al (2013) Deintensification candidate subgroups in human papillomavirus-related oropharyngeal cancer according to minimal risk of distant metastasis. J Clin Oncol 31:543–550
Paavonen J, Jenkins D, Bosch FX et al (2007) Efficacy of a prophylactic adjuvanted bivalent L1 virus-like-particle vaccine against infection with human papillomavirus types 16 and 18 in young women: an interim analysis of a phase III double-blind, randomised controlled trial. Lancet 369:2161–2170
Park K, Cho KJ, Lee M, Yoon DH, Kim J, Kim SY, Nam SY, Choi SH, Roh JL, Han MW, Lee SW, Song SY, Back JH, Kim SB (2013) p16 immunohistochemistry alone is a better prognosticator in tonsil cancer than human papillomavirus in situ hybridization with or without p16 immunohistochemistry. Acta Otolaryngol 133(3):297–304. doi:10.3109/00016489.2012.741327
Park WS, Ryu J, Cho KH, Choi MK, Moon SH, Yun T, Chun BS, Lee GK, Ahn HJ, Lee JH, Vermeer P, Jung YS (2012) Human papillomavirus in oropharyngeal squamous cell carcinomas in Korea: use of G1 cycle markers as new prognosticators. Head Neck 34(10):1408–1417. doi:10.1002/hed.21939
Pauck A, Lener B, Hoell M et al (2014) Depletion of the cdk inhibitor p16INK4a differentially affects proliferation of established cervical carcinoma cells. J Virol 88:5256–5262
Perrone F, Gloghini A, Cortelazzi B et al (2011) Isolating p16-positive/HPV-negative oropharyngeal cancer: an effort worth making. Am J Surg Pathol 35:774–777 (author reply 777–778)
Pignon JP, Le Maitre A, Maillard E et al (2009) Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): an update on 93 randomised trials and 17,346 patients. Radiother Oncol 92:4–14
Qian X, Wagner S, Ma C et al (2014) Prognostic significance of ALDH1A1-positive cancer stem cells in patients with locally advanced, metastasized head and neck squamous cell carcinoma. J Cancer Res Clin Oncol 140:1151–1158
Quabius ES, Haag J, Kuhnel A et al (2015) Geographical and anatomical influences on human papillomavirus prevalence diversity in head and neck squamous cell carcinoma in Germany. Int J Oncol 46:414–422
Ragin CC, Taioli E (2007) Survival of squamous cell carcinoma of the head and neck in relation to human papillomavirus infection: review and meta-analysis. Int J Cancer 121:1813–1820
Rainsbury JW, Ahmed W, Williams HK et al (2013) Prognostic biomarkers of survival in oropharyngeal squamous cell carcinoma: systematic review and meta-analysis. Head Neck 35:1048–1055
Rcoreteam (2014) R Statistical Software. A language and environment for statistical computing. R Foundation for Statistical Computing. R Version 3.1.0. In: Software RS (ed)URL, Vienna, Austria
Rieckmann T, Tribius S, Grob TJ et al (2013) HNSCC cell lines positive for HPV and p16 possess higher cellular radiosensitivity due to an impaired DSB repair capacity. Radiother Oncol 107:242–246
Rietbergen MM, Brakenhoff RH, Bloemena E, Witte BI, Snijders PJ, Heideman DA, Boon D, Koljenovic S, Baatenburg-de Jong RJ, Leemans CR (2013) Human papillomavirus detection and comorbidity: critical issues in selection of patients with oropharyngeal cancer for treatment de-escalation trials. Ann Oncol 24(11):2740–2745. doi:10.1093/annonc/mdt319
Rietbergen MM, Snijders PJ, Beekzada D et al (2014) Molecular characterization of p16-immunopositive but HPV DNA-negative oropharyngeal carcinomas. Int J Cancer 134:2366–2372
Robinson M, Sloan P, Shaw R (2010) Refining the diagnosis of oropharyngeal squamous cell carcinoma using human papillomavirus testing. Oral Oncol 46:492–496
Rodrigo JP, Heideman DA, Garcia-Pedrero JM et al (2014) Time trends in the prevalence of HPV in oropharyngeal squamous cell carcinomas in northern Spain (1990–2009). Int J Cancer 134:487–492
Salazar CR, Anayannis N, Smith RV, Wang Y, Haigentz M Jr, Garg M, Schiff BA, Kawachi N, Elman J, Belbin TJ, Prystowsky MB, Burk RD, Schlecht NF (2014) Combined P16 and human papillomavirus testing predicts head and neck cancer survival. Int J Cancer 135(10):2404–2412. doi:10.1002/ijc.28876
Schache AG, Liloglou T, Risk JM et al (2011) Evaluation of human papilloma virus diagnostic testing in oropharyngeal squamous cell carcinoma: sensitivity, specificity, and prognostic discrimination. Clin Cancer Res 17:6262–6271
