Abstract
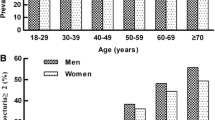
To determine the prevalence of nocturia and associated bother among patients presenting to a tertiary urogynecology clinic and to describe patient characteristics related to nocturic frequency and associated bother. Chart review of sequential new patients presenting to our clinic between June 2004 and May 2005. We recorded patients’ response to a question about their frequency of nocturia, the level of associated bother, demographic data, history of chronic medical illness and clinical urogynecologic diagnosis. Seven hundred sixty patients were of mean age 56 (19–95) years. Eighty-seven percent of patients voided at least once nightly, and 60% usually voided at least twice nightly. Forty one percent of patients reported bother ≥5/10 from nocturia. High bother rating was associated with increasing number of nocturic episodes (p < 0.0005) and mixed incontinence (p = 0.012). Nocturia is common and bothersome to women presenting for urogynecologic care. Concomitant mixed incontinence significantly increases bother arising from nocturia.

Similar content being viewed by others
References
Van Kerrebroeck P, Abrams P, Chaikin D et al (2002) The standardization of terminology in nocturia: report from the Standardization Subcommittee of the International Continence Society. BJU Int 90(Suppl 3):11–15
Swithinbank LV, Donovan JL, du Heaume JC et al (1999) Urinary symptoms and incontinence in women: relationships between occurrence, age, and perceived impact. Br J Gen Pract 49(448):897–900
Middelkoop HA, Smilde-van den Doel DA, Neven AK et al (1996) Subjective sleep characteristics of 1,485 males and females aged 50–93: effects of sex and age, and factors related to self-evaluated quality of sleep. J Gerontol Ser A Biol Sci Med Sci 51(3):M108–M115
Asplund R, Aberg H (1996) Nocturnal micturition, sleep and well-being in women of ages 40–64 years. Maturitas 24(1–2):73–81
Stewart RB, Moore MT, May FE et al (1992) Nocturia: a risk factor for falls in the elderly. J Am Geriatr Soc 40(12):1217–1220
Fiske J, Scarpero HM, Xue X, Nitti VW (2004) Degree of bother caused by nocturia in women. Neurourol Urodyn 23(2):130–133
Bing MH, Mollar LA, Jennum P et al (2006) Prevalence and bother of nocturia, and the causes of sleep interruption in a Danish population of men and women aged 60–80 years. BJU Int 98(3):599–604
Gourova LW, van de Beek C, Spigt MG et al (2006) Predictive factors for nocturia in elderly men: a cross-sectional study in 21 general practices. BJU Int 97(3):528–532
Brieger GM, Yip SK, Hin LY et al (1996) The prevalence of urinary dysfunction in Hong Kong Chinese women. Obstet Gynecol 88(6):1041–1044
Fitzgerald MP, Stablein U, Brubaker L (2002) Urinary habits among asymptomatic women. Am J Obstet Gynecol 187(5):1384–1388
Rembratt A, Norgaard JP, Andersson KE (2003) Nocturia and associated morbidity in a community-dwelling elderly population. BJU Int 92(7):726–730
Asplund R (2002) Nocturia in relation to sleep, somatic disease and medical treatment in the elderly. BJU Int 90:533–536
Coyne KS, Payne C, Bhattacharyya SK et al (2004) The impact of urinary urgency and frequency on health-related quality of life in overactive bladder: results from a national community survey. Value Health 7(4):455–463
Federal Interagency Forum on Aging Related Statistics, in Older Americans (2000) Key indicators of well-being. US Government
US Department of Commerce (1998) Statistical abstract of the United States: the national data book
Bing MH, Mollar LA, Jennum P et al (2006) Validity and reliability of a questionnaire for evaluating nocturia, nocturnal enuresis and sleep interruptions in an elderly population. Eur Urol 49(4):710–719
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lowenstein, L., Brubaker, L., Kenton, K. et al. Prevalence and impact of nocturia in a urogynecologic population. Int Urogynecol J 18, 1049–1052 (2007). https://doi.org/10.1007/s00192-006-0289-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-006-0289-1