Abstract
Introduction and hypothesis
We evaluated the effects of pulsed magnetic stimulation (PMS) on overall and different aspects of quality of life (QoL) in female patients with stress urinary incontinence (SUI).
Methods
This study involved 120 female SUI subjects aged ≥21 years old randomized to either active or sham PMS. Treatment involved two PMS sessions per week for 2 months (16 sessions). After 2 months, subjects could opt for 16 additional sessions regardless of initial randomization. The primary response criterion was a 7-point reduction in the total score of the International Consultation on Incontinence Questionnaire-Lower Urinary Tract Symptoms Quality of Life (ICIQ-LUTSqol) questionnaire. Follow-ups were conducted at months 1, 2, 5, 8, and 14.
Results
At 2 months, 35 out of 60 (58%) subjects in the active arm and 21 out of 60 (21%) in the sham arm were treatment responders (≥7-point reduction) (p = 0.006). There was a significant difference in changes in the mean ± SE ICIQ-LUTSqol total score between the active and sham arms (Mdiff = −8.74 ± 1.25 vs −4.10 ± 1.08, p = 0.006). At 1-year post-treatment, regardless of number of PMS sessions (16 or 32 sessions), subjects who received active PMS (63 out of 94, 67%) were more likely to be treatment responders compared with subjects who did not receive any active PMS (3 out of 12, 25%; p < 0.001). The impact of PMS treatment was the greatest on the “physical activities” domain.
Conclusions
PMS resulted in significant short- and long-term improvements in overall and various physical, social, and psychological aspects of QoL.

Similar content being viewed by others
References
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn. 2010;29(1):4–20. doi:10.1002/nau.20798.
Chong EC, Khan AA, Anger JT. The financial burden of stress urinary incontinence among women in the United States. Curr Urol Rep. 2011;12(5):358–62. doi:10.1007/s11934-011-0209-x.
Lim R, Liong ML, Leong WS, Khan NAK, Yuen KH. Effect of stress urinary incontinence on sexual function of couples and quality of life of the patients. J Urol. 2016;196(1):153–8. doi:10.1016/j.juro.2016.01.090.
Abrams P, Smith AP, Cotterill N. The impact of urinary incontinence on health-related quality of life (HRQoL) in a real-world population of women aged 45–60 years: results from a survey in France, Germany, the UK and the USA. BJU Int. 2015;115(1):143–52. doi:10.1111/bju.12852.
Fatton B, de Tayrac R, Costa P. Stress urinary incontinence and LUTS in women—effects on sexual function. Nat Rev Urol. 2014;11(10):565–78. doi:10.1038/nrurol.2014.205.
Tennstedt SL, Fitzgerald MP, Nager CW, Xu Y, Zimmern P, Kraus S, et al. Quality of life in women with stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2007;18(5):543–9. doi:10.1007/s00192-006-0188-5.
Oh S-J, Ku JH. Impact of stress urinary incontinence and overactive bladder on micturition patterns and health-related quality of life. Int Urogynecol J. 2007;18(1):65–71. doi:10.1007/s00192-006-0112-z.
Goldberg RP, Sand PK. Electromagnetic pelvic floor stimulation for urinary incontinence and bladder disease. Int Urogynecol J Pelvic Floor Dysfunct. 2001;12(6):401–4.
Galloway NT, El-Galley RE, Sand PK, Appell RA, Russell HW, Carlan SJ. Extracorporeal magnetic innervation therapy for stress urinary incontinence. Urology. 1999;53(6):1108–11.
Funk RH, Knels L, Augstein A, Marquetant R, Dertinger HF. Potent stimulation of blood flow in fingers of volunteers after local short-term treatment with low-frequency magnetic fields from a novel device. Evid Based Complement Alternat Med. 2014;2014:543564. doi:10.1155/2014/543564.
Quek P. A critical review on magnetic stimulation: what is its role in the management of pelvic floor disorders? Curr Opin Urol. 2005;15(4):231–5.
Lim R, Liong ML, Leong WS, Khan NAK, Yuen KH. Randomized controlled trial of pulsed magnetic stimulation for stress urinary incontinence: 1-year results. J Urol. 2017;197(5):1302–8. doi:10.1016/j.juro.2016.11.091.
Burkhard FC, Lucas MG, Berghmans LC, et al. EAU guidelines on urinary incontinence. 2017. https://uroweb.org/wp-content/uploads/EAU-Guidelines-Urinary-Incontinence-2016.pdf.
Abrams P, Cardozo L, Wein A, Wagg A (2017) Incontinence: 6th International Consultation on Incontinence, Tokyo, September 2016. 6 ed. Bristol: ICUD.
Lim R, Lee SWH, Tan PY, Liong ML, Yuen KH. Efficacy of electromagnetic therapy for urinary incontinence: a systematic review. Neurourol Urodyn. 2015;34(8):713–22. doi:10.1002/nau.22672.
Fujishiro T, Enomoto H, Ugawa Y, Takahashi S, Ueno S, Kitamura T. Magnetic stimulation of the sacral roots for the treatment of stress incontinence: an investigational study and placebo controlled trial. J Urol. 2000;164(4):1277–9.
Manganotti P, Zaina F, Vedovi E, Pistoia L, Rubilotta E, D'Amico A, et al. Repetitive magnetic stimulation of the sacral roots for the treatment of stress incontinence: a brief report. Eura Medicophys. 2007;43(3):339–44.
Gilling PJ, Wilson LC, Westenberg AM, McAllister WJ, Kennett KM, Frampton CM, et al. A double-blind randomized controlled trial of electromagnetic stimulation of the pelvic floor vs sham therapy in the treatment of women with stress urinary incontinence. BJU Int. 2009;103(10):1386–90. doi:10.1111/j.1464-410X.2008.08329.x.
