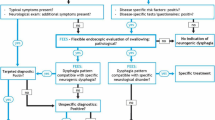
Opinion statement
Substantial ignorance and controversy surround the management of neuromyogenic pharyngeal dysphagia. The major obstacle to confident recommendations is the lack of high-level evidence supporting most available therapies. There is reasonable evidence supporting cricopharyngeal disruption (myotomy or dilatation) in primary restrictive disorders of this region, but low-level evidence supporting myotomy in pure neuromyogenic dysphagia. There is reasonable evidence supporting current dietary recommendations as aspiration-minimization strategies. There is only low-level evidence, albeit consistent, to support swallow-behavior modification therapies. The type of therapy needs to be tailored to the individual and depends upon many variables, including cognitive ability, severity and mechanics of pharyngeal dysfunction, and the perceived safety of continued oral feeding. One or more of these strategies are recommended where appropriate because where the level of evidence is low, it is at least consistently favorable and such therapies have not been proven to be ineffective.
Similar content being viewed by others
References and Recommended Reading
Schmidt J, Holas M, Halvorson K, Reding M: Videofluoroscopic evidence of aspiration predicts pneumonia and death but not dehydration following stroke. Dysphagia 1994, 9:7–11.
Smithard DG, O’Neill PA, Park C, et al.: Complications and outcome after acute stroke: does dysphagia matter? [published erratum appears in Stroke 1998, 29:1480-1481]. Stroke 1996, 27:1200–1204.
Cook IJ, Kahrilas PJ: American Gastroenterological Association technical review on management of oropharyngeal dysphagia. Gastroenterology 1999, 116:455–478.
Anonymous: Diagnosis and treatment of swallowing disorders (dysphagia) in acute-care stroke patients. Summary, Evidence Report/Technology Assessment: Number 8. Rockville, MD: Agency for Health Care Policy and Research; 1999:1–6.
Hamdy S, Aziz Q, Rothwell JC, et al.: Sensorimotor modulation of human cortical swallowing pathways. J Physiol 1998, 506:857–866.
Langmore SE, Skarupski KA, Park PS, Fries BE: Predictors of aspiration pneumonia in nursing home residents. Dysphagia 2002, 17:298–307. Thorough, recent evaluation of a range of risk factors for aspiration.
Mann G, Hankey GJ, Cameron D: Swallowing function after stroke. Prognosis and prognostic factors at six months. Stroke 1999, 30:744–748.
Mann G, Hankey GJ, Cameron D: Swallowing disorders following acute stroke: prevalence and diagnostic accuracy. Cerebrovasc Dis 2000, 10:380–386.
Aviv JE, Sacco RL, Thomson J, et al.: Silent laryngopharyngeal sensory deficits after stroke. Ann Otol Rhinol Laryngol 1997, 106:87–93.
Logemann JA: Role of the modified barium swallow in management of patients with dysphagia. Otolaryngol Head Neck Surg 1997, 116:335–338.
Horner J, Massey EW, Riski JE, et al.: Aspiration following stroke: clinical correlates and outcome. Neurology 1988, 38:1359–1362.
Eisenhuber E, Schima W, Schober E, et al.: Videofluoroscopic assessment of patients with dysphagia: Pharyngeal retention is a predictive factor for aspiration. Am J Roentgenol 2002, 178:393–398.
Croghan JE, Burke EM, Caplan S, Denman S: Pilot study of 12-month outcomes of nursing home patients with aspiration on videofluoroscopy. Dysphagia 1994, 9:141–146.
Johnson ER, McKenzie SW, Sievers A: Aspiration pneumonia in stroke. Arch Phys Med Rehab 1993, 74:973–976.
DePippo KL, Holas MA, Reding MJ, et al.: Dysphagia therapy following stroke: a controlled trial. Neurology 1994, 44:1655–1660.
Daniels SK, Brailey K, Preistly DH, et al.: Aspiration in patients with acute stroke. Arch Phys Med Rehab 1998, 79:14–19.
Doggett DL, Tappe KA, Mitchell MD, et al.: Prevention of pneumonia in elderly stroke patients by systematic diagnosis and treatment of dysphagia: an evidencebased comprehensive analysis of the literature. Dysphagia 2001, 16:279–295. Evidence-based review of swallow therapy.
Cook IJ, Kahrilas PJ: Medical position statement on management of oropharyngeal dysphagia. Gastroenterology 1999, 116:452–454.
Chang MW, Rosendall B, Finlayson BA: Mathematical modelling of normal pharyngeal bolus transport: a preliminary study. J Rehab Res Dev 1998, 35:327–334.
Nicosia MA, Robbins JA: The fluid mechanics of bolus ejection from the oral cavity. J Biomechan 2001, 34:1537–1544. Modelling of bolus rheology explaining the balance between “fluidity” promoting turbulence and penetration risk on one hand versus viscosity demanding greater propulsive forces for clearance on the other.
Groher ME: Bolus management and aspiration pneumonia in patients with pseudobulbar dysphagia. Dysphagia 1987, 1:215–216.
Dennis M: FOOD Trial (Feed or Ordinary Diet): a multicentre trial to evaluate various feeding policies in patients admitted to hospital with a recent stroke [abstract]. Stroke 1998, 29:551.
