Abstract
Introduction and hypothesis
Pelvic floor muscle training (PFMT) is a treatment for stress urinary incontinence (SUI) that can be done individually or in a group. The aim of this study was to compare these two types of treatment.
Methods
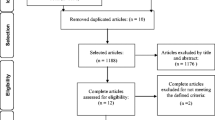
Sixty women 30 to 75 years old with SUI were randomly assigned to participate in the two groups. They were evaluated before and after the treatment with the Oxford grading system, pad test, voiding diary, and the King’s Health Questionnaire.
Results
Both groups experienced significant reductions in urinary leakage as measured by the pad test and bladder diary. A negative pad test was observed in about 50% of patients in both groups. There were statistically significant improvements in both muscle strength and quality of life. When the groups were compared, there were no differences in the results between them.
Conclusions
Individual treatment and group PFMT appear to be equally effective for improving SUI.
Similar content being viewed by others
References
Hunskaar S, Burgio K, Diokno A, Herzog AR, Hjalmas K, Lapitan MC (2003) Epidemiology and natural history of urinary incontinence in women. Urology 62:16–23
Kegel AH (1948) Progressive resistance exercise in the functional restoration of the perineal muscle. Am J Obstet Gynecol 56:238–248
Thakar R, Stanton S (2000) Management of urinary incontinence in women. Br Med J 321:1326–1331
Freeman RM (2004) The role of pelvic floor muscle training in urinary incontinence. Br J Obstet Gynaecol 111:37–40
Castro RA, Arruda RM, Zanetti MR, Santos PD, Sartori MG, Girão MJ (2008) Single-blind, randomized, controlled trial of pelvic floor muscle training, electrical stimulation, vaginal cones, and no active treatment in the management of stress urinary incontinence. Clinics 63:465–472
Hay-Smith E, Bø K, Berghmans L, Hendriks H, deBie R, van Waalwijk van Doorn E et al (2007) Pelvic floor muscle training for urinary incontinence in women. Cochrane Database Syst Rev, CD 001407
Bø K (2004) Pelvic floor muscle training is effective in treatment of female stress urinary incontinence, but how does it work? Int Urogynecol J 15:76–84
Bø K, Talseth T, Holme I (1999) Single blind, randomized controlled trial of pelvic floor exercises, electrical stimulation, vaginal cones and no treatment in management of genuine stress incontinence in women. Br Med J 318:487–493
Bø K, Sherburn M (2005) Evaluation of female pelvic floor muscle function and strength. Phys Ther 85:269–282
Laycock J, Jerwood D (2001) Pelvic floor muscle assessment: the perfect scheme. Physiotherapy 87:631–642
Lose G, Rosenkilde P, Gammelgaard J, Schroeder T (1988) Pad-weighing test performed with standardized bladder volume. Urology 32:78–80
Kelleher C (2000) Quality of life and urinary incontinence. Baillieres Best Pract Res Clin Obst Gynaecol 14:363–379
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, Kerrebroeck P, Victor A, Wein A (2002) The standardisation of terminology of lower urinary tract function: report from the Standardisation Subcommittee of the International Continence Society. Am J Obstet Gynecol 187:116–126
Konstantinidou E, Apostolidis A, Kondelidis N, Tsimtsiou Z, Hatzichristou D, Ioannides E (2007) Short-term efficacy of group pelvic floor training under intensive supervision versus unsupervised home training for female stress urinary incontinence: a randomized pilot study. Neurourol Urodyn 26:486–491
Lagro-Janssen TL, Debruyne FM, Smits AJ, van Weel C (1991) Controlled trial of pelvic floor exercises in the treatment of urinary stress incontinence in general practice. Br J Gen Pract 41:445–449
Janssen CC, Lagro-Janssen AL, Felling AJ (2001) The effects of physiotherapy for female urinary incontinence: individual compared with group treatment. BJU Int 87:201–206
Bø K, Hagen RH, Kvarstein B, Jørgensen J, Larsen S (1990) Pelvic floor muscle exercises for the treatment of female stress urinary incontinence. III: Effects of two different degrees of pelvic floor muscle exercise. Neurourol Urodyn 9:489–502
Jòzwik M (1998) The physiological basis of pelvic floor exercises in the treatment of stress urinary incontinence. Br J Obstet Gynaecol 105:1046–1051
Balmforth JR, Cardozo LD (2003) Trends toward less invasive treatment of female stress urinary incontinence. Urology 62:52–60
Thompson JA, O’Sullivan PB, Briffa NK, Neumann P (2006) Assessment of voluntary pelvic floor muscle contraction in continent and incontinent women using transperineal ultrasound, manual muscle testing and vaginal squeeze pressure measurements. Int Urogynecol J 17(6):624–630
Morin M, Dumoulin C, Bourbonnais D, Gravel D, Lemieux MC (2004) Pelvic floor maximal strength using vaginal digital assessment compared to dynamometric measurements. Neurourol Urodyn 23(4):336–341
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Oliveira Camargo, F., Rodrigues, A.M., Arruda, R.M. et al. Pelvic floor muscle training in female stress urinary incontinence: comparison between group training and individual treatment using PERFECT assessment scheme. Int Urogynecol J 20, 1455–1462 (2009). https://doi.org/10.1007/s00192-009-0971-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-009-0971-1