Abstract
Purpose
To examine the prevalence, symptomatology, and risk factors for nocturia using data from an internet-based questionnaire conducted in China, South Korea, and Taiwan.
Methods
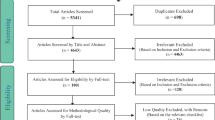
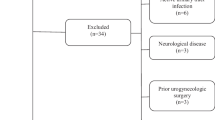
Data from a cross-sectional, population-representative, internet-based study conducted among men and women aged ≥ 40 years were analysed post hoc. Nocturia prevalence and bother were analysed by sex and age group, and with regard to comorbid conditions and lower urinary tract symptoms (LUTS). Multivariate and univariate logistic regression models to identify risk factors for nocturia were constructed, with nocturia involving ≥ 2 nocturnal voids as the dependent variable.
Results
Among the 8284 participants, the prevalence of nocturia involving ≥ 1, ≥ 2, or ≥ 3 voids was slightly higher for women (76.1, 37.3, and 17.5%, respectively) compared with men (74.0, 34.5, and 15.5%, respectively). The prevalence and associated bother of nocturia increased with age. Greater proportions of patients with comorbid conditions or wet/more severe overactive bladder syndrome (OAB) experienced nocturia than those without. Multivariate analysis identified that female sex, age > 60 years, diabetes, cardiac disease, body mass index, International Prostate Symptom Score (IPSS) voiding score, stress urinary incontinence, wet OAB, and Hospital Anxiety And Depression Scale (HADS) anxiety score were associated with ≥ 2 nocturnal voids. Hypertension was associated with ≥ 2 nocturnal voids in women but not men, and alcohol consumption in men but not women.
Conclusions
Nocturia is a common and bothersome condition affecting a large proportion of men and women aged ≥ 40 years in China, South Korea, and Taiwan. Factors associated with nocturia included age, sex, comorbid conditions, and LUTS.
Trial registration
This study is registered at ClinicalTrials.gov: NCT02618421.


Similar content being viewed by others
Abbreviations
- ANOVA:
-
Analysis of variance
- ESOMAR:
-
World Association for Social, Opinion and Market Research
- HADS:
-
Hospital Anxiety and Depression Scale
- HRQoL:
-
Health-related quality of life
- ICS:
-
International Continence Society
- IIEF:
-
International Index of Erectile Function
- IPSS:
-
International Prostate Symptom Score
- OAB:
-
Overactive bladder syndrome
- OAB-q SF:
-
Overactive Bladder Questionnaire, Short Form
- OABSS:
-
Overactive Bladder Symptom Score
- PPBC:
-
Patient Perception of Bladder Condition
- SQoL-F:
-
Sexual Quality of Life—Female questionnaire
- WLQ:
-
Work Limitations Questionnaire
References
Abrams P, Cardozo L, Fall M et al (2002) The standardisation of terminology of lower urinary tract function: report from the standardisation sub-committee of the international continence society. Neurourol Urodyn 21:167–178
van Kerrebroeck P, Abrams P, Chaikin D et al (2002) The standardisation of terminology in nocturia: report from the standardisation sub-committee of the international continence society. Neurourol Urodyn 21:179–183
Andersson F, Anderson P, Holm-Larsen T, Piercy J, Everaert K, Holbrook T (2016) Assessing the impact of nocturia on health-related quality-of-life and utility: results of an observational survey in adults. J Med Econ 19:1200–1206
Dani H, Esdaille A, Weiss JP (2016) Nocturia: aetiology and treatment in adults. Nat Rev Urol 13:573–583
Tikkinen KA, Johnson TM 2nd, Tammela TL et al (2010) Nocturia frequency, bother, and quality of life: how often is too often? A population-based study in Finland. Eur Urol 57:488–496
Zumrutbas AE, Bozkurt AI, Alkis O, Toktas C, Cetinel B, Aybek Z (2016) The prevalence of nocturia and nocturnal polyuria: can new cutoff values be suggested according to age and sex? Int Neurourol J 20:304–310
Bower WF, Whishaw DM, Khan F (2017) Nocturia as a marker of poor health: causal associations to inform care. Neurourol Urodyn 36:697–705