Sedrakyan A, Campbell B, Merino JG, Kuntz R, Hirst A, McCulloch P. IDEAL-D: a rational framework for evaluating and regulating the use of medical devices. BMJ. 2016;353:i2372. doi:10.1136/bmj.i2372.
Lim R, Liong ML, Leong WS, Khan NAK, Yuen KH. Magnetic stimulation for stress urinary incontinence: study protocol for a randomized controlled trial. Trials. 2015;16:279. doi:10.1186/s13063-015-0803-1.
Nystrom E, Sjostrom M, Stenlund H, Samuelsson E. ICIQ symptom and quality of life instruments measure clinically relevant improvements in women with stress urinary incontinence. Neurourol Urodyn. 2015;34(8):747–51. doi:10.1002/nau.22657.
Avery K, Donovan J, Peters TJ, Shaw C, Gotoh M, Abrams P. ICIQ: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourol Urodyn. 2004;23(4):322–30. doi:10.1002/nau.20041.
Coyne K, Kelleher C. Patient reported outcomes: the ICIQ and the state of the art. Neurourol Urodyn. 2010;29(4):645–51. doi:10.1002/nau.20911.
Lim R, Liong ML, Lau YK, Yuen KH. Validity, reliability, and responsiveness of the ICIQ-UI SF and ICIQ-LUTSqol in the Malaysian population. Neurourol Urodyn. 2017;36(2):438–42. doi:10.1002/nau.22950.
Ayeleke RO, Hay-Smith EJ, Omar MI. Pelvic floor muscle training added to another active treatment versus the same active treatment alone for urinary incontinence in women. Cochrane Data Syst Rev. 2013;11:CD010551. doi:10.1002/14651858.CD010551.pub2.
Dumoulin C, Hay-Smith J, Habée-Séguin GM, Mercier J. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women: a short version Cochrane systematic review with meta-analysis. Neurourol Urodyn. 2015;34(4):300–8. doi:10.1002/nau.22700.
Lagro-Janssen T, Smits A, Van Weel C. Urinary incontinence in women and the effects on their lives. Scand J Prim Health Care. 1992;10(3):211–6.
World Health Organisation. Global recommendations on physical activity for health. Geneva: World Health Organisation; 2010.
Nygaard I, Girts T, Fultz NH, Kinchen K, Pohl G, Sternfeld B. Is urinary incontinence a barrier to exercise in women? Obstet Gynecol. 2005;106(2):307–14. doi:10.1097/01.AOG.0000168455.39156.0f.
Rapp MA, Gerstorf D, Helmchen H, Smith J (2008) Depression predicts mortality in the young old, but not in the oldest old: results from the Berlin Aging Study. Am J Geriatr Psychiatry 16(10):844–52. doi: 10.1097/JGP.0b013e31818254eb.
Coyne KS, Kvasz M, Ireland AM, Milsom I, Kopp ZS, Chapple CR. Urinary incontinence and its relationship to mental health and health-related quality of life in men and women in Sweden, the United Kingdom, and the United States. Eur Urol. 2012;61(1):88–95. doi:10.1016/j.eururo.2011.07.049.
McCulloch P, Altman DG, Campbell WB, Flum DR, Glasziou P, Marshall JC, et al. No surgical innovation without evaluation: the IDEAL recommendations. Lancet. 2009;374(9695):1105–12. doi:10.1016/S0140-6736(09)61116-8.
Pennell CP, Hirst A, Sedrakyan A, McCulloch PG. Adapting the IDEAL framework and recommendations for medical device evaluation: a modified Delphi survey. Int J Surg. 2016;28:141–8. doi:10.1016/j.ijsu.2016.01.082.
Krueger C, Tian L. A comparison of the general linear mixed model and repeated measures ANOVA using a dataset with multiple missing data points. Biol Res Nursing. 2004;6(2):151–7. doi:10.1177/1099800404267682.
Arnau J, Balluerka N, Bono R, Gorostiaga A. General linear mixed model for analysing longitudinal data in developmental research. Percept Mot Skills. 2010;110(2):547–66. doi:10.2466/pms.110.2.547-566.
Acknowledgements
We would like to thank all the study participants.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The study was funded by QRS International, Liechtenstein.
Ethics committee
The study was approved by the Joint Ethics Committee of the School of Pharmaceutical Sciences, USM-HLWE on Clinical Studies (USM-HLWE/IEC/2013[0006]).
Conflicts of interest
Renly Lim was a PhD student who received a research allowance from QRS International (sponsor of the clinical trial) during her PhD candidature. All other authors declare that they have no competing interests.
Electronic supplementary material
Supplement 1
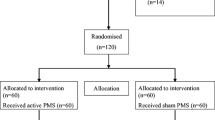
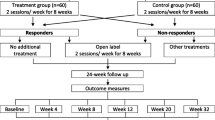
First phase: 120 subjects were randomized to either active (n = 60) or sham (n = 60) PMS for 2 months. Second phase: after 2 months, subjects could opt for 16 additional active PMS sessions (open-label phase). Third phase: subjects returned for follow-up at months 5, 8, and 14. (GIF 12 kb)
Rights and permissions
About this article
Cite this article
Lim, R., Liong, M.L., Leong, W.S. et al. Effect of pulsed magnetic stimulation on quality of life of female patients with stress urinary incontinence: an IDEAL-D stage 2b study. Int Urogynecol J 29, 547–554 (2018). https://doi.org/10.1007/s00192-017-3439-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-017-3439-8