Abstract
Purpose
To assess whether the PSA level (threshold 4 ng/mL) is a prognostic factor in biochemical recurrence-free survival in men with prostate cancer (PCa) with an initial PSA level <10 ng/mL who underwent robotic-assisted laparoscopic radical prostatectomy (RARLP).
Methods
We prospectively recruited data for consecutive patients treated by RARLP for PCa with an initial PSA level below 10 ng/mL between 2003 and 2011 at our institution. We divided the population into two groups: patients with a PSA level below 4 ng/mL (G1; n = 53) and patients with a PSA level between 4 and 10 ng/mL (G2; n = 371). Biochemical recurrence was defined as a single increase in PSA greater than 0.2 ng/mL after surgery. Multivariate analysis was used to assess prognostic factors of recurrence-free survival.
Results
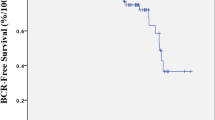
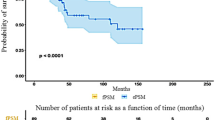
Overall, 424 patients were included, and the median age was 62 (58–67) years. The median PSA was 5.8 ng/mL (4.8–7.7 ng/mL). Overall, 6 patients from G1 and 34 patients from G2 experienced a biochemical recurrence. Overall, the 5-year recurrence-free survival rate was 86.6 %. The PSA level at diagnosis (under or over 4 ng/mL) was not significantly linked to recurrence-free survival (HR = 0.59, p = 0.25). However, positive margins and a Gleason score >7 on the specimen were significantly linked to recurrence-free survival with respective hazard ratios of 4.30 (p < 0.0001) and 6.18 (p < 0.0001), respectively.
Conclusion
A PSA level <4 ng/mL alone appears to be obsolete as a cut-off to define a population of men likely to have indolent disease.

Similar content being viewed by others
References
Schröder FH, Hugosson J, Roobol MJ et al (2009) Screening and prostate-cancer mortality in a randomized European study. N Engl J Med 36:1320–1328. doi:10.1056/NEJMoa0810084
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Murray T, Thun MJ (2008) Cancer statistics, 2008. CA Cancer J Clin 58:71–96. doi:10.3322/CA.2007.0010
Schröder FH, Hugosson J, Roobol MJ et al (2012) Prostate-cancer mortality at 11 years of follow-up. N Engl J Med 366:981–990. doi:10.1056/NEJMoa1113135
Rébillard X, Grosclaude P, Lebret T, Patard JJ, Pfister C, Richaud P, Rigaud J, Salomon L, Soulié M (2010) Projected incidence and mortality from urologic cancer in France in 2010. Prog Urol Suppl 4:S211–S214. doi:10.1016/S1166-7087(10)70041-5
Freedland SJ, Mangold LA, Walsh PC, Partin AW (2005) The prostatic specific antigen era is alive and well: prostatic specific antigen and biochemical progression following radical prostatectomy. J Urol 174:1276–1281
Andriole GL, Crawford ED, Grubb RL 3rd (2009) Mortality results from a randomized prostate-cancer screening trial. N Engl J Med 360:1310–1319. doi:10.1056/NEJMoa0810696
Crawford ED, Moul JW, Rove KO, Pettaway CA, Lamerato LE, Hughes A (2011) Prostate-specific antigen 1.5–4.0 ng/mL: a diagnostic challenge and danger zone. BJU Int 108:1743–1749. doi:10.1111/j.1464-410X.2011.10224.x
Tang P, Sun L, Uhlman MA, Robertson CN, Polascik TJ, Albala DM, Donatucci CF, Moul JW (2010) Initial prostate specific antigen 1.5 ng/ml or greater in men 50 years old or younger predicts higher prostate cancer risk. J Urol 183:946–950. doi:10.1016/j.juro.2009.11.021
Thompson IM, Pauler DK, Goodman PJ, Tangen CM, Lucia MS, Parnes HL, Minasian LM, Ford LG, Lippman SM, Crawford ED, Crowley JJ, Coltman CA Jr (2004) Prevalence of prostate cancer among men with a prostate-specific antigen level < or = 4.0 ng per milliliter. N Engl J Med 350:2239–2246
