Abstract
Purpose
Previous studies have included a limited number of randomized controlled trials (RCTs) and compared limited parameters after treatment with imidafenacin and other anticholinergic drugs (ADs) for overactive bladder syndrome (OAB), and controversy about the superiority of these ADs still remains. We aim to update the evidence and provide better clinical guidance.
Methods
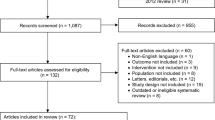
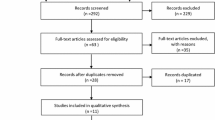
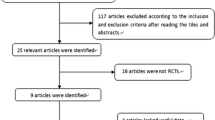
A systematic search of PubMed, Embase, ClinicalTrial.gov and Cochrane Library Central Register of Controlled Trials was conducted from January 2007 to April 2019. Meta-analysis of all published RCTs comparing imidafenacin with other ADs in patients with OAB was performed. The primary outcomes were the changes in OAB symptoms and OAB symptom score (OABSS). Secondary outcomes included adverse events (AEs) and the dropout rate related to AEs.
Results
A total of 6 studies including 7 RCTs involving 1430 patients with mean follow-up of 23.43 weeks were included. All ADs improved OAB symptoms. Regarding efficacy, these drugs had similar efficacy in voids, urgency episodes, urgency incontinence episodes, incontinence episodes and OABSS. However, imidafenacin performed better in the reduction of nocturia episodes (MD = –0.24, 95% CI –0.44 to –0.04, P = 0.02). Moreover, imidafenacin was associated with a statistically lower dry mouth rate (RR = 0.87, 95% CI 0.75–1.00, P = 0.04), lower constipation rate (RR = 0.68, 95% CI 0.50–0.93, P = 0.01) and lower AE-related withdrawal rate (RR = 0.51, 95% CI 0.29–0.89, P = 0.02). There was no significant difference in terms of other complications.
Conclusions
In conclusion, imidafenacin was comparable to other ADs in the treatment of OAB. Moreover, imidafenacin presented a lower dry mouth rate, lower constipation rate and higher adherence and persistence.










Similar content being viewed by others
Abbreviations
- OAB:
-
overactive bladder syndrome
- OABSS:
-
Overactive bladder symptom score
- RCT:
-
randomized controlled trials
- AE:
-
adverse event
- AD:
-
anticholinergic drug
- PVR:
-
postvoid residual volume
- UTI:
-
urinary tract infection
- ROB:
-
risk of bias
- MD:
-
mean difference
- RR:
-
relative risk
- CI:
-
confidential interval
- QOL:
-
quality of life
References
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, et al. The standardization of terminology of lower urinary tract function: report from the standardization sub-committee of the International Continence Society. Am J Obstet Gynecol. 2002;187(1):116–26. https://doi.org/10.1067/mob.2002.125704.
Drake MJ. Do we need a new definition of the overactive bladder syndrome? ICI-RS 2013. Neurourol Urodyn. 2014;33(5):622–4. https://doi.org/10.1002/nau.22609.
Irwin DE, Milsom I, Hunskaar S, Reilly K, Kopp Z, Herschorn S, et al. Population-based survey of urinary incontinence, overactive bladder, and other lower urinary tract symptoms in five countries: results of the EPIC study. Eur Urol. 2006;50(6):1306–14; discussion 1314-1305. https://doi.org/10.1016/j.eururo.2006.09.019.
Stewart WF, Van Rooyen JB, Cundiff GW, Abrams P, Herzog AR, Corey R, et al. Prevalence and burden of overactive bladder in the United States. World J Urol. 2003;20(6):327–36. https://doi.org/10.1007/s00345-002-0301-4.
Milsom I, Kaplan SA, Coyne KS, Sexton CC, Kopp ZS. Effect of bothersome overactive bladder symptoms on health-related quality of life, anxiety, depression, and treatment seeking in the United States: results from EpiLUTS. Urology. 2012;80(1):90–6. https://doi.org/10.1016/j.urology.2012.04.004.
Andersson K-E. Antimuscarinics for treatment of overactive bladder. Lancet Neurol. 2004;3(1):46–53. https://doi.org/10.1016/s1474-4422(03)00622-7.
