Abstract
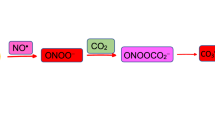
Porphyrias are inherited and acquired diseases of erythroid or hepatic origin, in which there are defects in specific enzymes of the heme biosynthetic pathway. In patients with intermittent acute porphyria and lead poisoning the erythrocytic activities of superoxide dismutase and glutathione peroxidase are reported to be increased. Our studies demonstrated that d-aminolevulinic acid, a heme precursor accumulated in both diseases, undergoes enolization at pH < 7.0 before it autoxidizes. The autoxidation of d-aminolevulinic acid, in the presence or absence of oxyhemoglobin has been proposed as a source of oxy and carbon-centred radicals in the cells of intermittent acute porphyria and saturnism carriers. Thus, the increased levels of antioxidant enzymes can be viewed as an intracellular response against the deleterious effects of these extremely reactive species.
Similar content being viewed by others
References
Halliwell B, Gutteridge JMC: Oxygen toxicity, oxygen radicals, transition metals and disease. Biochem J 219: 1–14, 1984
Halliwell B, Gutteridge JMC: The importance of free radicals and catalytic metal ions in human diseases. Mol Aspects Med 8: 89–193, 1985
Hammond B, Kontos HA, Hess ML: Oxygen radicals in the adult respiratory distress syndrome, in myocardial ischemia and reperfusion injury, and in cerebral vascular damage. Can J Physiol Pharmacol 63: 173–187, 1985
Cross CE, Halliwell B, Borish ET, Pryor WA, Ames BN, Saul RL, McCord JM, Harman D: Oxygen Radicals and Human Disease. Ann Intern Med 107: 526–545, 1987
Ribarov SR, Benov LC, Benchev IC: The effect of lead on hemoglobin-catalyzed lipid peroxidation. Biochim Biophys Acta 664: 453–459, 1981
Ito Y, Murai Y, Niiya Y, Nagao F, Aritaki M, Koide T, Kanosi Y, Otani M, Shima S, Sarai S: Studies on Serum Lipid Peroxides and Superoxide Dismutase Activities of Workers Exposed to Lead. J Science of Labour 60: 53–64, 1984
Ito Y, Niigya Y, Kurita H, Shima S, Sarai S: Serum Lipid Peroxide Level and Blood Superoxide Dismutase Activity in Workers with Occupational Exposure to Lead. Int Arch Occup Environ Health 56: 119–128, 1985
Medeiros MHG, Marchiori PE, Bechara EJH: Superoxide Dismutase, Glutathione Peroxidase and Catalase Activities in the Erythrocytes of Patients with Intermittent Acute Porphyria. Clin Chem 28: 242–243, 1982
Monteiro HP, Abdalla DSP, Arcuri ASA, Bechara EJH: Oxygen Toxicity Related to Exposure to Lead. Clin Chem 31:1673–1676, 1985
Hindmarsh JT: The porphyrias: Recent Advances. Clin Chem 32: 1255–1263, 1986
Farant JP, Wigfield DC: Biomonitoring lead exposure with delta-aminolevulinate dehydratase (ALA-D) activity ratios. Int Arch Occup Environ Health 51: 15–24, 1982
McGillion FB, Thompson GG, Goldberg A: Tissue uptake of d-aminolevulinic acid. Biochem Pharmacol 24: 299–301, 1975
Schreiber WE: Iron, porphyrin, and bilirubin metabolism. In: Kaplan LA, Pesce AJ (eds) Clinical Chemistry-Theory, Analysis and Correlation. The C.V. Mosby Company, St. Louis, 1989, pp 496–511
Marsh DO: The neurotoxicity of mercury and lead. In: O'Donoghue JL (ed) Neurotoxicity of Industrial and Commercial Chemicals. Vol 1, CRC Press, Boca Raton, Florida, 1985, pp 159–169
