Abstract
Purpose
This cadaveric study aimed to elucidate PCL morphology by observing the anatomical relationship with other structures and the fibre layers of the PCL in cross section for remnant preserving PCL reconstruction.
Methods
Seventeen fresh-frozen cadaveric knees were studied, using the clock-face method to analyse the anatomical relationship between the PCL and Humphrey’s ligament. The width and thickness of the PCL, Humphrey’s and Wrisberg’s ligaments were measured. The PCL was cut sharply perpendicular to the tibia shaft, and the fibre layers were observed in cross section.
Results
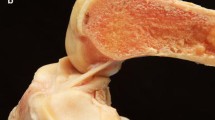
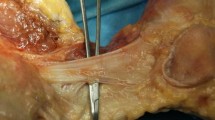
The PCL was located between 12 and 4 o’clock in the right knee (8 and 12 o’clock in the left), while Humphrey’s ligament was located between 2 and 4 o’clock in the right knee (8 and 10 o’clock in the left). Humphrey’s ligament at femoral insertion, midsubstance and lateral meniscus insertion averaged 8.7 ± 2.3, 5.9 ± 2.1 and 6.1 ± 2.0 mm, respectively, while the thickness at each level averaged 2.0 ± 1.2, 1.6 ± 0.6 and 1.9 ± 0.6 mm. The width of the PCL at midsubstance and at medial meniscus level averaged 13.3 ± 2.0 and 11.0 ± 1.6 mm, respectively, while the thickness of the PCL averaged 5.4 ± 0.8 and 5.5 ± 1.4 mm. In cross section, multiple, interconnected layers were observed which could not be divided. The main layers at each level were aligned from the posterolateral to the anteromedial aspect and formed a C-shape at the medial meniscus level.
Conclusion
The PCL at midsubstance is flat. PCL appears as a twisted ribbon composed of many small fibres without clearly separate bundles. When remnant preserving PCL reconstruction is performed, it is necessary to take account of not only PCL morphology but also the ligaments of Humphrey and Wrisberg. These findings may affect the PCL footprint and the graft shape in the future remnant preserving PCL reconstruction.





Similar content being viewed by others
References
Adachi N, Ochi M, Uchio Y, Iwasa J, Ishikawa M, Shinomiya R (2007) Temporal change of joint position sense after posterior cruciate ligament reconstruction using multi-stranded hamstring tendons. Knee Surg Sports Traumatol Arthrosc 15(1):2–8
Ahn JH, Chung YS, Oh I (2003) Arthroscopic posterior cruciate ligament reconstruction using the posterior trans-septal portal. Arthroscopy 19(1):101–107
Ahn JH, Lee SH (2014) Anatomic graft passage in remnant-preserving posterior cruciate ligament reconstruction. Arthrosc Tech 3(5):e579–e582
Ahn JH, Nha KW, Kim YC, Lim HC, Nam HW, Wang JH (2006) Arthroscopic femoral tensioning and posterior cruciate ligament reconstruction in chronic posterior cruciate ligament injury. Arthroscopy 22(3):e341–e344
Amis AA, Bull AM, Gupte CM, Hijazi I, Race A, Robinson JR (2003) Biomechanics of the PCL and related structures: posterolateral, posteromedial and meniscofemoral ligaments. Knee Surg Sports Traumatol Arthrosc 11(5):271–281
Amis AA, Gupte CM, Bull AM, Edwards A (2006) Anatomy of the posterior cruciate ligament and the meniscofemoral ligaments. Knee Surg Sports Traumatol Arthrosc 14(3):257–263
Anderson CJ, Ziegler CG, Wijdicks CA, Engebretsen L, LaPrade RF (2012) Arthroscopically pertinent anatomy of the anterolateral and posteromedial bundles of the posterior cruciate ligament. J Bone Joint Surg Am 94(21):1936–1945
Apple M, Gradinger R (1989) Die Architektur des Kreuzbandaufbaus. Praktische Sport-Traumatologie und Sportmedizin 1:12–16
Chwaluk A, Ciszek B (2009) Anatomy of the posterior cruciate ligament. Folia Morphologica (Warsz) 68(1):8–12