Schlecht NF, Brandwein-Gensler M, Nuovo GJ et al (2011) A comparison of clinically utilized human papillomavirus detection methods in head and neck cancer. Mod Pathol 24:1295–1305
Shi W, Kato H, Perez-Ordonez B et al (2009) Comparative prognostic value of HPV16 E6 mRNA compared with in situ hybridization for human oropharyngeal squamous carcinoma. J Clin Oncol 27:6213–6221
Singhi AD, Westra WH (2010) Comparison of human papillomavirus in situ hybridization and p16 immunohistochemistry in the detection of human papillomavirus-associated head and neck cancer based on a prospective clinical experience. Cancer 116:2166–2173
Smeets SJ, Hesselink AT, Speel EJ et al (2007) A novel algorithm for reliable detection of human papillomavirus in paraffin embedded head and neck cancer specimen. Int J Cancer 121:2465–2472
Smith EM, Wang D, Kim Y, Rubenstein LM, Lee JH, Haugen TH, Turek LP (2008) P16INK4a expression, human papillomavirus, and survival in head and neck cancer. Oral Oncol 44(2):133–142. doi:10.1016/j.oraloncology.2007.01.010
Stephen JK, Divine G, Chen KM, Chitale D, Havard S, Worsham MJ (2013) Significance of p16 in site-specific HPV positive and HPV negative head and neck squamous cell carcinoma. Cancer Clin Oncol 2(1):51–61. doi:10.5539/cco.v2n1p51
Talis AL, Huibregtse JM, Howley PM (1998) The role of E6AP in the regulation of p53 protein levels in human papillomavirus (HPV)-positive and HPV-negative cells. J Biol Chem 273:6439–6445
Termine N, Panzarella V, Falaschini S et al (2008) HPV in oral squamous cell carcinoma vs head and neck squamous cell carcinoma biopsies: a meta-analysis (1988–2007). Ann Oncol 19:1681–1690
Tinhofer I, Johrens K, Keilholz U et al (2015) Contribution of human papilloma virus to the incidence of squamous cell carcinoma of the head and neck in a European population with high smoking prevalence. Eur J Cancer
Tran N, Rose BR, O’brien CJ (2007) Role of human papillomavirus in the etiology of head and neck cancer. Head Neck 29:64–70
Upile NS, Shaw RJ, Jones TM et al (2014) Squamous cell carcinoma of the head and neck outside the oropharynx is rarely human papillomavirus related. Laryngoscope 124:2739–2744
Weinberger PM, Merkley MA, Khichi SS, Lee JR, Psyrri A, Jackson LL, Dynan WS (2010) Human papillomavirus-active head and neck cancer and ethnic health disparities. Laryngoscope 120(8):1531–1537. doi:10.1002/lary.20984
Weinberger PM, Yu Z, Haffty BG et al (2006) Molecular classification identifies a subset of human papillomavirus–associated oropharyngeal cancers with favorable prognosis. J Clin Oncol 24:736–747
Weiss D, Koopmann M, Rudack C (2011) Prevalence and impact on clinicopathological characteristics of human papillomavirus-16 DNA in cervical lymph node metastases of head and neck squamous cell carcinoma. Head Neck 33:856–862
Westra WH (2014) Detection of human papillomavirus (HPV) in clinical samples: evolving methods and strategies for the accurate determination of HPV status of head and neck carcinomas. Oral Oncol 50:771–779
Wiest T, Schwarz E, Enders C et al (2002) Involvement of intact HPV16 E6/E7 gene expression in head and neck cancers with unaltered p53 status and perturbed pRb cell cycle control. Oncogene 21:1510–1517
Wittekindt C, Gultekin E, Weissenborn SJ, Dienes HP, Pfister HJ, Klussmann JP (2005) Expression of p16 protein is associated with human papillomavirus status in tonsillar carcinomas and has implications on survival. Adv Otorhinolaryngol 62:72–80. doi:10.1159/000082474
Xie X, Piao L, Bullock BN et al (2013) Targeting HPV16 E6-p300 interaction reactivates p53 and inhibits the tumorigenicity of HPV-positive head and neck squamous cell carcinoma. Oncogene
Xu Y, Liu S, Yi H, Wang J, Luo Y, Yin S (2015) Low prevalence of human papillomavirus in head and neck squamous cell carcinoma in Chinese patients. J Med Virol 87(2):281–286. doi:10.1002/jmv.24052
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Coordes, A., Lenz, K., Qian, X. et al. Meta-analysis of survival in patients with HNSCC discriminates risk depending on combined HPV and p16 status. Eur Arch Otorhinolaryngol 273, 2157–2169 (2016). https://doi.org/10.1007/s00405-015-3728-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-015-3728-0