Monteiro HP, Abdalla DSP, Alario AF, Bechara EJH: Generation of Active Oxygen Species During Coupled Autoxidation of Oxyhemoglobin and d-aminolevulinic Acid. Biochim Biophys Acta 881: 100–106, 1986
Monteiro HP, Abdalla DSP, Augusto O, Bechara EJH: Free Radical Generation during d-aminolevulinic acid autoxidation: induction by hemoglobin and connections with porphyrinpathies. Arch Biochem Biophys 271: 206–216, 1989
Fridovich I: Superoxide dismutase in biology and medicine. In: Autor A (ed) Pathology of Oxygen. New York, Academic Press, 1982, pp 1–20
Fridovich I: Superoxide Radical: An endogenous toxicant. Ann Rev Pharmacol Toxicol 23: 239–257, 1983
Halliwell B, Gutteridge JMC: Oxygen Free Radicals and iron in relation to biology and medicine: some problems and concepts. Arch Biochem Biophys 246: 501–514, 1986
Cadenas E: Biochemistry of Oxygen Toxicity. Ann Rev Biochem 58: 79–110, 1989
Sies H: Biochemistry of oxidative stress. Angew Chem Int Ed Engl 25: 1058–1071, 1986
Fridovich I: Oxygen tocicity in prokaryotes: the importance of superoxide dismutase. In: Oberley LW (ed) Superoxide Dismutase. Vol I. Florida, CRC Press, Boca Raton 1982, pp 79–88
Privalle CT, Gregory EM: Superoxide dismutase and O2 lethality in bacteroides fragilis. J Bacteriol 138: 139–145, 1979
Gregory EM, Fridovich J: Induction of superoxide dismutase by molecular oxygen. J Bacteriol 114: 543–548, 1973
Gregory EM, Goscin SA, Fridovich I: Superoxide dismutase and oxygen toxicity in a eukaryote. J Bacteriol 117: 456–460, 1974
Hassan HM, Fridovich I: Enzymatic defences against the toxicity of oxygen and of streptonigrin in Escherichia coli. J Bacteriol 129: 1574–1583, 1977
Hassan HM, Fridovich I: Regulation of superoxide dismutase synthesis in Escherichia coli. J Biol Chem 252: 7667–7672, 1977
Stevens JB, Autor AP: Induction of superoxyde dismutase by oxygen in neonatal rat lung. J Biol Chem 252: 3509–3514, 1977
Housset B, Junod AF: Effects of culture conditions and hyperoxia and antioxidant enzymes in pig pulmonary artery and aortic endothelium. Biochim Biophys Acta 716: 283–289, 1982
Frank L: Effects of oxygen on the newborn. Federation Proc 44: 2328–2334, 1985
Finn GJ, Condon S: Regulation of catalase synthesis in Salmonella typhimurium. J Bacteriol 123: 570–579, 1975
Richter HE, Loewen PC: Induction of catalase in Escherichia coli by ascorbic acid involves hydrogen peroxide. Biochem Biophys Res Commun 100: 1039–1046, 1981
Crapo JD, Tierney DF: Superoxide dismutase and pulmonary oxygen toxicity. Am J Physiol 226: 1401–1407, 1974
Bhuian KC, Bhuian DK: Mechanism of cataractogenesis induced by 3-amino-1H-1,2,4-Triazole II: Superoxide dismutase of the eye and its role in protecting the ocular lens from oxidative damage by endogenous O2-, H202 and/or-OH. In: Caughey WS (ed) Biochemical and Clinical Aspects of Oxygen. Academic Press, New York. 1979, pp 797–807
Mavelli T, Ciriolo MR, Rotilio G, de Sole P, Castorino M, Stabile A: Superoxyde dismutase, glutathione peroxidase and catalase, in oxidative hemolysis. A study of Fanconi's anemia erythrocytes. Biochem Biophys Res Commun 106: 286–290, 1982
Abdalla DSP, Monteiro HP, Oliveira JAC, Bechara EJH: Activities of superoxide dismutase and glutathione peroxidase in schizophrenic and manic-depressive patients. Clin Chem 32: 805–807, 1986
