Abstract
Purpose
The aim of this study is to investigate the spectrum of underlying disease in children with torticollis.
Methods
We investigated the spectrum of underlying disease and to evaluate the clinical features of the children presented with torticollis in the last 2 years.
Results
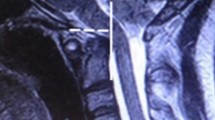
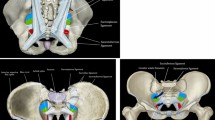
Of the 20 children (13 girls and 7 boys with the mean age of 8 years, ranging 2 months–12 years), eight of them have craniospinal pathologies (cerebellar tumors in three, exophytic brain stem glioma, eosinophilic granuloma of C2 vertebra, neuroenteric cyst of the spinal cord, Chiari type 3 malformation, arachnoid cysts causing brainstem compression, and cerebellar empyema), followed by osseous origin in five (congenital vertebral anomalies including hemivertebrae, blocked vertebra, and segmentation anomalies), two muscular torticollis (soft tissue inflammation due to subclavian artery catheterization, myositis ossificans with sternocleidomastoid muscle atrophy), and ocular (congenital cataract and microphthalmia), Sandifer syndrome, paroxysmal torticollis, retropharyngeal abscess each in one patients were detected. Ten patients underwent surgery; two patients received medical therapy for reflux and benign paroxysmal torticollis; and one patient with torticollis due to muscle spasm and soft tissue inflammation was treated with physiotherapy.
Conclusions
Various underlying disorders from relatively benign to life-threatening conditions may present with torticollis. The first step should be always a careful and complete physical examination, which must include all systems. Imaging must be performed for ruling out underlying life-threatening diseases in children with torticollis, particularly, if acquired neurological symptoms exist. Besides craniospinal tumors, ophthalmological problems and central nervous system infections should also be kept in mind. Moreover, early diagnosis of these disorders will reduce mortality and morbidity. Therefore, alertness of clinicians in pediatric and pediatric neurosurgery practice must be increased about this alert symptom.







Similar content being viewed by others
References
Per H, Canpolat M, Tümtürk A, Gumuş H, Gokoglu A, Yikilmaz A, Özmen S, KaçarBayram A, Poyrazoğlu HG, Kumandas S, Kurtsoy A (2014) Different etiologies of acquired torticollis in childhood. Childs Nerv Syst 30:431–440
Fafara-Leś A, Kwiatkowski S, Maryńczak L, Kawecki Z, Adamek D, Herman-Sucharska I, Kobylarz K (2014) Torticollis as a first sign of posterior fossa and cervical spinal cord tumors in children. Childs Nerv Syst 30:425–430
Cheng JC, Au AW (1994) Infantile torticollis: a review of 624 cases. J Pediatr Orthop 14:802–808
Tomczak KK, Rosman NP (2013) Torticollis. J Child Neurol 28:365–378
Kumandaş S, Per H, Gümüş H, Tucer B, Yikilmaz A, Kontaş O, Coşkun A, Kurtsoy A (2006) Torticollis secondary to posterior fossa and cervical spinal cord tumors: report of five cases and literature review. Neurosurg Rev 29:333–338
Herman MJ, Wolf M (2013) Torticollis in children. Curr Orthop Pract 24:598–603
Gray GM, Tasso KH (2009) Differential diagnosis of torticollis: a case report. Pediatr Phys Ther 21:369–374
Gupta AK, Roy DR, Conlan ES, Crawford AH (1996) Torticollis secondary to posterior fossa tumors. J Pediatr Orthop 16:505–507
Turgut M, Akalan N, Bertan V, Erbengi A, Eryilmaz M (1995) Acquired torticollis as the only presenting symptom in children with posterior fossa tumors. Childs Nerv Syst 11:86–88
Per H, Koç KR, Gümüş H, Canpolat M, Kumandaş S (2008) Cervical eosinophilic granuloma and torticollis: a case report and review of the literature. J Emerg Med 35:389–392
Shay V, Fattal-Valevski A, Beni-Adani L, Constantini S (2012) Diagnostic delay of pediatric brain tumors in Israel: a retrospective risk factor analysis. Childs Nerv Syst 28:93–100
Hensinger RN (1991) Congenital anomalies of the cervical spine. Clin Orthop Relat Res 264:16–38
Daya H, Lo S, Papsin BC, Zachariasova A, Murray H, Pirie J, Laughlin S, Blaser S (2005) Retropharyngeal and parapharyngeal infections in children: the Toronto experience. Int J Pediatr Otorhinolaryngol 69:81–86
Haque S, Bilal Shafi BB, Kaleem M (2012) Imaging of torticollis in children. Radiographics 32:557–571
Lalakea MI, Messner AH (1999) Retropharyngeal abscess management in children: current practices. Otolaryngol Head Neck Surg 121:398–405
Guille JT, Sherk HH (2002) Congenital osseous anomalies of the upper and lower cervical spine in children. J Bone Joint Surg Am 84:227–288
Ulmer JL, Elster AD, Ginsberg LE, Williams DW 3rd (1993) Klippel-Feil Syndrome: CT and MR of acquired and congenital abnormalities of cervical spine and cord. J Comput Assist Tomogr 17:215–224
Williams CRP, O’Flynn E, Clarke NMP, Morris RJ (1996) Torticollis secondary to ocular pathology. J Bone Joint Surg (Br) 78B:620–624
Dikici K, Kızılkaya M (2002) Ocular causes of abnormal head posture. Cerrahpaşa J Med 33:42–46
Vandenplas Y, Hassall E (2002) Mechanisms of gastroesophageal reflux and gastroesophageal reflux disease. J Pediatr Gastroenterol Nutr 35:119–136
Orenstein S, Peters J, Khan S, Yousef N, Hussain SZ (2004) The esophagus. In: Berhman RE, Kliegman RM, Jenson HB (eds) Nelson textbook of pediatrics, 17th edition. Saunders Company, 1217–1227
Rudolph CD, Mazur LJ, Liptak GS, Baker RD, Boyle JT, Colletti RB, Gerson WT, Werlin SL (2001) Guidelines for evaluation and treatment of gastroesophageal reflux in infants and children: recommendations of the North American Society for Pediatric Gastroenterology and Nutrition. J Pediatr Gastroenterol Nutr 32:1–31
Rosman NP, Douglass LM, Sharif UM, Paolini J (2009) The neurology of benign paroxysmal torticollis of infancy: report of 10 new cases and review of the literature. J Child Neurol 24:155–160
Conflict of interest
The author(s) declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Tumturk, A., Kaya Ozcora, G., Kacar Bayram, A. et al. Torticollis in children: an alert symptom not to be turned away. Childs Nerv Syst 31, 1461–1470 (2015). https://doi.org/10.1007/s00381-015-2764-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2764-9