Abstract
Introduction and hypothesis
Patients with genital prolapse and occult stress urinary incontinence (OSUI) are typically treated with prolapse surgery and anti-incontinence surgery based on either a one-step approach or a two-step approach. The aim of our study was to determine whether anti-incontinence surgery is necessary based on the occurrence of OSUI in a study cohort with a long follow-up period.
Methods
Prolapse surgery was performed using a vaginal approach. Preoperatively, a stress test, a pad test and an assessment of the urodynamics were performed with and without prolapse reduction. Over a follow-up period of 2–8 years, the patients with preoperative evidence of OSUI underwent urogynaecological examinations, stress tests and pad tests.
Results
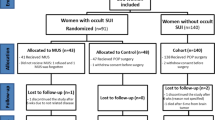
Of 113 patients with preoperative evidence of OSUI, 57 (50.4 %) were followed up for an average of 5.7 years (range 2–8) after prolapse surgery. Of 57 patients, 16 (28.1 %) had objective and/or subjective stress urinary incontinence (SUI) during the follow-up period, but only 3 patients (5.3 %) required subsequent tension-free vaginal tape (TVT) surgery. In 17 of 57 patients (29.8 %), prolapse recurred.
Conclusions
Despite the preoperative evidence of OSUI, the manifestation of SUI rarely occurs, with 28.1 % of patients experiencing SUI over long-term follow-up after vaginal prolapse surgery. Anti-incontinence surgery was necessary in only three cases (5.3 %). These results indicate that with the one-step approach, 54 of 57 patients (94.7 %) would have received prophylactic anti-incontinence surgery unnecessarily. In conclusion, we recommend the two-step approach in the management of vaginal prolapse surgery in patients with OSUI.

Similar content being viewed by others
References
Long CY, Hsu SC, Wu TP, Sun DJ, Su JH, Tsai EM (2004) Urodynamic comparison of continent and incontinent women with severe uterovaginal prolapse. J Reprod Med 49(1):33–37
Ghoniem GM, Walters F, Lewis V (1994) The value of the vaginal pack test in large cystoceles. J Urol 152(3):931–934
Hextall A, Boos K, Cardozo L, Toozs-Hobson P, Anders K, Khullar V (1998) Videocystourethrography with a ring pessary in situ. A clinically useful preoperative investigation for continent women with urogenital prolapse? Int Urogynecol J Pelvic Floor Dysfunct 9(4):205–209
Romanzi LJ (2002) Management of the urethral outlet in patients with severe prolapse. Curr Opin Urol 12(4):339–344
Deszensus der Frau - Diagnostik und Therapie AWMF 015/006. Deutsche Gesellschaft für Gynäkologie und Geburtshilfe ev Leitlinien Stand August 2008
Bump RC, Mattiasson A, Bø K et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175(1):10–17
Karram M (1993) Urodynamics; cystometry, voiding studies, urethral pressure profilometry. In: Walters M, Karram M (eds) Clinical urogynecology. Mosby, St. Louis, pp 62–101
Heesakkers JP, Vriesema JL (2005) The role of urodynamics in the treatment of lower urinary tract symptoms in women. Curr Opin Urol 15(4):215–221
Liang CC, Chang YL, Chang SD, Lo TS, Soong YK (2004) Pessary test to predict postoperative urinary incontinence in women undergoing hysterectomy for prolapse. Obstet Gynecol 104(4):795–800
Visco A, Brubaker L, Nygaard I et al (2008) The role of preoperative urodynamic testing in stress-continent women undergoing sacrocolpopexy: the Colpopexy and Urinary Reduction Efforts (CARE) randomized surgical trial. Int Urogynecol J Pelvic Floor Dysfunct 19(5):607–614
Lowder J, Burrows L, Howden N, Weber A (2006) Prophylactic antibiotics after urodynamics in women: a decision analysis. Int Urogynecol J Pelvic Floor Dysfunct 18(2):159–164
Latthe PM, Foon R, Toozs-Hobson P (2008) Prophylactic antibiotics in urodynamics: a systematic review of effectiveness and safety. Neurourol Urodyn 27(3):167–173
Roovers JP, Oelke M (2007) Clinical relevance of urodynamic investigation tests prior to surgical correction of genital prolapse: a literature review. Int Urogynecol J Pelvic Floor Dysfunct 18(4):455–460
Klutke JJ, Ramos S (2000) Urodynamic outcome after surgery for severe prolapse and potential stress incontinence. Am J Obstet Gynecol 182(6):1378–1381
Jundt K, Wagner S, von Bodungen V, Friese K, Peschers UM (2010) Occult incontinence in women with pelvic organ prolapse—does it matter? Eur J Med Res 15:112–116
Groutz A, Gold R, Pauzner D, Lessing JB, Gordon D (2004) Tension-free vaginal tape (TVT) for the treatment of occult stress urinary incontinence in women undergoing prolapse repair: a prospective study of 100 consecutive cases. Neurourol Urodyn 23:632–635
de Tayrac R, Gervaise A, Chauveaud-Lambling A, Fernandez H (2004) Combined genital prolapse repair reinforced with a polypropylene mesh and tension-free vaginal tape in women with genital prolapse and stress urinary incontinence: a retrospective case-control study with short-term follow-up. Acta Obstet Gynecol Scand 83:950–954
Schierlitz L, Dwyer P, Rosamilia A et al (2010) A prospective randomised controlled trial comparing vaginal prolapse repair with and without tensionfree vaginal tape (TVT) in women with severe genital prolapse and occult stress urinary incontinence: long term follow up. Int Urogynecol J 21(Suppl 1):S1–S428. doi:10.1007/s00192-010-1192-3
Bergman A, Elia G (1995) Three surgical procedures for genuine stress-incontinence: five-year follow-up of a prospective randomized study. Am J Obstet Gynecol 173:66–71
Glazener C, Cooper K (2001) Anterior vaginal repair for urinary incontinence in women. Cochrane Database Syst Rev 1:CD001755. doi:10.1002/14651858
Whiteside JL, Weber AM, Meyn LA, Walters MD (2004) Risk factors for prolapse recurrence after vaginal repair. Am J Obstet Gynecol 191(5):1533–1538
Chaikin DC, Groutz A, Blaivas JG (2000) Predicting the need for anti-incontinence surgery in continent women undergoing repair of severe urogenital prolapse. J Urol 163:531–534
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ennemoser, S., Schönfeld, M., von Bodungen, V. et al. Clinical relevance of occult stress urinary incontinence (OSUI) following vaginal prolapse surgery: long-term follow-up. Int Urogynecol J 23, 851–855 (2012). https://doi.org/10.1007/s00192-012-1765-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1765-4