Murphy MJ, Kehrer JP: Activities of antioxidant enzymes in muscle, liver and lung of chickens with inherited muscular distrophy. Biochem Biophys Res Commun 134: 550–556, 1986
Stocker R, Hunt NH, Weidemann MJ: Antioxidants in plasma from mice infected with Plasmodium, Vinkei. Biochem Biophys Res Commun 134: 152–158, 2q 1986
Kappas A, Sassa S, Anderson KE: The porphyrias. In: Stanbury JB, Wyngaarden JB, Frederickson DS, Goldstein JL, Brown MS (eds) Metabolic Basis of Inherited Diseases. McGraw Hill, New York, 1983, pp 1301–1384
Granick S: The induction in vitro of the synthesis of daminolevulinic acid synthetase in chemical porphyria: A response to certain drugs, sex hormones, and foreign chemicals. J Biol Chem 241: 1359–1375, 1966
Marver HS, Tschudy DP, Perlroth MG, Collins A: d-aminolevulinic acid synthetase. I. Studies in liver homogenates. J Biol Chem 241: 2803–2809, 1966
Marver HS, Collins A, Tschudy DP, Rechcigl M Jr: d-aminolevulinic acid synthetase. II. Induction in rat liver. J Biol Chem 241: 4323–4329, 1966
Strand LJ, Flesher BF, Redeker AG, Marver HS: Enzymatic abnormality in heme biosynthesis in acute intermittent porphyrias: Decreased hepatic conversion of porphobilinogen to porphyrins and increased d-aminolevulinic acid synthetase activity. Proc Natl Acad Sci USA 67: 1315–1320, 1970
McIntyre N, Pearson AJG, Allan DJ, Craske S, West GML, Moore MR, Beattie AD, Paxton J, Goldberg A: Hepatic d-aminolevulinic acid synthetase in an attack of hereditary coproporphyria and during remission. Lancet i: 560–564, 1971
Dowdle EB, Mustard P, Eales L: d-aminolevulinic acid synthetase activity in normal and porphyric human livers. S Afr Med J 41: 1093–1096, 1967
Pirolla BA, Borthwick IA, Srivastava G, May BK, Elliot WH: Effect of lead ions on chick embryo liver mitochondrial d-aminolevulinic acid synthase. Biochem J 222: 627–630, 1984
Sassa S, Urabe A: Uroporphyrinogen I synthase induction in normal human bone marrow cultures: An early and quantitative response of erythroid differentiation. Proc Natl Acid Sci USA 76: 5321–5325, 1979
Rose J, Ikawa Y, Leder P: Globin messenger RNA induction during erythroid differentiation of cultured leukemia cells. Proc Natl Acad Sci USA 69: 3620–3624, 1972
Granick JL, Sassa S, Granick S, Levere RD, Kappas A: Studies in lead poisoning. II. Correlations between the ratio of activated and inactivated d-aminolevulinic acid de hydratase of whole blood and the blood level. Biochem Med 8: 149–159, 1973
Doss M, Schneider J, von Tiepermann R, Brandt A: A new type of acute porphyria with porphobilinogen synthase (daminolevulinic acid dehydratase) defect in the homozygous state. Clin Biochem 15: 52–55, 1982
Romeo G, Levin EY: Uroporphyrinogen III co-synthetase in human congenital erythropoietic porphyria. Proc Natl Acad Sci USA 63: 856–863, 1969
Wada O, Yano Y, Tokoyama K, Suzuki T, Suzuki S, Katsununa H: Human Responses to Lead. In: Special References to Porphyrin Metabolism in Bone Marrow Erythroid Cells, a Clinical and Laboratory Study. Ind Health 10: 84–92, 1972
Bloomer JR, Ebert PS, Mahoney MJ: Study of factors causing excess protoporphyrin accumulation in cultured skin fibroblasts from patients with protoporphyria. J Clin Invest 60: 1354–1361, 1977