Clancy WG Jr, Shelbourne KD, Zoellner GB, Keene JS, Reider B, Rosenberg TD (1983) Treatment of knee joint instability secondary to rupture of the posterior cruciate ligament. Report of a new procedure. J Bone Joint Surg Am 65(3):310–322
Covey CD, Sapega AA (1993) Injuries of the posterior cruciate ligament. J Bone Joint Surg Am 75(9):1376–1386
Covey DC, Sapega AA, Marshall RC (2004) The effects of varied joint motion and loading conditions on posterior cruciate ligament fiber length behavior. Am J Sports Med 32(8):1866–1872
Covey DC, Sapega AA, Riffenburgh RH (2008) The effects of sequential sectioning of defined posterior cruciate ligament fiber regions on translational knee motion. Am J Sports Med 36(3):480–486
Covey DC, Sapega AA, Sherman GM (1996) Testing for isometry during reconstruction of the posterior cruciate ligament. Anatomic and biomechanical considerations. Am J Sports Med 24(6):740–746
Edwards A, Bull AM, Amis AA (2007) The attachments of the fiber bundles of the posterior cruciate ligament: an anatomic study. Arthroscopy 23(3):284–290
Eguchi A, Adachi N, Nakamae A, Usman MA, Deie M, Ochi M (2014) Proprioceptive function after isolated single-bundle posterior cruciate ligament reconstruction with remnant preservation for chronic posterior cruciate ligament injuries. Orthop Traumatol Surg Res 100(3):303–308
Girgis FG, Marshall JL, Monajem A (1975) The cruciate ligaments of the knee joint. Anatomical, functional and experimental analysis. Clin Orthop Relat Res 106:216–231
Gupte CM, Bull AM, Atkinson HD, Thomas RD, Strachan RK, Amis AA (2006) Arthroscopic appearances of the meniscofemoral ligaments: introducing the “meniscal tug test”. Knee Surg Sports Traumatol Arthrosc 12:1259–1265
Gupte CM, Bull AM, Thomas RD, Amis AA (2003) The meniscofemoral ligaments: secondary restraints to the posterior drawer. Analysis of anteroposterior and rotary laxity in the intact and posterior-cruciate-deficient knee. J Bone Joint Surg Br 85(5):765–773
Jung HJ, Kim JH, Lee HJ, Koo S, Chang SH, Jung YB, Lee SH (2013) The isometry of two different paths for remnant-preserving posterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 5:1029–1035
Keller PM, Shelbourne KD, McCarroll JR, Rettig AC (1993) Nonoperatively treated isolated posterior cruciate ligament injuries. Am J Sports Med 21(1):132–136
Kim SJ, Kim TE, Jo SB, Kung YP (2009) Comparison of the clinical results of three posterior cruciate ligament reconstruction techniques. J Bone Joint Surg Am 91(11):2543–2549
Kim YM, Lee CA, Matava MJ (2011) Clinical results of arthroscopic single-bundle transtibial posterior cruciate ligament reconstruction: a systematic review. Am J Sports Med 39(2):425–434
Kusayama T, Harner CD, Carlin GJ, Xerogeanes JW, Smith BA (1994) Anatomical and biomechanical characteristics of human meniscofemoral ligaments. Knee Surg Sports Traumatol Arthrosc 2(4):234–237
LaPrade CM, Civitarese DM, Rasmussen MT, LaPrade RF (2015) Emerging updates on the posterior cruciate ligament: a review of the current literature. Am J Sports Med 43(12):3077–3092
Lee DW, Jang HW, Lee YS, Oh SJ, Kim JY, Song HE, Kim JG (2014) Clinical, functional, and morphological evaluations of posterior cruciate ligament reconstruction with remnant preservation: minimum 2-year follow-up. Am J Sports Med 42(8):1822–1831
Lopes OV Jr, Ferretti M, Shen W, Ekdahl M, Smolinski P, Fu FH (2008) Topography of the femoral attachment of the posterior cruciate ligament. J Bone Joint Surg Am 90(2):249–255
Makris CA, Georgoulis AD, Papageorgiou CD, Moebius UG, Soucacos PN (2000) Posterior cruciate ligament architecture: evaluation under microsurgical dissection. Arthroscopy 16(6):627–632
Mejia EA, Noyes FR, Grood ES (2002) Posterior cruciate ligament femoral insertion site characteristics. Importance for reconstructive procedures. Am J Sports Med 30(5):643–651