Thompson IM, Ankerst DP, Chi C, Goodman PJ, Tangen CM, Lucia MS, Feng Z, Parnes HL, Coltman CA Jr (2006) Assessing prostate cancer risk: results from the prostate cancer prevention trial. J Natl Cancer Inst 98:529–534
Beauval JB, Ploussard G, Soulié M, Pfister C, Van Agt S, Vincendeau S, Larue S, Rigaud J, Gaschignard N, Rouprêt M, Drouin S, Peyromaure M, Long JA, Iborra F, Vallancien G, Rozet F, Salomon L; Members of Committee of Cancerology of the French Association of Urology (CCAFU) (2012) Pathologic findings in radical prostatectomy specimens from patients eligible for active surveillance with highly selective criteria: a multicenter study. Urology 80:656–660. doi:10.1016/j.urology.2012.04.051
Klotz L, Zhang L, Lam A, Nam R, Mamedov A, Loblaw A (2010) Clinical results of long-term follow-up of a large, active surveillance cohort with localized prostate cancer. J Clin Oncol 28:126–131. doi:10.1200/JCO.2009.24.2180
Heidenreich A, Bellmunt J, Bolla M, Joniau S, Mason M, Matveev V, Mottet N, Schmid HP, van der Kwast T, Wiegel T, Zattoni F (2011) EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and treatment of clinically localised disease. Eur Urol 59:61–71
Drouin SJ, Vaessen C, Misraï V, Ferhi K, Bitker MO, Chartier-Kastler E, Haertig A, Richard F, Rouprêt M (2009) Oncologic and functional outcomes after robot-assisted laparoscopic radical prostatectomy. Prog Urol 19:158–164. doi:10.1016/j.purol.2008.11.009
Diblasio CJ, Kattan MW (2003) Use of nomograms to predict the risk of disease recurrence after definitive local therapy for prostate cancer. Urology 62(Suppl 1):9–18
Bill-Axelson A, Holmberg L, Ruutu M, Häggman M, Andersson SO, Bratell S, Spångberg A, Busch C, Nordling S, Garmo H, Palmgren J, Adami HO, Norlén BJ, Johansson JE; Scandinavian Prostate Cancer Group Study No. 4 (2005) Radical prostatectomy versus watchful waiting in early prostate cancer. N Engl J Med 352:1977–1984
Mitsuzuka K, Narita S, Koie T, Kaiho Y, Tsuchiya N, Yoneyama T, Kakoi N, Kawamura S, Tochigi T, Habuchi T, Ohyama C, Arai Y (2013) Pathological and biochemical outcomes after radical prostatectomy in men with low-risk prostate cancer meeting the Prostate Cancer International: active Surveillance criteria. BJU Int. doi:10.1111/j.1464-410X.2012.11658.x
Drouin SJ, Vaessen C, Hupertan V, Comperat E, Misraï V, Haertig A, Bitker MO, Chartier-Kastler E, Richard F, Rouprêt M (2009) Comparison of mid-term carcinologic control obtained after open, laparoscopic, and robot-assisted radical prostatectomy for localized prostate cancer. World J Urol 27:599–605. doi:10.1007/s00345-009-0379-z
Drouin SJ, Comperat E, Cussenot O, Bitker MO, Haertig A, Roupret M (2012) Clinical characteristics and pathologic findings in patients eligible for active surveillance who underwent radical prostatectomy. Urol Oncol 30:402–407
Stephenson AJ, Jones JS, Hernandez AV, Ciezki JP, Gong MC, Klein EA (2009) Analysis of T1c prostate cancers treated at very low prostate-specific antigen levels. Eur Urol 55:610–616. doi:10.1016/j.eururo.2008.07.005
Cooner WH, Mosley BR, Rutherford CL Jr, Beard JH, Pond HS, Terry WJ, Igel TC, Kidd DD (1990) Prostate cancer detection in a clinical urological practice by ultrasonography, digital rectal examination and prostate specific antigen. J Urol 143:1146–1152