Fan Y, Wei F, Lang Y, Qi W (2015) Meta-analysis of nocturia and risk of all-cause mortality in adult population. Int J Cardiol 195:120–122
Endeshaw YW, Schwartz AV, Stone K et al (2016) Nocturia, insomnia symptoms and mortality among older men: the health, aging and body composition study. J Clin Sleep Med 12:789–796
Kupelian V, Fitzgerald MP, Kaplan SA, Norgaard JP, Chiu GR, Rosen RC (2011) Association of nocturia and mortality: results from the third national health and nutrition examination survey. J Urol 185:571–577
Liu HY, Chung MS, Wang HJ, Liu RT, Chuang YC (2016) Nocturia indicates a poor health status and increases mortality in male patients with type 2 diabetes mellitus. Int Urol Nephrol 48:1209–1214
Ho LY, Chu PS, Consigliere DT et al (2018) Symptom prevalence, bother, and treatment satisfaction in men with lower urinary tract symptoms in Southeast Asia: a multinational, cross-sectional survey. World J Urol 36:79–86
Lee YS, Lee KS, Jung JH et al (2011) Prevalence of overactive bladder, urinary incontinence, and lower urinary tract symptoms: results of Korean EPIC study. World J Urol 29:185–190
Wang Y, Hu H, Xu K, Wang X, Na Y, Kang X (2015) Prevalence, risk factors and the bother of lower urinary tract symptoms in China: a population-based survey. Int Urogynecol J 26:911–919
Kim SY, Bang W, Kim MS, Park B, Kim JH, Choi HG (2017) Analysis of the prevalence and factors associated with nocturia in adult Korean men. Sci Rep 7:41714
Zhang L, Zhu L, Xu T et al (2015) A population-based survey of the prevalence, potential risk factors, and symptom-specific bother of lower urinary tract symptoms in adult Chinese women. Eur Urol 68:97–112
Kim TH, Han DH, Lee KS (2014) The prevalence of lower urinary tract symptoms in Korean men aged 40 years or older: a population-based survey. Int Neurourol J 18:126–132
Huang MH, Chiu AF, Wang CC, Kuo HC (2012) Prevalence and risk factors for nocturia in middle-aged and elderly people from public health centers in Taiwan. Int Braz J Urol 38:818–824
Lee YJ, Jeong SJ, Byun SS, Lee JJ, Han JW, Kim KW (2012) Prevalence and correlates of nocturia in community-dwelling older men: results from the Korean longitudinal study on health and aging. Korean J Urol 53:263–267
Zhang X, Zhang J, Chen J et al (2011) Prevalence and risk factors of nocturia and nocturia-related quality of life in the Chinese population. Urol Int 86:173–178
Wang Y, Hu H, Xu K et al (2015) Prevalence, risk factors, and symptom bother of nocturia: a population-based survey in China. World J Urol 33:677–683
Chapple C, Castro-Diaz D, Chuang YC et al (2017) Prevalence of lower urinary tract symptoms in China, Taiwan, and South Korea: results from a cross-sectional, population-based study. Adv Ther 34:1953–1965
ESOMAR (2017) ESOMAR guideline for online research. Available from https://www.esomar.org/uploads/public/knowledge-and-standards/codes-and-guidelines/ESOMAR_Guideline-for-online-research.pdf, accessed June 23 2017
Madhu C, Coyne K, Hashim H, Chapple C, Milsom I, Kopp Z (2015) Nocturia: risk factors and associated comorbidities; findings from the EpiLUTS study. Int J Clin Pract 69:1508–1516
Tam CA, Helfand BT, Erickson BA (2017) The relationship between diabetes, diabetes severity, diabetes biomarkers, and the presence of lower urinary tract symptoms: findings from the national health and nutrition examination survey. Urology 105:141–148
Yoshimura K (2012) Correlates for nocturia: a review of epidemiological studies. Int J Urol 19:317–329
Wang S, Mitu GM, Hirschberg R (2008) Osmotic polyuria: an overlooked mechanism in diabetic nephropathy. Nephrol Dial Transplant 23:2167–2172
Fitzgerald MP, Litman HJ, Link CL, McKinlay JB, BACH Survey Investigators (2007) The association of nocturia with cardiac disease, diabetes, body mass index, age and diuretic use: results from the BACH survey. J Urol 177:1385–1389