Papannagari R, DeFrate LE, Nha KW, Moses JM, Moussa M, Gill TJ, Li G (2007) Function of posterior cruciate ligament bundles during in vivo knee flexion. Am J Sports Med 35(9):1507–1512
Poynton A, Moran CJ, Moran R, O’Brien M (2011) The meniscofemoral ligaments influence lateral meniscal motion at the human knee joint. Arthroscopy 27(3):365–371
Safran MR, Allen AA, Lephart SM, Borsa PA, Fu FH, Harner CD (1999) Proprioception in the posterior cruciate ligament deficient knee. Knee Surg Sports Traumatol Arthrosc 7(5):310–317
Shelbourne KD, Clark M, Gray T (2013) Minimum 10-year follow-up of patients after an acute, isolated posterior cruciate ligament injury treated nonoperatively. Am J Sports Med 41(7):1526–1533
Shelbourne KD, Jennings RW, Vahey TN (1999) Magnetic resonance imaging of posterior cruciate ligament injuries: assessment of healing. Am J Knee Surg 12(4):209–213
Shelbourne KD, Muthukaruppan Y (2005) Subjective results of nonoperatively treated, acute, isolated posterior cruciate ligament injuries. Arthroscopy 21(4):457–461
Shino K, Horibe S, Nakata K, Maeda A, Hamada M, Nakamura N (1995) Conservative treatment of isolated injuries to the posterior cruciate ligament in athletes. J Bone Joint Surg Br 77(6):895–900
Siebold R, Schuhmacher P, Fernadez F, Smigielski R, Fink C, Brehmer A, Kirsch J (2014) Flat midsubstance of the anterior cruciate ligament with tibial “C”-shaped insertion site. Knee Surg Sports Traumatol Arthrosc 23(11):3136–3142
Smigielski R, Zdanowicz U, Drwiega M, Ciszek B, Ciszkowska-Lyson B, Siebold R (2014) Ribbon like appearance of the midsubstance fibres of the anterior cruciate ligament close to its femoral insertion site: a cadaveric study including 111 knees. Knee Surg Sports Traumatol Arthrosc 23(11):3143–3150
Spiridonov SI, Slinkard NJ, LaPrade RF (2011) Isolated and combined grade-III posterior cruciate ligament tears treated with double-bundle reconstruction with use of endoscopically placed femoral tunnels and grafts: operative technique and clinical outcomes. J Bone Joint Surg Am 93(19):1773–1780
Takahashi M, Matsubara T, Doi M, Suzuki D, Nagano A (2006) Anatomical study of the femoral and tibial insertions of the anterolateral and posteromedial bundles of human posterior cruciate ligament. Knee Surg Sports Traumatol Arthrosc 14(11):1055–1059
Van Dommelen BA, Fowler PJ (1989) Anatomy of the posterior cruciate ligament. A review. Am J Sports Med 17(1):24–29
Acknowledgements
The authors gratefully thank Maciej Śmiarowski (maciej.smiarowski@gmail.com) for taking all photographs.
Author information
Authors and Affiliations
Contributions
TK performed the study design, dissections, measurements, interpretation of the data and drafted the manuscript. RS performed the study concept, dissections, interpretation of the data and critical comments on drafting of the manuscript. YG performed the dissections. UZ interpreted the data. BC instructed the dissections. MO was involved in interpretation of data and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Funding
There was no outside funding or grants received that assisted in this study.
Ethical approval
This study has been performed in accordance with the ethical standards concerning investigations on human cadavers in Poland.
Informed consent
For this type of article informed consent is not required.
Rights and permissions
About this article
Cite this article
Kato, T., Śmigielski, R., Ge, Y. et al. Posterior cruciate ligament is twisted and flat structure: new prospective on anatomical morphology. Knee Surg Sports Traumatol Arthrosc 26, 31–39 (2018). https://doi.org/10.1007/s00167-017-4634-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-017-4634-3