Ohori M, Wheeler TM, Dunn JK, Stamey TA, Scardino PT (1994) The pathological features and prognosis of prostate cancer detectable with current diagnostic tests. J Urol 152:1714–1720
Smith RA, Cokkinides V, von Eschenbach AC, Levin B, Cohen C, Runowicz CD, Sener S, Saslow D, Eyre HJ, Society American Cancer (2002) American Cancer society guidelines for the early detection of cancer. CA Cancer J Clin 52:8–22
Schröder FH, Roobol MJ, Andriole GL, Fleshner N (2009) Defining increased future risk for prostate cancer: evidence from a population based screening cohort. J Urol 181:69–74. doi:10.1016/j.juro.2008.09.012
Park KK, Lee SH, Choi YD, Chung BH (2012) Optimal baseline prostate-specific antigen level to distinguish risk of prostate cancer in healthy men between 40 and 69 years of age. J Korean Med Sci 27:40–45. doi:10.3346/jkms.2012.27.1.40
Vickers AJ, Lilja H (2012) Predicting prostate cancer many years before diagnosis: how and why? World J Urol 30(2):131–135. doi:10.1007/s00345-011-0795-8
Thompson IM, Ankerst DP, Chi C, Lucia MS, Goodman PJ, Crowley JJ, Parnes HL, Coltman CA Jr (2005) Operating characteristics of prostate-specific antigen in men with an initial PSA level of 3.0 ng/ml or lower. JAMA 294:66–70
Krumholtz JS, Carvalhal GF, Ramos CG, Smith DS, Thorson P, Yan Y, Humphrey PA, Roehl KA, Catalona WJ (2002) Prostate-specific antigen cutoff of 2.6 ng/mL for prostate cancer screening is associated with favorable pathologic tumor features. Urology 60:469–473
Nguyen K, Eltz S, Drouin SJ, Comperat E, Audenet F, Renard-Penna R, Bitker MO, Chartier-Kastler E, Richard F, Cussenot O, Rouprêt M (2009) Oncologic outcome after radical prostatectomy in men with PSA values above 20 ng/ml: a monocentric experience. World J Urol 27:653–658. doi:10.1007/s00345-009-0419-8
Lughezzani G, Gallina A, Larcher A et al (2012) Radical prostatectomy represents an effective treatment in patients with specimen-confined high pathological Gleason score prostate cancer. BJU Int. doi:10.1111/j.1464-410X.2012.11114.x
Ritch CR, Morrison BF, Hruby G, Coard KC, Mayhew R, Aiken W, Benson MC, McKiernan JM (2012) Pathological outcome and biochemical recurrence-free survival after radical prostatectomy in African-American, Afro-Caribbean (Jamaican) and Caucasian-American men: an international comparison. BJU Int. doi:10.1111/j.1464-410X.2012.11540.x
Berglund RK, Masterson TA, Vora KC, Eggener SE, Eastham JA, Guillonneau BDJ (2008) Pathological upgrading and up staging with immediate repeat biopsy in patients eligible for active surveillance. Urology 180:1964–1967. doi:10.1016/j.juro.2008.07.051
Xylinas E, Yates DR, Renard-Penna R, Seringe E, Bousquet JC, Comperat E, Bitker MO, Grenier P, Rouprêt M (2011) Role of pelvic phased array magnetic resonance imaging in staging of prostate cancer specifically in patients diagnosed with clinically locally advanced tumours by digital rectal examination. World J Urol. doi:10.1007/s00345-011-0811-z
Conflict of interest
The authors state that they have no conflicts of interest to disclose regarding the current manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dariane, C., Le Cossec, C., Drouin, S.J. et al. Comparison of oncologic outcomes after radical prostatectomy in men diagnosed with prostate cancer with PSA levels below and above 4 ng/mL. World J Urol 32, 481–487 (2014). https://doi.org/10.1007/s00345-013-1089-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-013-1089-0