Bottomley SS, Tanaka M, Everett MA: Diminished erythroid ferrochelatase activity in protoporphyria. J Lab Clin Med 86: 126–131, 1975
Kinington C, Magnus IA, Ryan EA, Dripps DJ:Porphyria and photosensitivity. Quart. J Med 36: 29–57, 1967
Meyer-Betz F: Studies on the biological (photodynamic) action of haematoporphyrins and other derivatives of the blood and bile pigments. Deutsch Arch Klin Med 112: 476–503, 1913
Goldstein BD, Harber LC: Erythropoietic protoporphyria: Lipid peroxidation and red cell membrane damage associated with photohemolysis. J Clin Invest 51: 892–902, 1972
Bonnett R: Oxygen activation and tetrapyroles. In: Campbell PN, Marshall RD (eds) Essays in Biochemistry. Vol 17. Academic Press, London, 1981, pp 1–51
Spikes JD: Porphyrins and related compounds as photodynamic sensitizers. Ann NY Acad Sci 244: 496–508, 1975
Bodaness RS, Chan PC: Singlet oxygen as a mediator in the hematoporphyrin-catalyzed photooxidation of NADPH to NADP+ in deuterium oxide. J Biol Chem 252: 8554–8560, 1977
Sandberg S, Romslo I: Porphyrin induced photodamage at the cellular and the subcellular level as related to the solubility of the porphyrin. Clin Chim Acta 109: 193–201, 1981
De Goeiji AFPM, Van Steveninck J: Photodynamic effects of protoporphyrin on cholesterol and insaturated fatty acids in erythrocyte membranes in protoporphyria and in normal red blood cells. Clin Chim Acta 68: 115–122, 1976
Matheson IBC, Etheridge RD, Kratovich NR, Lee J: The quenching of singlet oxygen by amino acids and proteins. Photochem Photobiol 21: 165–172, 1975
Schothorst AA, Van Steveninck J, WentLN, Summond D: Photodynamic damage of the erythrocyte membrane caused by protoporphyrin in protoporphyria and in normal red blood cells. Clin Chim Acta 39: 161–170, 1972
Buettner GR, Oberley LW: The apparent production of superoxyde and hydroxyl radicals in hematoporphyrin and light as seen by spintrapping. FEBS Lett 121: 161–164, 1980
Morehouse KM, Moreno SNJ, Mason RP: The one-electron reduction of Uroporphyrin I by rat hepatic microsomes. Arch Biochem Biophys 257: 275–284, 1987
Bloomer JR, Bonkovsky HL: The porphyrias. Dis Mon 35: 1–54, 1989
Cutler MG, Moore MR, Dick JM:Effects of d-aminolevulinic acid on contractile activity of rabbit duodenum. Eur J Pharmacol 64: 221–230, 1984
Becker D, Viljoen D, Kramer S: The inhibition of red cell and brain ATPase by d-aminolevulinic acid. Biochim Biophys Acta 225: 26–34, 1971
Russell VA, Lamm MCL, Taljaard JJF: Inhibition of sodium potassium ATPase activity by Delta-aminolevulinic acid. Neurochem Res 8: 1407–1416, 1983
Dhawan M, Flora SJ, Tandon SK: Preventive and therapeutic role of vitamin E in chronic plumbism. Biomed Environ Sci 2: 335–340, 1989
Brennan MJW, Cantrill RC, Kramer S: Effect of d-aminolevulinic acid on GABA receptor binding in synaptic plasma membranes. Int J Biochem 12: 833–835, 1980
Debler EA, Sershen H, Lajtha A, Gennaro JF Jr: Superoxide radical-mediated alteration of synaptosome membrane structure and high-affinity [14C] gamma-aminobutyric acid uptake. J Neurochem 47: 1804–1813, 1986