Chapple CR, Nazir J, Hakimi Z, Bowditch S, Fatoye F, Guelfucci F, et al. Persistence and adherence with mirabegron versus antimuscarinic agents in patients with overactive bladder: a retrospective observational study in UK clinical practice. Eur Urol. 2017;72(3):389–99. https://doi.org/10.1016/j.eururo.2017.01.037.
Akino H, Namiki M, Suzuki K, Fuse H, Kitagawa Y, Miyazawa K, et al. Factors influencing patient satisfaction with antimuscarinic treatment of overactive bladder syndrome: results of a real-life clinical study. Int J Urol: Off J Japan Urol Assoc. 2014;21(4):389–94. https://doi.org/10.1111/iju.12298.
Kobayashi F, Yageta Y, Segawa M, Matsuzawa S. Effects of imidafenacin (KRP-197/ONO-8025), a new anti-cholinergic agent, on muscarinic acetylcholine receptors. High affinities for M3 and M1 receptor subtypes and selectivity for urinary bladder over salivary gland. Arzneimittel-Forschung. 2007;57(2):92–100. https://doi.org/10.1055/s-0031-1296589.
Kobayashi F, Yageta Y, Yamazaki T, Wakabayashi E, Inoue M, Segawa M, et al. Pharmacological effects of imidafenacin (KRP-197/ONO-8025), a new bladder selective anti-cholinergic agent, in rats. Comparison of effects on urinary bladder capacity and contraction, salivary secretion and performance in the Morris water maze task. Arzneimittel-Forschung. 2007;57(3):147–54. https://doi.org/10.1055/s-0031-1296598.
Homma Y, Yamaguchi T, Yamaguchi O. A randomized, double-blind, placebo-controlled phase II dose-finding study of the novel anti-muscarinic agent imidafenacin in Japanese patients with overactive bladder. Int J Urol: Off J Japan Urol Assoc. 2008;15(9):809–15. https://doi.org/10.1111/j.1442-2042.2008.02104.x.
Huang W, Zong H, Zhou X, Zhang Y. Efficacy and safety of imidafenacin for overactive bladder in adult: a systematic review and meta-analysis. Int Urol Nephrol. 2015;47(3):457–64. https://doi.org/10.1007/s11255-015-0916-1.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ (Clinical research ed). 2009;339:b2535. https://doi.org/10.1136/bmj.b2535.
Homma Y, Yoshida M, Seki N, Yokoyama O, Kakizaki H, Gotoh M, et al. Symptom assessment tool for overactive bladder syndrome—overactive bladder symptom score. Urology. 2006;68(2):318–23. https://doi.org/10.1016/j.urology.2006.02.042.
Homma Y, Yamaguchi O, Imidafenacin Study G. A randomized, double-blind, placebo- and propiverine-controlled trial of the novel antimuscarinic agent imidafenacin in Japanese patients with overactive bladder. Int J Urol: Off J Japan Urol Assoc. 2009;16(5):499–506. https://doi.org/10.1111/j.1442-2042.2009.02286.x.
Yokoyama T, Koide T, Hara R, Fukumoto K, Miyaji Y, Nagai A. Long-term safety and efficacy of two different antimuscarinics, imidafenacin and solifenacin, for treatment of overactive bladder: a prospective randomized controlled study. Urol Int. 2013;90(2):161–7. https://doi.org/10.1159/000345055.
Zaitsu M, Mikami K, Ishida N, Takeuchi T. Comparative evaluation of the safety and efficacy of long-term use of imidafenacin and solifenacin in patients with overactive bladder: a prospective, open, randomized, parallel-group trial (the LIST study). Adv Urol. 2011;2011:854697. https://doi.org/10.1155/2011/854697.
Park C, Park J, Choo MS, Kim JC, Lee JG, Lee JZ, et al. A randomized, prospective double-blind, propiverine-controlled trial of imidafenacin in patients with overactive bladder. Int J Clin Pract. 2014;68(2):188–96. https://doi.org/10.1111/ijcp.12255.
Lee KS, Park B, Kim JH, Kim HG, Seo JT, Lee JG, et al. A randomized, double-blind, parallel design, multi-institutional, non-inferiority phase IV trial of imidafenacin versus fesoterodine for overactive bladder. Int J Clin Pract. 2013;67(12):1317–26. https://doi.org/10.1111/ijcp.12272.