Bath PM, Bath FJ, Smithard DG: Interventions for dysphagia in acute stroke (Cochrane Review). The Cochrane Library. Oxford:Update Software, 2002:CD000323. Evidence-based review of efficacy studies.
Bartolome G, Neumann S: Swallowing therapy in patients with neurological disorders causing cricopharyngeal dysfunction. Dysphagia 1993, 8:146–149.
Gresham SL: Clinical assessment and management of swallowing difficulties after stroke. Med J Aust 1990, 153:397–399.
Neumann S: Swallowing therapy with neurologic patients: results of direct and indirect therapy methods in 66 patients suffering from neurological disorders. Dysphagia 1993, 8:150–153.
Neumann S, Bartolome G, Buchholz D, Prosiegel M: Swallowing therapy of neurologic patients: correlation of outcome with pretreatment variables and therapeutic methods. Dysphagia 1995, 10:1–5.
Selley WG, Roche MT, Pearce VR, et al.: Dysphagia following strokes: clinical observations of swallowing rehabilitation employing palatal training appliances. Dysphagia 1995, 10:32–35.
Rosenbek JC, Robbins J, Fishback B, Levine RL: Effects of thermal application on dysphagia after stroke. J Speech Hear Res 1991, 34:1257–1268.
Kasprisin AT, Clumeck H, Nino-Murcia M: The efficacy of rehabilitative management of dysphagia. Dysphagia 1989, 4:48–52.
Martens L, Cameron T, Simonsen M: Effects of a multidisciplinary management program on neurologically impaired patients with dysphagia. Dysphagia 1990, 5:147–151.
Lerut T, Van Raemdonck D, Guelinckx P: Pharyngooesophageal diverticulum (Zenker’s). Clinical therapeutic and morphological aspects. Acta Gastroenterol Belg 1990, 53:330–337.
Mulder CJ, den Hartog G, Robijn RJ, Thies JE: Flexible endoscopic treatment of zenker’s diverticulum: a new approach. Endoscopy 1995, 27:438–442.
Cook RD, Huang PC, Richstmeier WJ, Scher RL: Endoscopic staple-assisted esophagodiverticulostomy: an excellent treatment of choice for Zenker’s diverticulum. Laryngoscope 2000, 110:2020–2025.
Wisdom G, Blitzer A: Surgical therapy for swallowing disorders. Otolaryngol Clin North Am 1998, 31:537–560.
Eibling DE, Snyderman CH, Eibling C: Laryngotracheal separation for intractable aspiration: a retrospective review of 34 patients. Laryngoscope 1995, 105:83–85.
Yamana T, Kitano H, Hanamitsu M, Kitajima K: Clinical outcome of laryngotracheal separation for intractable aspiration pneumonia. J Oto-Rhino-Laryngol Related Specialties 2001, 63:321–324.
Haapaniemi JJ, Laurikainen EA, Pulkkinen J, Marttila RJ: Botulinum toxin in the treatment of cricopharyngeal dysphagia. Dysphagia 2001, 16:171–175.
Thomas M, Haigh RA: Dysphagia, a reversible cause not to be forgotten. Postgrad Med J 1995, 71:94–95.
Fonda D, Schwarz J, Clinnick S: Parkinsonian medication one hour before meals improves symptomatic swallowing: a case study. Dysphagia 1995, 10:165–166.
Deane KH, Whurr R, Clarke CE, et al.: Non-pharmacological therapies for dysphagia in Parkinson’s disease (Cochrane review). Cochrane Database of Systematic Reviews. 2002, 2:CD002816. Evidence-based review of swallow therapy in Parkinson’s disease.
Dalakas MC, Illa I, Dambrosia JM, et al.: A controlled trial of high dose intravenous immune globulin infusions as treatment of dermatomyositis. N Engl J Med 1993, 329:1993–2000.
Williams RB, Grehan MJ, Hersch M, et al.: Biomechanics, diagnosis, and treatment outcome in inflammatory myopathy presenting as oropharyngeal dysphagia. Gut 2003, in press. Thorough evaluation of dysphagia in a population with inflammatory myopathy
Darrow DH, Hoffman GT, Barnes GJ, Wiley CA: Management of dysphagia in inclusion body myositis. Arch Otolaryngol Head Neck Surg 1992, 118:313–317.
Kluin KJ, Bromberg MB, Feldman EL, Simmons Z: Dysphagia in elderly men with myasthenia gravis. J Neurol Sci 1996, 138:49–52.
Branski D, Levy J, Globus M, et al.: Dysphagia as a primary manifestation of hyperthyroidism. J Clin Gastroenterol 1984, 6:437–440.
Bhatia KP, Munchau A, Brown P: Botulinum toxin is a useful treatment in excessive drooling in saliva [letter]. J Neurol Neurosurg Psychiatry 1999, 67:697.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Cook, I.J. Treatment of oropharyngeal dysphagia. Curr Treat Options Gastro 6, 273–281 (2003). https://doi.org/10.1007/s11938-003-0019-4
Issue Date:
DOI: https://doi.org/10.1007/s11938-003-0019-4