Demopoulos HB, Flamm E, Seligman M, Pietronigro DD: Oxygen free radicals in central nervous system ischemia and trauma. In: Autor A (ed) Pathology of Oxygen. Academic Press, New York, 1982, pp 127–155
Colton CA, Fagni L, Gilbert D: The action of hydrogen peroxide on paired pulse and long-term potentiation in the hippocampus. Free Rad Biol Med 7: 3–8, 1989
Bonkovsky HL, Schady W: Neurologic manifestation of acute porphyria. Semin Liver Dis 2: 108–124, 1982
Thornalley PJ, Wolff S, Crabbe J, Stern A: The autoxidation of glyceraldehyde and other simple monosaccharides under physiological conditions catalyzed by buffer ions. Biochim Biophys Acta 794: 276–287, 1984
Thornalley PJ, Stern A: The production of free radicals during the autoxidation of monosaccharides by buffer ions. Carbohyd Res 134: 191–204, 1984
Buettner GR: Spin trapping: ESR parameters of spin adducts. Free Radical Biol Med 3: 259–303, 1987
Medeiros MHG, Bechara EJH: Chemiluminescent aerobic oxidation of protein adducts with glycolaldehyde catalysed by horseradish peroxidase. Arch Biochem Biophys 248: 433–439, 1986
Goyer RA: Toxic Effects of Metals. In: Klaassen CD, Amdur MO, Doull J (eds) Toxicology the basic science of poisons. Macmillan Publishing Co, New York, 1986, pp 582–635
Hasan J, Vihko V, Henberg S: Deficient red cell membrane (Na+/K+(ATPase in lead poisoning. Arch Environ Health 14: 313–324, 1967
Levander OA, Morris VC, Higgs DJ, Ferreti RJ: Lead poisoning in vitamin E-deficient rats. J Nutr 105: 1481–1485, 1975
Ribarov SR, Bochev P: Lead-hemoglobin interaction as a possible source of reactive oxygen apecies — a chemiluminescent study. Arch Biochem Biophys 213: 288–292, 1982
Castro CE, Wade RA, Belser NO: Conversion of oxyhemoglobin to methemoglobin by organic and inorganic reductants. Biochemistry 17: 225–231, 1978
Kawanishi S, Caughey WS: Aquopentacyanoferrate (11): An effective probing electron donor in the conversion of oxyhemoglobin to methemoglobin and peroxide. Biochem Biophys Res Commun 88: 1203–1208, 1979
Winterbourn CC: Free radical production and oxidative reactions of hemoglobin. Environ Health Persp 64: 321–330, 1985
Wallace WJ, Houtchens RA, Maxwell JC, Caughey WS: Mechanism of autoxidation of hemoglobins and myoglobins promotion of superoxide production by protons and anions. J Biol Chem 257: 4966–4977, 1982
Bates DA, Winterbourn CC: Reactions of adriamycin with haemoglobin. Biochem J 203: 105–110, 1982
Winterbourn CC: The reaction of hemoglobin with paraquat radicals in the presence and absence of oxygen. Biochem Internatl 7: 1–8, 1983
Dershwitz M, Novak RF: Generation of superoxide via the interaction of nitrofurantoin with oxyhemoglobin. J Biol Chem 257: 75–79, 1982
Goldberg B, Stern A: Production of superoxyde anion during the oxidation of hemoglobin by menadione. Biochim Biophys Acta 437: 628–632, 1976
Thornalley PJ, Wolff SP, Crabbe MJC, Stern A: The oxidation of oxyhaemoglobin by glyceraldehyde and other simple monosaccharides. Biochem J 217: 615–622, 1984
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Monteiro, H.P., Bechara, E.J.H. & Abdalla, D.S.P. Free radicals involvement in neurological porphyrias and lead poisoning. Mol Cell Biochem 103, 73–83 (1991). https://doi.org/10.1007/BF00229595
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00229595