Pushkar DY, Kasyan GR, Kolontarev KB, Sharvadze GG, Mukhametshina EI. Randomized, open-label, tolterodine-controlled, comparative study of the novel antimuscarinic agent imidafenacin in patients with overactive bladder. Neurourol Urodyn. 2019. https://doi.org/10.1002/nau.23980.
Sussman D, Yehoshua A, Kowalski J, Lee W, Kish J, Chaudhari S, et al. Adherence and persistence of mirabegron and anticholinergic therapies in patients with overactive bladder: a real-world claims data analysis. Int J Clin Pract. 2017;71(3–4). https://doi.org/10.1111/ijcp.12824.
Murakami S, Yoshida M, Iwashita H, Otani M, Miyamae K, Masunaga K, et al. Pharmacological effects of KRP-197 on the human isolated urinary bladder. Urol Int. 2003;71:290–8. https://doi.org/10.1159/000072681.
Yamazaki T, Muraki Y, Anraku T. In vivo bladder selectivity of imidafenacin, a novel antimuscarinic agent, assessed by using an effectiveness index for bladder capacity in rats. Naunyn Schmiedeberg's Arch Pharmacol. 2001;384:319–29. https://doi.org/10.1007/s00210-011-0675-1.
Yamada S, Seki M, Ogoda M, Fukata A, Nakamura M, Ito Y. Selective binding of bladder muscarinic receptors in relation to the pharmacokinetics of a novel antimuscarinic agent, imidafenacin, to treat overactive bladder. J Pharmacol Exp Ther. 2011;336(2):365–71. https://doi.org/10.1124/jpet.110.172288.
Yokoyama O, Homma Y, Yamaguchi O. Imidafenacin, an antimuscarinic agent, improves nocturia and reduces nocturnal urine volume. Urology. 2013;82(3):515–20. https://doi.org/10.1016/j.urology.2013.05.017.
Wada N, Watanabe M, Kita M, Matsumoto S, Osanai H, Yamaguchi S, et al. Effect of imidafenacin on nocturia and sleep disorder in patients with overactive bladder. Urol Int. 2012;89(2):215–21. https://doi.org/10.1159/000339750.
Rosa GM, Bauckneht M, Scala C, Tafi E, Leone Roberti Maggiore U, Ferrero S, et al. Cardiovascular effects of antimuscarinic agents in overactive bladder. Expert Opin Drug Saf. 2013;12(6):815–27. https://doi.org/10.1517/14740338.2013.813016.
Yoshida M, Kato D, Nishimura T, Van Schyndle J, Uno S, Kimura T. Anticholinergic burden in the Japanese elderly population: use of antimuscarinic medications for overactive bladder patients. Int J Urol: Off J Japan Urol Assoc. 2018;25(10):855–62. https://doi.org/10.1111/iju.13758.
Lundgren R. Nocturia: a new perspective on an old symptom. Scand J Urol Nephrol. 2004;38(2):112–6. https://doi.org/10.1080/00365590310020033.
Asplund R. Mortality in the elderly in relation to nocturnal micturition. BJU Int. 1999;84(3):297–301.
Stewart RB, Moore MT, May FE, Marks RG, Hale WE. Nocturia: a risk factor for falls in the elderly. J Am Geriatr Soc. 1992;40(12):1217–20.
Brubaker L, FitzGerald MP. Nocturnal polyuria and nocturia relief in patients treated with solifenacin for overactive bladder symptoms. Int Urogynecol J Pelvic Floor Dysfunct. 2007;18(7):737–41. https://doi.org/10.1007/s00192-006-0239-y.
Funding
This study was funded by the National Natural Science Fund of China(grant nos. 81770673) and 1.3.5 project for disciplines of excellence, West China Hospital, Sichuan University (grant nos.ZY2017310).
Author information
Authors and Affiliations
Contributions
J-P Wu, L Peng and X Zeng: data collection, data analysis, manuscript writing; H Shen, H Li: data collection and management; J-P Wu and D-Y Luo: protocol/project development.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests that might have influenced the performance or presentation of the work described in this manuscript.
Informed content
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wu, JP., Peng, L., Zeng, X. et al. Is imidafenacin an alternative to current antimuscarinic drugs for patients with overactive bladder syndrome?. Int Urogynecol J 32, 1117–1127 (2021). https://doi.org/10.1007/s00192-020-04329-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04329-x