Feldstein CA (2013) Nocturia in arterial hypertension: a prevalent, underreported, and sometimes underestimated association. J Am Soc Hypertens 7:75–84
Wen L, Wen YB, Wang ZM et al (2015) Risk factors of nocturia (two or more voids per night) in Chinese people older than 40 years. Neurourol Urodyn 34:566–570
Chung MS, Chuang YC, Lee JJ, Lee WC, Chancellor MB, Liu RT (2014) Prevalence and associated risk factors of nocturia and subsequent mortality in 1301 patients with type 2 diabetes. Int Urol Nephrol 46:1269–1275
Hirayama A, Torimoto K, Mastusita C et al (2013) Evaluation of factors influencing the natural history of nocturia in elderly subjects: results of the Fujiwara-kyo study. J Urol 189:980–986
Varella LR, Bezzerra da Silva R, de Oliveira MCE, Melo PH, Maranhao TM, Micussi MT (2016) Assessment of lower urinary tract symptoms in different stages of menopause. J Phys Ther Sci 28:3116–3121
Lin TL, Ng SC, Chen YC, Hu SW, Chen GD (2005) What affects the occurrence of nocturia more: menopause or age? Maturitas 50:71–77
Shigehara K, Izumi K, Mizokami A, Namiki M (2017) Testosterone deficiency and nocturia: a review. World J Mens Health 35:14–21
Acknowledgements
The authors would like to thank the participants of the study for their time and Nanjangud Shankar Narasimha Murthy (Department of Community Medicine—SIMSRC, Bangalore, India) and Raviprakash Koni (Stratycon Business Solutions Pvt. Ltd., Bangalore, India) for statistical analyses. Medical writing support was provided by Emily Howard of Envision Scientific Solutions, funded by Astellas Pharma Global Development, Inc.
Funding
This study was funded by Astellas Pharma Singapore Pte. Ltd. Medical writing support was funded by Astellas Pharma Global Development, Inc.
Author information
Authors and Affiliations
Contributions
PMC: protocol/project development, data analysis, and manuscript writing/editing. SPL: protocol/project development, data analysis, and manuscript writing/editing. YCC: protocol/project development, data analysis, and manuscript writing/editing. KSL: protocol/project development, data analysis, and manuscript writing/editing. TKY: protocol/project development, data analysis, and manuscript writing/editing. LL: protocol/project development, data analysis, and manuscript writing/editing. JYW: protocol/project development, data analysis, and manuscript writing/editing. ML: protocol/project development, data analysis, and manuscript writing/editing. BS: protocol/project development, data collection or management, data analysis, and manuscript writing/editing. JJJ: protocol/project development, data analysis, and manuscript writing/editing
Corresponding author
Ethics declarations
Conflict of interest
All authors have acted as consultants for Astellas during a meeting to discuss the publications from this study. Po-Ming Chow has received a research grant from Astellas. Shih-Ping Liu, Yao-Chi Chuang, Kyu-Sung Lee, Limin Liao, Jian-ye Wang, and Ming Liu report no conflicts of interest. Tag Keun Yoo has received personal fees for lecturing from Hanmi Pharmaceutical and Pfizer, and has received grants and personal fees from Astellas to act as a consultant. Budiwan Sumarsono and Jar Jar Jong are employees of Astellas.
Ethical approval
For this type of study, formal consent is not required. As a survey-based study, institutional review board approval was not considered necessary, although the principles of the Declaration of Helsinki were followed and the study was performed in compliance with World Association for Social, Opinion, and Market Research (ESOMAR) guidelines and Good Clinical Practice. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chow, PM., Liu, SP., Chuang, YC. et al. The prevalence and risk factors of nocturia in China, South Korea, and Taiwan: results from a cross-sectional, population-based study. World J Urol 36, 1853–1862 (2018). https://doi.org/10.1007/s00345-018-2329-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2329-0